Fasting Blood Sugar Explained
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction
Fasting blood sugar is one of the most widely used indicators of metabolic health. It reflects how the body regulates glucose during periods without food, typically overnight. Because fasting glucose depends heavily on hormone balance, liver function, and insulin sensitivity, it provides valuable insight into early metabolic dysfunction.
Abnormal fasting blood sugar levels are often among the first measurable signs of insulin resistance and developing diabetes. Even small elevations can signal changes in Metabolism, shifts in Hormone Health, and disruptions in energy regulation. Fasting glucose is also closely connected to Nutrition, Sleep Health, and long-term cardiovascular risk.
Understanding fasting blood sugar helps individuals and clinicians detect problems early, monitor metabolic stability, and prevent chronic disease.
What Is Fasting Blood Sugar?
Fasting blood sugar refers to the level of glucose in the bloodstream after a period without eating, usually 8 to 12 hours.
This measurement reflects how the body maintains glucose balance when food is not actively supplying energy.
Typical testing conditions:
- No food for 8–12 hours
- Water allowed
- Usually measured in the morning
- Performed through a blood test
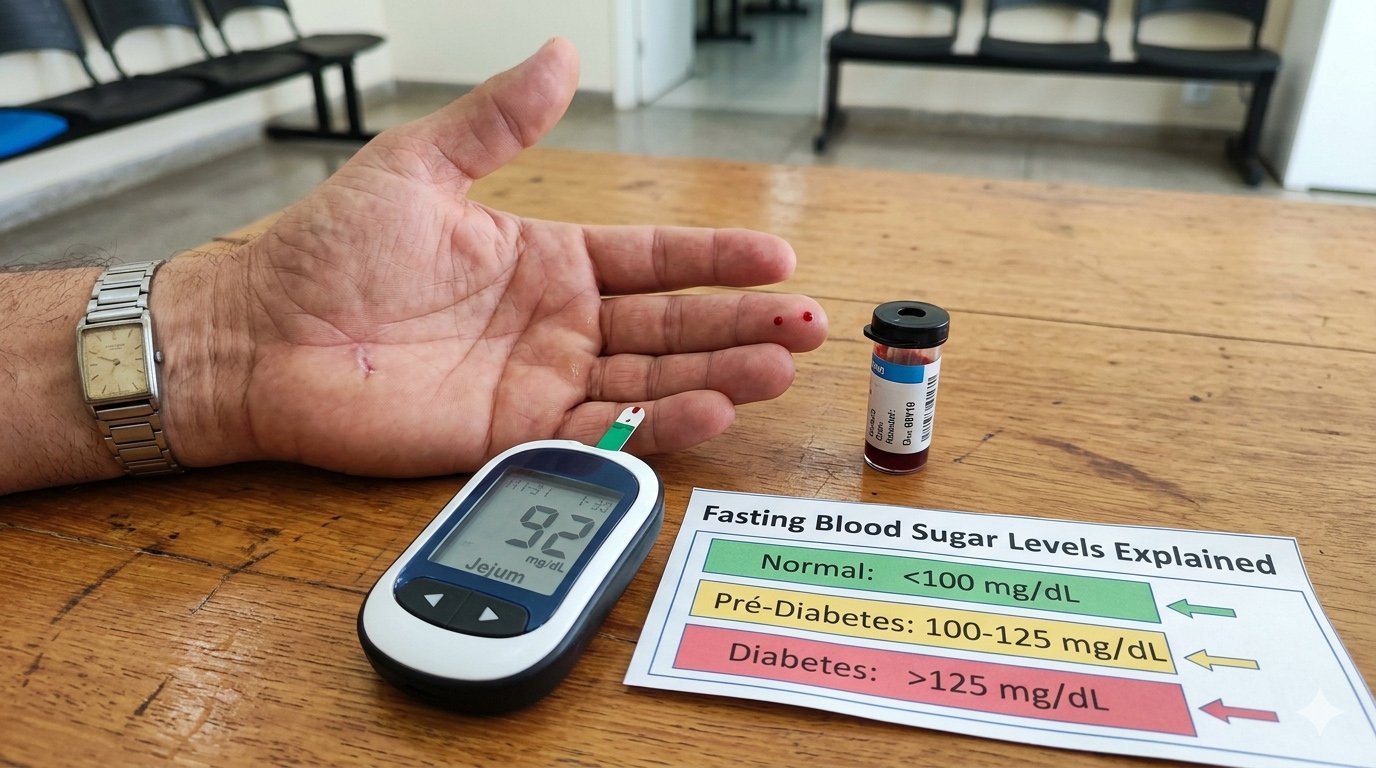
Clinical reference ranges:
- Normal: 70–99 mg/dL
- Prediabetes: 100–125 mg/dL
- Diabetes: 126 mg/dL or higher
These thresholds are widely used by medical organizations to assess Blood Sugar control and metabolic health.
