
Risk Comparisons to Better Understand Probabilities
How Comparing Risks Improves Decision-Making, Public Health Communication, and Statistical Literacy
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Understanding risk is one of the most important skills in modern health and science literacy. Yet many people struggle to interpret probabilities correctly, especially when numbers are presented in isolation. A risk of 1% may sound small or large depending on context, framing, and comparison.
Risk comparisons help translate abstract probabilities into meaningful information. They allow individuals, healthcare professionals, and policymakers to evaluate dangers realistically, avoid cognitive biases, and make informed decisions. In public health, risk comparison is a core tool for communicating safety, evaluating interventions, and prioritizing resources.
From medical treatments and lifestyle choices to environmental hazards and infectious diseases, comparing risks provides clarity in situations where uncertainty is unavoidable.
What Is Risk Comparison?
Risk comparison is the process of evaluating one risk relative to another in order to understand magnitude, likelihood, or impact.
Instead of presenting a probability alone, risk comparison answers the practical question:
“How risky is this compared to something familiar?”
For example:
- Risk of a severe vaccine reaction
- Risk of hospitalization from infection
- Risk of injury from daily activities
- Risk of disease from lifestyle factors
When risks are compared, people can better judge proportional danger.
Risk comparison transforms numbers into understanding.
Why Humans Struggle to Understand Probabilities
Human intuition is not naturally suited to interpreting probabilities. Psychological research shows that people rely on mental shortcuts—known as heuristics—that can distort risk perception.
Common cognitive biases include:
Availability bias
People overestimate risks they hear about frequently.
Fear amplification
Emotionally charged risks feel larger than statistically common ones.
Numeracy limitations
Many individuals have difficulty interpreting percentages, ratios, and probabilities.
Framing effects
The same statistic can produce different reactions depending on wording.
For example:
- “1 in 1,000 risk”
- “0.1% risk”
These statements describe the same probability but may feel different psychologically.
Risk comparisons reduce misunderstanding by providing context.
Absolute Risk vs Relative Risk
One of the most important distinctions in risk communication is the difference between absolute risk and relative risk.
Absolute Risk
Absolute risk describes the actual probability of an event occurring.
Example:
- 2 out of 1,000 people develop a condition
- Absolute risk = 0.2%
Absolute risk answers:
“What is the chance this will happen?”
Relative Risk
Relative risk compares the risk between two groups.
Example:
- Group A risk: 2 per 1,000
- Group B risk: 4 per 1,000
Relative risk:
RR=RiskexposedRiskunexposedRR = \frac{Risk_{exposed}}{Risk_{unexposed}}RR=RiskunexposedRiskexposed
In this example:
Relative risk = 2
This means:
The risk doubled.
But the absolute increase remains small.
Understanding this distinction prevents exaggerated interpretations of risk.
Risk Ratios and Probability Comparisons
Risk comparisons often use ratios to describe differences between probabilities.
Common formats include:
Risk ratio
Odds ratio
Percentage change
Frequency comparison
Rate comparison
For example:
Risk A: 1 in 10,000
Risk B: 1 in 1,000
Risk B is:
10 times higher.
However, both risks remain relatively low in absolute terms.
Risk comparisons help distinguish:
Large relative changes
Small absolute risks
This distinction is essential for evidence-based decision-making.
The Importance of Baseline Risk
Baseline risk is the starting probability before any intervention or exposure occurs.
Without baseline risk, comparisons can be misleading.
For example:
A medication reduces risk by 50%.
This sounds dramatic.
But if the baseline risk is:
2 in 10,000
The new risk becomes:
1 in 10,000
The benefit is real, but the magnitude is modest.
Baseline risk provides context for interpreting effectiveness.
Risk Comparisons in Public Health Communication
Public health agencies rely heavily on risk comparisons to communicate safety and urgency.
Effective communication requires balancing:
Accuracy
Clarity
Trust
Transparency
Risk comparisons are used in:
Vaccination campaigns
Disease prevention messaging
Environmental safety guidelines
Food safety warnings
Emergency response planning
When risk communication fails, public confusion increases.
Clear comparisons reduce panic and misinformation.
Comparing Health Risks in Everyday Life
Risk comparisons are relevant far beyond scientific research.
They influence daily decisions.
