
The Basics of Epidemiology
Understanding Disease Patterns, Population Health, and the Science Behind Prevention
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Epidemiology is the scientific foundation of public health. It provides the tools to understand how diseases spread, why they occur, who is most at risk, and how societies can prevent illness before it becomes a crisis. From infectious outbreaks to chronic diseases, environmental hazards, and mental health trends, epidemiology connects data, biology, behavior, and policy into a unified framework for protecting populations.
In modern public health systems, epidemiology functions as both an early warning system and a strategic planning tool. It informs vaccination programs, sanitation policies, disease surveillance, and emergency responses. It also shapes long-term prevention strategies, identifying patterns that would otherwise remain invisible.
Understanding the basics of epidemiology is essential not only for scientists and policymakers but also for healthcare professionals, educators, journalists, and informed citizens. In an interconnected world where diseases can cross borders within hours, epidemiological literacy has become a cornerstone of global resilience.
What Is Epidemiology?
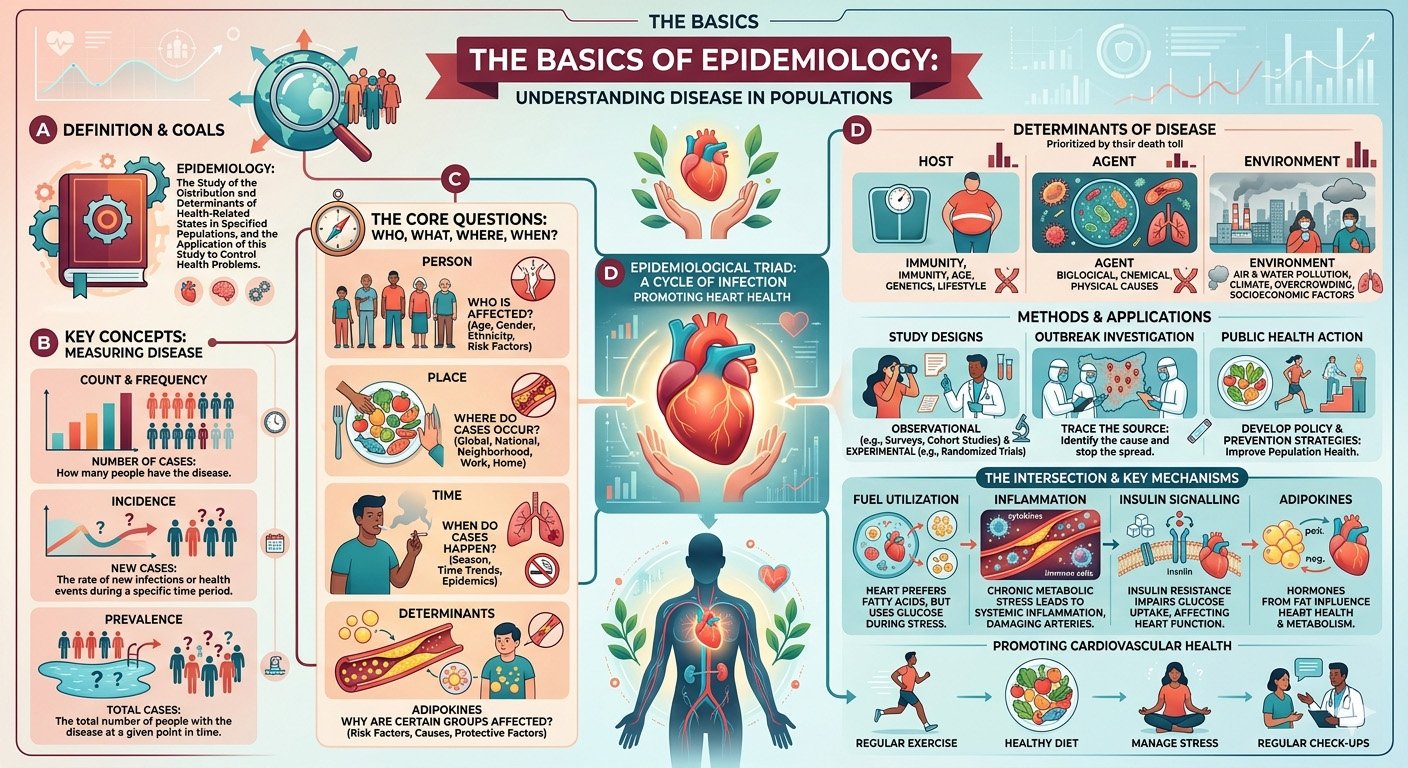
Epidemiology is the study of the distribution and determinants of health-related events in populations and the application of this knowledge to control health problems.
