Blood Sugar and Inflammation
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction: The Hidden Link Between Glucose and Chronic Inflammation
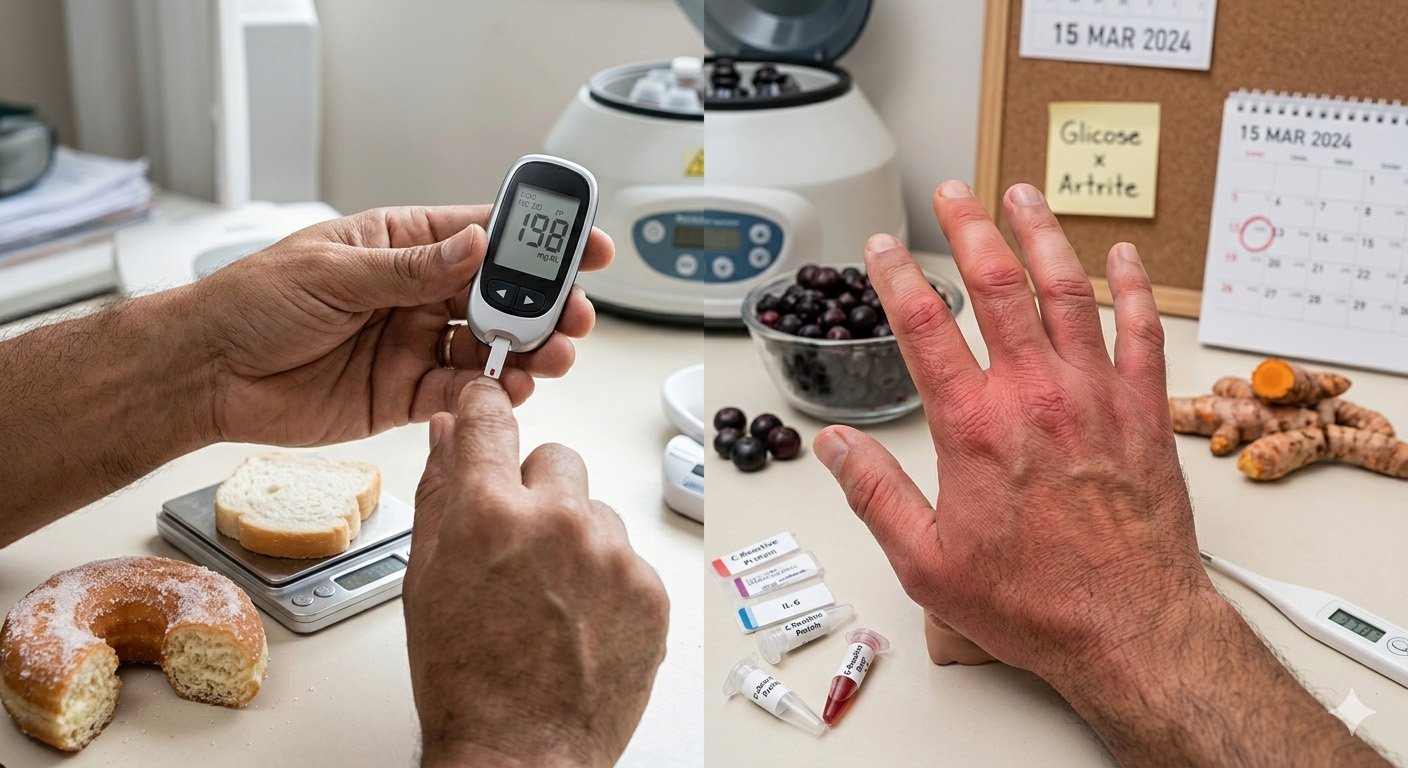
Blood sugar and inflammation are closely connected biological processes that influence nearly every system in the body. When blood sugar levels remain stable, the body maintains metabolic balance and healthy immune function. However, frequent spikes or chronically elevated glucose can trigger inflammatory responses that contribute to fatigue, weight gain, cardiovascular disease, and metabolic disorders.