Common examples include:
Smoking vs non-smoking disease risk
Obesity vs healthy weight health risk
Physical inactivity vs active lifestyle risk
Driving vs flying injury risk
Alcohol consumption vs abstinence risk
These comparisons help individuals prioritize behavior changes.
Risk comparison turns statistics into practical guidance.
Risk Perception and Emotional Response
Risk is not only mathematical—it is psychological.
People evaluate risk through emotion as well as data.
Factors that amplify perceived risk include:
Novel threats
Invisible hazards
Uncontrollable risks
Catastrophic potential
Media coverage intensity
Conversely, familiar risks are often underestimated.
For example:
Driving is statistically dangerous
Yet widely accepted
Air travel is statistically safer
Yet often feared
Risk comparison helps align perception with reality.
Communicating Risk Using Natural Frequencies
Research shows that people understand probabilities better when numbers are presented as natural frequencies rather than percentages.
Instead of:
0.1%
Use:
1 in 1,000
Natural frequency formats improve comprehension across education levels.
They are widely recommended in:
Medicine
Public health
Risk communication
Patient counseling
Natural frequencies make risk tangible.
Risk Comparisons in Medical Decision-Making
Healthcare professionals use risk comparisons to guide treatment decisions.
Patients must often choose between options that carry different probabilities of benefit and harm.
Examples include:
Surgery vs medication
Screening vs no screening
Treatment vs observation
Preventive therapy vs lifestyle change
Risk comparisons allow patients to evaluate:
Potential benefits
Potential side effects
Long-term outcomes
Informed decisions depend on clear comparisons.
Risk Comparisons and Preventive Medicine
Preventive medicine relies heavily on comparing risks.
Interventions are prioritized based on:
Risk reduction potential
Population impact
Cost-effectiveness
Feasibility
Equity
For example:
Vaccination programs
Screening programs
Smoking cessation initiatives
Nutrition policies
Safety regulations
Risk comparison ensures that resources are directed toward interventions with the greatest benefit.
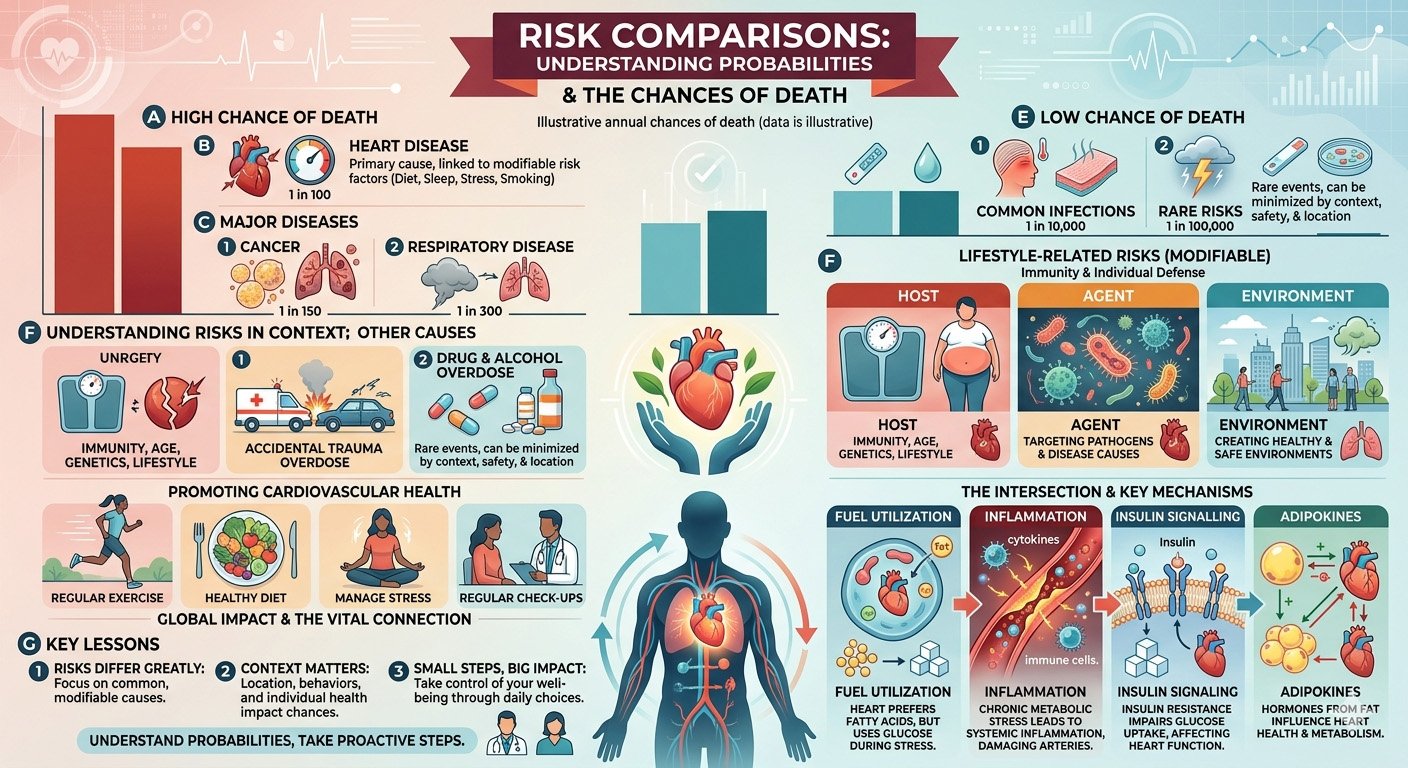
Risk Comparisons in Environmental and Occupational Health
Environmental and workplace risks are often complex and difficult to interpret.