Unlike clinical medicine, which focuses on individual patients, epidemiology focuses on populations. It examines patterns across communities, regions, and nations to identify trends that inform prevention strategies.
At its core, epidemiology answers four fundamental questions:
- Who is affected?
- Where does the disease occur?
- When does it occur?
- Why does it occur?
These questions form the basis of disease investigation and public health planning.
Epidemiology is used to:
- Detect disease outbreaks
- Identify risk factors
- Evaluate interventions
- Monitor public health trends
- Guide health policy decisions
- Predict future health risks
Without epidemiology, modern public health systems would operate blindly, reacting to crises rather than preventing them.
The Historical Foundations of Epidemiology
Epidemiology did not emerge suddenly. It evolved through centuries of observation, crisis, and scientific innovation.
One of the earliest examples of epidemiological thinking occurred during the cholera outbreaks of the 19th century. Physician John Snow mapped cholera cases in London and identified contaminated water as the source of infection. His work demonstrated that disease patterns could be analyzed scientifically to identify causes and prevent future outbreaks.
This shift transformed medicine from a reactive discipline into a preventive science.
Major milestones in epidemiology include:
- Development of sanitation systems
- Discovery of microbes and germ theory
- Introduction of vaccination programs
- Creation of disease surveillance systems
- Use of statistical modeling in public health
- Global coordination during pandemics
Each advancement expanded the ability of societies to control disease and protect populations.
Core Concepts in Epidemiology
Epidemiology relies on a set of foundational concepts that guide investigation and analysis.
Incidence
Incidence measures the number of new cases of a disease occurring in a population during a specific time period.
It helps determine how quickly a disease is spreading.
High incidence often signals:
- Active transmission
- Emerging outbreaks
- Environmental exposure
- Behavioral risk factors
Incidence is critical for outbreak detection and response planning.
Prevalence
Prevalence measures the total number of existing cases of a disease in a population at a given time.
It reflects the overall burden of disease.
High prevalence may indicate:
- Chronic disease persistence
- Improved survival rates
- Long-term exposure risks
- Inadequate treatment access
Prevalence helps governments allocate healthcare resources.
Mortality Rate
Mortality rate measures the number of deaths in a population over a specific period.
It is used to assess disease severity and healthcare effectiveness.
Mortality indicators include:
- Crude mortality rate
- Age-specific mortality rate
- Cause-specific mortality rate
- Case fatality rate
These metrics guide emergency response and healthcare planning.
Risk Factors
Risk factors are characteristics or exposures that increase the likelihood of developing a disease.
They can be:
Biological
- Genetics
- Age
- Immune status
Behavioral
- Smoking
- Poor diet
- Physical inactivity
Environmental
- Pollution
- Unsafe water
- Climate conditions
Social
- Poverty
- Education level
- Housing conditions
Identifying risk factors is one of the most powerful tools in disease prevention.
Types of Epidemiology
Epidemiology is not a single discipline. It includes specialized branches that focus on different aspects of health.
Descriptive Epidemiology
Descriptive epidemiology examines patterns of disease based on:
Person
Place
Time
It answers:
What is happening?
Where is it happening?
When is it happening?
This type of epidemiology is often the first step in identifying outbreaks.
Analytical Epidemiology
Analytical epidemiology investigates causes and relationships between exposures and disease outcomes.
It answers:
Why is this happening?
How is it happening?
This branch uses statistical methods to test hypotheses and identify causal factors.
Clinical Epidemiology
Clinical epidemiology focuses on patient outcomes, treatment effectiveness, and diagnostic accuracy.
It supports:
Evidence-based medicine
Treatment guidelines
Healthcare quality improvement
Environmental Epidemiology
Environmental epidemiology studies how environmental factors affect health.
Examples include:
Air pollution
Water contamination
Chemical exposure
Climate change
This field has become increasingly important as environmental risks grow worldwide.
Social Epidemiology
Social epidemiology examines how social conditions influence health outcomes.
Key factors include:
Income inequality
Education
Employment
Housing
Access to healthcare
Social determinants of health are now recognized as major drivers of disease patterns.
The Epidemiological Triangle
One of the most important models in epidemiology is the epidemiological triangle.
It explains how disease results from the interaction of three components:
Agent
Host
Environment
Agent
The cause of disease, such as bacteria, viruses, toxins, or physical hazards.
Host
The individual or population susceptible to disease.
Environment
External conditions that allow disease transmission.
Disease occurs when these three factors interact in a way that enables transmission or exposure.
This model helps public health professionals design targeted interventions.
Disease Surveillance and Monitoring
Disease surveillance is the continuous collection, analysis, and interpretation of health data.