This relationship connects directly to Metabolism, Hormone Health, and Nutrition, as well as immune regulation, gut function, and cardiovascular health. In recent years, researchers have identified chronic inflammation as a key mechanism linking high blood sugar to long-term diseases such as type 2 diabetes and heart disease.
Understanding how blood sugar influences inflammation helps explain why managing glucose levels is not just about energy—it is also about protecting long-term health.
What Is Inflammation and How Does It Relate to Blood Sugar?
Inflammation is the body’s natural defense response to injury, infection, or stress. In the short term, inflammation helps protect tissues and support healing. However, when inflammation becomes chronic, it can damage cells and disrupt normal metabolic function.
Blood sugar plays a major role in this process.
Healthy blood sugar regulation typically supports:
- Balanced immune response
- Normal tissue repair
- Stable energy levels
- Healthy metabolism
Poor blood sugar control can lead to:
- Persistent low-grade inflammation
- Oxidative stress
- Insulin resistance
- Tissue damage
This connection makes blood sugar regulation central to both Blood Sugar management and long-term Heart Health.
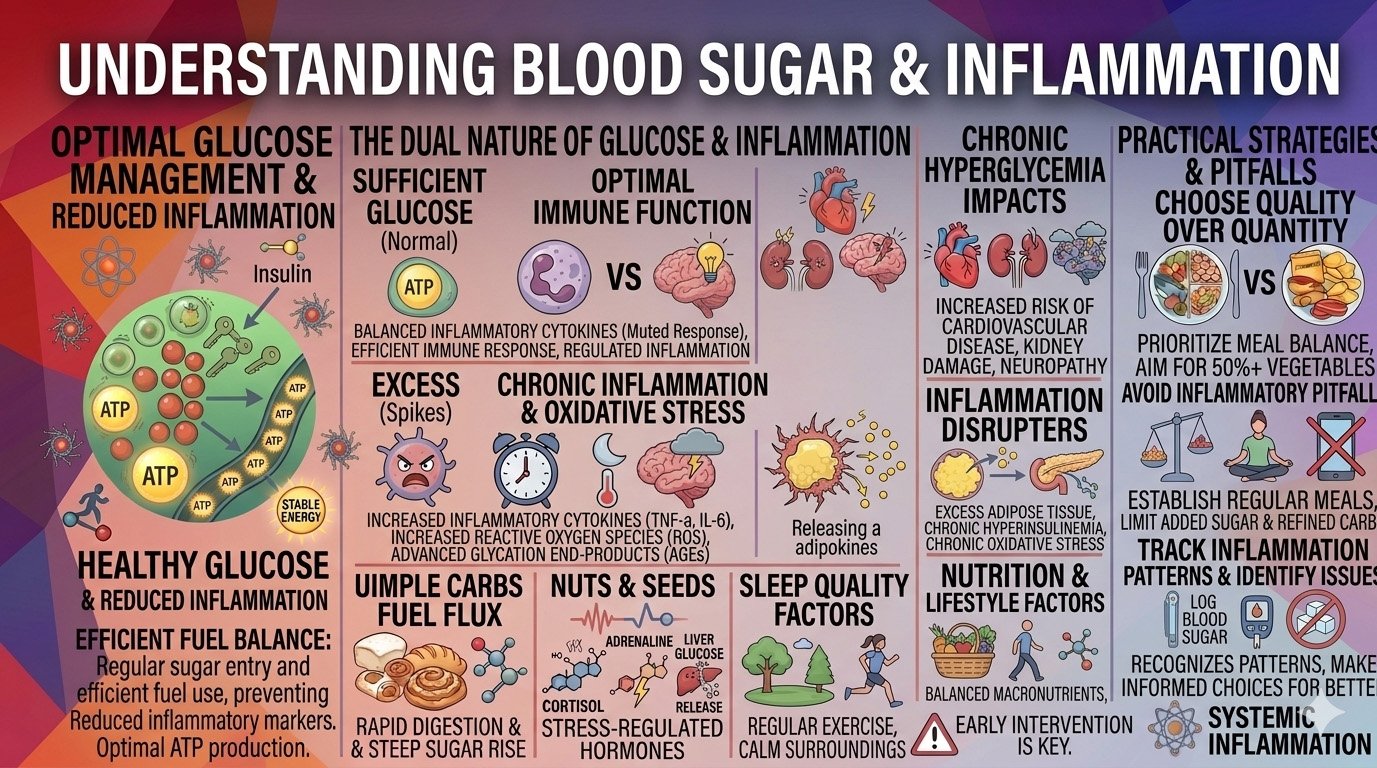
How High Blood Sugar Triggers Inflammation (Physiology)
Elevated glucose levels activate several biological pathways that increase inflammation throughout the body.