Risk comparisons help evaluate exposure hazards such as:
Air pollution
Chemical exposure
Radiation
Noise
Occupational injuries
Regulatory agencies use risk comparisons to determine:
Safety thresholds
Exposure limits
Protective standards
These comparisons protect workers and communities.
Common Mistakes in Risk Interpretation
Misinterpreting risk can lead to poor decisions.
Frequent errors include:
Confusing relative risk with absolute risk
Ignoring baseline risk
Overreacting to rare events
Underestimating common risks
Misunderstanding percentages
Misinterpreting statistical uncertainty
Risk comparisons reduce these errors by providing context.
Risk Comparisons in Epidemiology and Health Statistics
In epidemiology, risk comparison is a fundamental method for identifying associations between exposures and outcomes.
Researchers use risk comparisons to:
Detect disease patterns
Evaluate interventions
Measure treatment effectiveness
Identify risk factors
Monitor population health
Risk comparison supports:
Evidence-based medicine
Public health policy
Clinical decision-making
Without risk comparison, statistical findings would be difficult to interpret.
The Role of Risk Comparison in Media and Public Understanding
Media reporting plays a major role in shaping public perception of risk.
When risks are reported without comparison, audiences may misinterpret danger levels.
Responsible reporting includes:
Contextual statistics
Comparative benchmarks
Absolute risk values
Clear explanations
Avoidance of sensational framing
Accurate risk communication builds public trust.
The Future of Risk Communication
Risk communication is evolving alongside advances in data science and public health.
Emerging developments include:
Real-time risk dashboards
Personalized risk prediction models
Artificial intelligence risk analysis
Interactive probability tools
Behavioral science integration
These innovations will improve public understanding of risk.
Clear communication will remain essential.
Why Risk Comparisons Matter
Risk comparisons transform abstract numbers into meaningful knowledge.
They help individuals:
Understand probabilities
Evaluate trade-offs
Make informed decisions
Reduce unnecessary fear
Adopt preventive behaviors
They help societies:
Allocate resources efficiently
Communicate risks transparently
Protect public health
Build trust in science
Improve long-term outcomes
In a world filled with uncertainty, risk comparison is one of the most powerful tools for turning data into understanding.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources:
Gigerenzer, Gerd — Risk Literacy and Health Communication (Max Planck Institute)
https://www.mpib-berlin.mpg.de/en/research/risk-literacy
National Cancer Institute (NCI) — Understanding Risk and Probability
https://www.cancer.gov/about-cancer/understanding/statistics
Centers for Disease Control and Prevention (CDC) — Principles of Epidemiology in Public Health Practice
https://www.cdc.gov/csels/dsepd/ss1978/index.html
World Health Organization (WHO) — Communicating Risk in Public Health Emergencies
https://www.who.int/publications/i/item/9789241550208
National Institute of Standards and Technology (NIST) — Communicating Uncertainty and Risk
https://www.nist.gov/topics/risk-management
BMJ (British Medical Journal) — Understanding Absolute and Relative Risk
https://www.bmj.com/about-bmj/resources-readers/publications/statistics-square-one/11-absolute-and-relative-risk