How Fasting Blood Sugar Works (Physiology)
During fasting, the body must maintain a stable supply of glucose even without food intake. This process relies primarily on the liver and hormone regulation.
The body maintains fasting glucose through:
- Glycogen breakdown in the liver
- Glucose production (gluconeogenesis)
- Hormonal regulation
Key hormones involved include:
- Insulin
- Glucagon
- Cortisol
- Growth hormone
In healthy individuals:
- The liver releases small amounts of glucose
- Insulin regulates blood sugar levels
- Glucose remains stable throughout the night
When this system becomes impaired:
- The liver releases too much glucose
- Insulin becomes less effective
- Fasting blood sugar rises
These changes are central to dysfunction in Metabolism and disruptions in Hormone Health.
Why Fasting Blood Sugar Rises
Elevated fasting blood sugar is usually caused by underlying metabolic or hormonal factors rather than recent food intake.
1) Insulin Resistance
Insulin resistance is the most common cause of high fasting glucose.
When cells become resistant to insulin:
- The liver releases more glucose
- Insulin becomes less effective
- Blood sugar remains elevated overnight
This condition is strongly linked to Metabolism and long-term changes in Weight Loss patterns.
2) The Dawn Phenomenon
The dawn phenomenon is a natural early-morning rise in blood sugar caused by hormone release.
These hormones include:
- Cortisol
- Growth hormone
- Glucagon
They increase glucose production to prepare the body for waking and activity.
In people with insulin resistance, this response can lead to elevated fasting glucose.
This mechanism highlights the connection between fasting blood sugar and Hormone Health.
3) Poor Sleep
Sleep plays a critical role in glucose regulation.
Sleep deprivation can:
- Increase insulin resistance
- Raise stress hormone levels
- Elevate fasting blood sugar
Optimizing Sleep Health helps stabilize overnight glucose levels.
4) Late-Night Eating
Eating large meals late in the evening can affect fasting glucose the next morning.
Common effects include:
- Delayed digestion
- Increased glucose production
- Reduced insulin sensitivity
This connection reinforces the importance of balanced Nutrition and meal timing.
5) Stress and Cortisol
Chronic stress increases cortisol, a hormone that raises blood sugar.
Elevated cortisol can:
- Stimulate glucose production
- Reduce insulin sensitivity
- Increase fasting glucose levels
This relationship highlights the role of Hormone Health in metabolic regulation.

Symptoms of High Fasting Blood Sugar
Mild elevations in fasting glucose may not cause noticeable symptoms. However, persistent increases can produce signs associated with hyperglycemia.
Common symptoms include:
- Morning fatigue
- Increased thirst
- Frequent urination
- Headaches
- Blurred vision
- Brain fog
- Increased hunger
These symptoms often overlap with issues discussed in Energy & Fatigue and long-term Blood Sugar instability.
Health Risks of Elevated Fasting Blood Sugar
Chronically high fasting glucose is associated with increased risk of metabolic and cardiovascular disease.
Metabolic Risks
- Prediabetes
- Type 2 diabetes
- Metabolic syndrome
- Insulin resistance
- Weight gain
These conditions reflect impaired Metabolism and reduced insulin efficiency.
Cardiovascular Risks
Elevated fasting blood sugar contributes to vascular damage and inflammation.
Potential risks include:
- Atherosclerosis
- Hypertension
- Heart disease
- Stroke
This connection underscores the importance of monitoring fasting glucose for long-term Heart Health.
Energy and Cognitive Effects
Persistent high fasting blood sugar can affect brain function and daily performance.