1) Oxidative Stress and Cellular Damage
When blood sugar levels are high, cells produce excess reactive molecules known as free radicals.
These molecules can:
- Damage cell membranes
- Disrupt normal metabolism
- Trigger inflammatory responses
- Accelerate aging processes
Oxidative stress is one of the primary mechanisms linking high blood sugar to chronic disease.
2) Advanced Glycation End Products (AGEs)
High glucose levels can cause sugar molecules to attach to proteins and fats, forming compounds called advanced glycation end products (AGEs).
AGEs can:
- Promote inflammation
- Damage blood vessels
- Impair tissue repair
- Increase disease risk
This process is strongly associated with cardiovascular disease and metabolic dysfunction, highlighting the connection between glucose control and Heart Health.
3) Insulin Resistance and Inflammatory Signals
Chronic inflammation can make cells less responsive to insulin.
This creates a cycle:
High blood sugar → Inflammation → Insulin resistance → Higher blood sugar
This feedback loop is a central feature of metabolic disease and is closely tied to Metabolism and long-term glucose regulation.
4) Gut Health and Immune Activation
The digestive system plays a critical role in inflammation.
Unstable blood sugar can disrupt gut bacteria balance, leading to:
- Increased intestinal permeability
- Immune activation
- Systemic inflammation
This mechanism explains why Gut Health is closely linked to both metabolic health and inflammation.
Common Signs of Blood Sugar-Related Inflammation
Chronic inflammation often develops gradually and may not produce obvious symptoms at first.
Common signs include:
- Persistent fatigue
- Brain fog
- Joint pain
- Frequent infections
- Slow wound healing
- Digestive discomfort
- Weight gain
These symptoms frequently overlap with issues in Energy & Fatigue regulation.
Conditions Associated With Blood Sugar and Inflammation
Long-term glucose instability and chronic inflammation are associated with several major health conditions.
Insulin Resistance
A condition where cells respond poorly to insulin.
Inflammation contributes to:
- Reduced insulin sensitivity
- Elevated blood sugar
- Increased fat storage
- Metabolic imbalance
This condition is closely linked to Weight Loss challenges and metabolic dysfunction.
Type 2 Diabetes
Chronic high blood sugar promotes inflammatory damage in blood vessels and tissues.
Common complications include:
- Nerve damage
- Kidney disease
- Vision problems
- Cardiovascular disease
Inflammation is now recognized as a central driver of diabetes progression.
Cardiovascular Disease
Inflammation and high blood sugar can damage blood vessels and increase plaque formation.
Risk factors include:
- Hypertension
- Atherosclerosis
- Heart attack
- Stroke
This relationship highlights the importance of protecting Heart Health through stable glucose control.
Metabolic Syndrome
A cluster of conditions including:
- High blood sugar
- High blood pressure
- Excess body fat
- Abnormal cholesterol levels
Chronic inflammation is a defining feature of metabolic syndrome and is strongly linked to Metabolism.
Lifestyle Factors That Influence Blood Sugar and Inflammation
Several daily habits can either increase or reduce inflammation.
Diet Quality
Diet is one of the strongest drivers of inflammation.