It allows authorities to detect threats early and respond quickly.
Surveillance systems track:
Infectious diseases
Chronic diseases
Injuries
Environmental hazards
Mental health trends
Vaccination coverage
Modern surveillance uses:
Laboratory testing
Electronic health records
Mobile reporting systems
Statistical modeling
Artificial intelligence
Surveillance is the backbone of epidemic preparedness.
Outbreak Investigation
When an unusual number of cases occurs, epidemiologists conduct an outbreak investigation.
This process typically follows a structured sequence.
Steps include:
Confirming the outbreak
Defining the case
Collecting data
Identifying patterns
Testing hypotheses
Implementing control measures
Evaluating outcomes
Rapid investigation can prevent thousands of additional infections.
Measures of Disease Transmission
Understanding how diseases spread is essential for controlling epidemics.
One of the most important indicators is the reproduction number.
Basic Reproduction Number (R₀)
The basic reproduction number represents the average number of people one infected person will transmit the disease to in a fully susceptible population.
R0>1R_0 > 1R0>1
When the reproduction number is greater than one, the disease spreads.
When it is less than one, the outbreak declines.
Public health interventions aim to reduce transmission below this threshold.
Modes of Disease Transmission
Diseases spread through different pathways depending on the pathogen and environment.
Common transmission modes include:
Direct contact
Respiratory droplets
Airborne particles
Contaminated surfaces
Food and water
Vector-borne transmission
Blood and body fluids
Understanding transmission pathways allows targeted prevention strategies.
Examples:
Hand hygiene reduces contact transmission
Vaccination reduces susceptibility
Water treatment prevents gastrointestinal disease
Mosquito control prevents vector-borne infections
The Role of Epidemiology in Public Health Policy
Epidemiology directly influences public health decisions.
Governments rely on epidemiological data to:
Design vaccination programs
Set quarantine policies
Allocate healthcare resources
Regulate environmental hazards
Plan emergency responses
Evaluate health interventions
Evidence-based policy reduces uncertainty and improves outcomes.
Without epidemiological data, public health policy becomes reactive rather than preventive.
Epidemiology and Chronic Diseases
While epidemiology is often associated with infectious diseases, it plays an equally important role in chronic disease prevention.
Chronic diseases now represent the leading cause of death worldwide.
Examples include:
Heart disease
Cancer
Diabetes
Stroke
Respiratory diseases
Epidemiology identifies:
Behavioral risk patterns
Environmental exposures
Population trends
Preventable risk factors
This information guides prevention strategies such as:
Tobacco control
Nutrition policies
Physical activity programs
Screening campaigns
Chronic disease epidemiology has transformed public health from crisis management into long-term prevention planning.
Epidemiology in Global Health Emergencies
Global health emergencies demonstrate the importance of epidemiology in real time.
During pandemics, epidemiologists:
Track infection rates
Model disease spread
Identify vulnerable populations
Evaluate interventions
Guide vaccination strategies
Their work supports coordinated international responses.
In large-scale emergencies, epidemiology becomes the primary decision-making framework.
Ethical Principles in Epidemiology
Epidemiological research must balance public health protection with individual rights.
Key ethical principles include:
Privacy and confidentiality
Informed consent
Equity
Transparency
Scientific integrity
Ethical epidemiology builds public trust, which is essential for compliance with health measures.
Without trust, even effective interventions can fail.
The Future of Epidemiology
Epidemiology is evolving rapidly with advances in technology and data science.
Emerging trends include:
Artificial intelligence in disease prediction
Genomic epidemiology
Real-time surveillance systems
Digital contact tracing
Climate-health modeling
Global health data integration
These innovations will transform how societies detect and respond to health threats.
Future epidemiology will be faster, more precise, and more predictive.
Why Epidemiology Matters
Epidemiology is not just a scientific discipline. It is a societal safeguard.
It allows communities to:
Detect threats early
Prevent disease
Allocate resources efficiently
Reduce healthcare costs
Protect vulnerable populations
Improve quality of life
Every vaccination campaign, sanitation system, and disease prevention strategy is rooted in epidemiological science.
Understanding the basics of epidemiology means understanding how societies protect themselves from invisible threats.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
SOURCES:
Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov/csels/dsepd/ss1978/index.html
World Health Organization (WHO)
https://www.who.int/health-topics/epidemiology
Johns Hopkins Bloomberg School of Public Health
https://www.jhsph.edu/departments/epidemiology
National Institutes of Health (NIH)
https://www.nih.gov
European Centre for Disease Prevention and Control (ECDC)
https://www.ecdc.europa.eu
Oxford Academic
https://academic.oup.com