Possible effects include:
- Low energy levels
- Difficulty concentrating
- Mood changes
- Reduced mental clarity
These symptoms are closely associated with Energy & Fatigue regulation.
How Fasting Blood Sugar Is Measured
Fasting blood sugar can be measured through several clinical methods.
Fasting Plasma Glucose (FPG) Test
This is the most common diagnostic test.
Characteristics:
- Performed after overnight fasting
- Simple blood test
- Widely used for diabetes screening
Hemoglobin A1C Test
The A1C test measures average blood sugar levels over approximately three months.
It helps:
- Diagnose diabetes
- Monitor long-term glucose control
- Assess treatment effectiveness
This test complements fasting glucose measurements within the broader Blood Sugar system.
Continuous Glucose Monitoring (CGM)
CGM devices provide continuous tracking of glucose levels.
They allow:
- Detection of overnight glucose patterns
- Identification of fasting spikes
- Improved glucose awareness
These tools support better management of Metabolism and daily energy balance.
Practical Strategies to Improve Fasting Blood Sugar
Evidence-based strategies can help stabilize fasting glucose and improve metabolic health.
Improve Evening Nutrition
Focus on:
- Balanced meals
- Moderate carbohydrate intake
- Fiber-rich foods
- Lean protein
Avoid:
- Large late-night meals
- Sugary snacks
- Refined carbohydrates
Healthy evening nutrition supports stable overnight Nutrition and glucose regulation.
Maintain Consistent Sleep Patterns
Regular sleep schedules help regulate hormone balance and glucose metabolism.
Benefits include:
- Improved insulin sensitivity
- Reduced stress hormone levels
- Better metabolic control
This reinforces the importance of Sleep Health.
Increase Physical Activity
Regular movement improves glucose use by muscles and enhances insulin sensitivity.
Benefits include:
- Lower fasting blood sugar
- Improved metabolic efficiency
- Reduced inflammation
This supports both Metabolism and sustainable Weight Loss.
Manage Stress
Reducing chronic stress helps regulate cortisol and glucose production.
Effective strategies include:
- Physical activity
- Relaxation techniques
- Structured routines
- Adequate recovery
These behaviors support long-term Hormone Health.
Why Fasting Blood Sugar Matters
Fasting blood sugar is one of the most important indicators of metabolic health because it reflects how the body regulates glucose without food intake.
It helps detect:
- Insulin resistance
- Early diabetes risk
- Hormonal imbalance
- Metabolic dysfunction
Because fasting glucose is easy to measure and highly predictive of long-term health outcomes, it is widely used in preventive medicine.
Monitoring fasting blood sugar helps protect:
- Metabolism
- Heart Health
- Energy levels
- Hormone balance
- Long-term health
Final Thoughts
Fasting blood sugar provides a clear window into metabolic function and hormone regulation. While temporary fluctuations are normal, persistent elevations may signal underlying metabolic stress and increased disease risk.
Maintaining healthy fasting glucose requires coordination between:
- Metabolism
- Nutrition
- Hormone Health
- Sleep Health
- Energy & Fatigue
- Heart Health
- Gut Health
- Weight Loss
Understanding fasting blood sugar empowers individuals to detect early metabolic changes and take proactive steps toward long-term health.
FAQ — Fasting Blood Sugar
What is a normal fasting blood sugar level?
Most guidelines define:
- 70–99 mg/dL as normal
- 100–125 mg/dL as prediabetes
- 126 mg/dL or higher as diabetes
How long should you fast before a blood sugar test?
Typically:
- 8 to 12 hours
Water is allowed, but food and caloric drinks should be avoided.
Can fasting blood sugar be high even if diet is healthy?
Yes. Elevated fasting glucose can result from:
- Insulin resistance
- Hormonal changes
- Poor sleep
- Stress
- Genetic factors
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Centers for Disease Control and Prevention (CDC)
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
American Diabetes Association (ADA)
World Health Organization (WHO)
American Heart Association — Blood Sugar and Cardiovascular Health
Nathan DM. “Diagnosis and Classification of Diabetes Mellitus.”
Diabetes Care
International Diabetes Federation — Global Diabetes Overview