Foods associated with increased inflammation:
- Sugary beverages
- Refined carbohydrates
- Ultra-processed foods
- Excess saturated fats
Foods associated with reduced inflammation:
- Vegetables
- Whole grains
- Nuts and seeds
- Fatty fish
- Olive oil
Healthy eating patterns are central to Nutrition and metabolic health.
Sleep
Poor sleep can increase inflammatory markers and disrupt glucose regulation.
Sleep deprivation can lead to:
- Elevated cortisol
- Increased blood sugar
- Increased inflammation
This connection highlights the importance of Sleep Health in metabolic regulation.
Physical Activity
Regular movement reduces inflammation and improves insulin sensitivity.
Exercise helps:
- Lower blood sugar
- Improve metabolism
- Reduce inflammatory signals
- Support immune function
Physical activity is a core component of both Metabolism and long-term health.
Chronic Stress
Stress increases cortisol levels, which can raise blood sugar and trigger inflammation.
Managing stress supports:
- Hormonal balance
- Stable glucose levels
- Reduced inflammation
This connection underscores the role of Hormone Health.
Practical Strategies to Reduce Inflammation Through Blood Sugar Control
These evidence-based strategies help stabilize glucose and reduce inflammatory risk.
Focus on Stable Blood Sugar
Helpful habits include:
- Eating balanced meals
- Limiting refined carbohydrates
- Avoiding sugary drinks
- Monitoring portion sizes
Stable glucose levels reduce inflammatory signals.
Increase Fiber Intake
Fiber helps:
- Slow glucose absorption
- Improve gut health
- Reduce inflammation
High-fiber diets are consistently associated with better metabolic outcomes.
Maintain Healthy Body Weight
Excess body fat can increase inflammatory signals.
Weight management supports:
- Insulin sensitivity
- Reduced inflammation
- Better metabolic health
This is closely linked to Weight Loss and long-term disease prevention.
Stay Physically Active
Even moderate activity can significantly reduce inflammation.
Examples:
- Walking
- Resistance training
- Cycling
- Swimming
Prioritize Sleep and Stress Management
Healthy sleep and stress control are essential for reducing inflammation and stabilizing blood sugar.
Why the Blood Sugar–Inflammation Connection Matters
Chronic inflammation is now recognized as a major driver of modern disease.
When blood sugar remains unstable, inflammation can develop silently and gradually.
Over time, this process can contribute to:
- Insulin resistance
- Diabetes
- Heart disease
- Fatigue
- Accelerated aging
- Metabolic dysfunction
Maintaining stable blood sugar is one of the most effective ways to protect long-term health.
Final Thoughts: Blood Sugar Stability Protects More Than Energy
Blood sugar control is not just about preventing diabetes—it is about reducing inflammation throughout the body.
Stable glucose supports:
- Healthy immune function
- Balanced metabolism
- Cardiovascular health
- Sustained energy
- Reduced disease risk
Understanding the relationship between Blood Sugar, Inflammation, Metabolism, Nutrition, and Hormone Health provides a practical foundation for improving both daily well-being and long-term health.
FAQ
Can high blood sugar cause inflammation?
Yes. Elevated blood sugar can trigger inflammatory responses through oxidative stress and immune activation.
Does inflammation increase blood sugar?
Yes. Inflammation can reduce insulin sensitivity, making it harder for cells to use glucose effectively.
Can lowering blood sugar reduce inflammation?
Yes. Improving blood sugar control is one of the most effective ways to reduce chronic inflammation.
What foods reduce inflammation and support blood sugar control?
Foods rich in fiber, healthy fats, and antioxidants—such as vegetables, whole grains, nuts, and fatty fish—are consistently associated with reduced inflammation.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
Inflammation and Diabetes
American Diabetes Association (ADA)
Inflammation and Blood Glucose
Centers for Disease Control and Prevention (CDC)
Hotamisligil GS
Inflammation and Metabolic Disorders
Nature
Pradhan AD et al.
Inflammatory Biomarkers and Risk of Type 2 Diabetes
Journal of the American Medical Association (JAMA)
Donath MY, Shoelson SE
Type 2 Diabetes as an Inflammatory Disease
Nature Reviews Immunology
