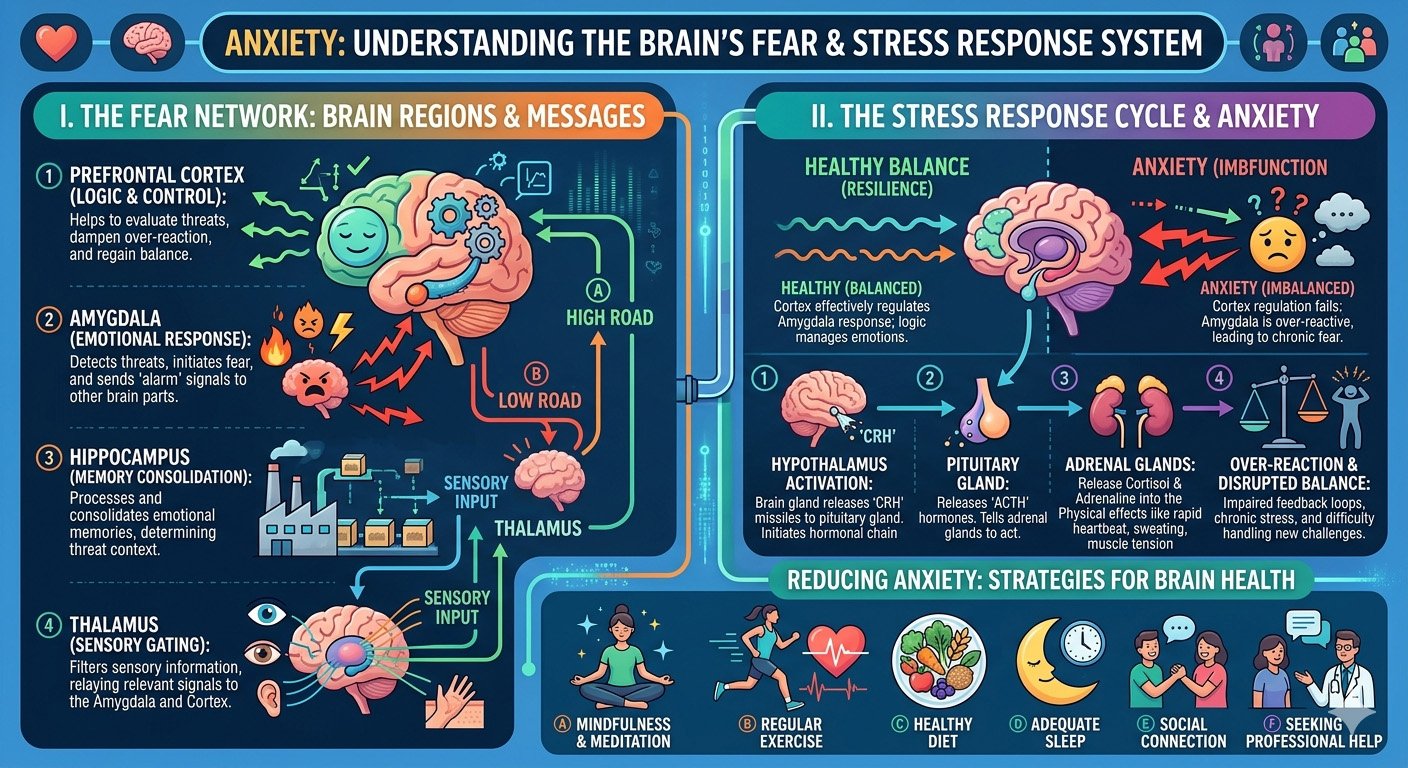
Anxiety: Understanding the Brain’s Fear and Stress Response System
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Anxiety is one of the most fundamental emotional responses in human biology. It evolved as a survival mechanism designed to detect danger, mobilize energy, and protect the organism from harm. In modern life, however, the same neural systems that once protected humans from predators and environmental threats are frequently activated by psychological stressors—deadlines, financial uncertainty, social pressures, health concerns, and constant information exposure.
When this fear and stress response system becomes chronically activated, anxiety shifts from a protective signal into a disruptive physiological state. It begins to alter brain function, hormonal balance, immune activity, and emotional regulation. Over time, anxiety can affect nearly every system in the body, increasing vulnerability to both mental and physical disease.
Understanding anxiety requires understanding the brain systems that generate it. Anxiety is not simply an emotion—it is a coordinated biological response involving neural circuits, stress hormones, memory systems, and survival mechanisms designed to anticipate threat.
The Evolutionary Purpose of Anxiety
Anxiety originated as a predictive survival system. Unlike fear, which responds to immediate danger, anxiety anticipates potential threats before they occur. This anticipatory function allows the brain to prepare the body for action in uncertain environments.
In early human history, this system improved survival by increasing vigilance, accelerating reaction time, and enhancing threat detection. The body entered a state of readiness that supported rapid escape or defense.
Key survival functions of anxiety include:
- Heightened awareness of surroundings
- Faster reaction time
- Increased attention to potential danger
- Mobilization of energy
- Risk assessment and avoidance behavior
In short-term situations, anxiety is adaptive and protective. It becomes harmful when the threat detection system remains active without resolution.
Modern environments expose individuals to persistent psychological stress rather than short-term physical danger. As a result, the anxiety system is often triggered continuously, even when physical safety is not at risk.
The Brain’s Fear Circuit: The Role of the Amygdala
At the center of the anxiety response is the amygdala, a small almond-shaped structure deep within the brain responsible for detecting threats and generating emotional responses.
The amygdala acts as an early warning system. It continuously scans sensory input for signs of danger. When a potential threat is detected, the amygdala sends signals to other brain regions that initiate the stress response.
This process occurs rapidly—often before conscious awareness.
The amygdala communicates with:
- The hypothalamus
- The brainstem
- The prefrontal cortex
- The hippocampus
Together, these regions form the brain’s fear network.
When the amygdala becomes overactive, the brain begins to interpret neutral situations as threatening. This heightened sensitivity is a hallmark of anxiety disorders.
Over time, repeated activation strengthens fear pathways in the brain, making anxiety responses more automatic and more difficult to regulate.
The Hypothalamic-Pituitary-Adrenal (HPA) Axis: The Stress Response Engine
Once the amygdala detects threat, it activates the hypothalamus, which triggers the hypothalamic-pituitary-adrenal (HPA) axis—the body’s central stress response system.
This system releases stress hormones that prepare the body for action.
The sequence unfolds in stages:
- The hypothalamus releases corticotropin-releasing hormone (CRH)
- The pituitary gland releases adrenocorticotropic hormone (ACTH)
- The adrenal glands release cortisol
Cortisol increases:
- Blood sugar levels
- Heart rate
- Blood pressure
- Energy availability
- Alertness
In acute situations, this response enhances survival. In chronic anxiety, repeated activation keeps the body in a prolonged state of physiological arousal.
This state is often described as:
Hyperarousal
The body remains prepared for danger even when no threat is present.
The Prefrontal Cortex: The Brain’s Regulatory System
While the amygdala generates emotional responses, the prefrontal cortex regulates them.
This region of the brain is responsible for:
- Decision-making
- Risk evaluation
- Emotional control
- Impulse regulation
- Planning and judgment
The prefrontal cortex acts as a braking system for the fear response. It evaluates whether a perceived threat is real and determines whether the stress response should continue.
Under chronic stress and anxiety, the regulatory capacity of the prefrontal cortex weakens.
This imbalance leads to:
- Increased emotional reactivity
- Difficulty calming down
- Impaired concentration
- Reduced problem-solving ability
- Persistent worry
In severe anxiety, the emotional system overrides rational control.
The Hippocampus: Memory and Threat Context
The hippocampus plays a critical role in distinguishing real threats from remembered experiences.
It stores contextual memories and helps the brain recognize whether a situation is safe or dangerous.
Chronic stress and elevated cortisol can impair hippocampal function, reducing the brain’s ability to regulate fear responses.
This impairment contributes to:
- Persistent worry
- Intrusive memories
- Difficulty learning new information
- Heightened sensitivity to stress
- Emotional instability
The interaction between the hippocampus and amygdala explains why past experiences can shape future anxiety responses.

The Autonomic Nervous System: Fight, Flight, or Freeze
The autonomic nervous system controls the body’s immediate response to threat.
It has two major branches:
Sympathetic nervous system
Activates the fight-or-flight response.
Parasympathetic nervous system
Promotes recovery and relaxation.
In anxiety, the sympathetic system dominates.
This dominance produces physical symptoms such as:
- Rapid heart rate
- Muscle tension
- Shortness of breath
- Sweating
- Trembling
- Digestive discomfort
When the parasympathetic system fails to restore balance, the body remains in a prolonged state of activation.
This persistent activation is one of the defining features of chronic anxiety.
Neurotransmitters and Anxiety Regulation
Anxiety is strongly influenced by chemical messengers in the brain known as neurotransmitters.
Three key neurotransmitters regulate anxiety:
Serotonin
Supports mood stability and emotional regulation.
Dopamine
Regulates motivation, reward, and focus.
Gamma-aminobutyric acid (GABA)
Acts as the brain’s primary inhibitory neurotransmitter, reducing neural activity and promoting calmness.
Imbalances in these neurotransmitters can increase anxiety sensitivity and reduce the brain’s ability to regulate emotional responses.
This biochemical dimension explains why medications that target these systems can reduce anxiety symptoms.
Chronic Anxiety and the Body: A System-Wide Response
Although anxiety originates in the brain, its effects extend throughout the body.
Chronic anxiety is associated with:
Cardiovascular effects:
- Elevated blood pressure
- Increased heart rate
- Increased risk of heart disease
Immune effects:
- Increased inflammation
- Reduced immune defense
- Slower recovery from illness
Metabolic effects:
- Increased blood sugar levels
- Appetite changes
- Weight fluctuations
Digestive effects:
- Irritable bowel symptoms
- Nausea
- Stomach discomfort
Sleep effects:
- Insomnia
- Fragmented sleep
- Reduced deep sleep
Anxiety is therefore both a psychological and physiological condition.
The Anxiety-Stress Feedback Loop
Anxiety and stress reinforce each other in a self-sustaining cycle.
Stress increases physiological arousal.
Increased arousal increases anxiety.
Anxiety increases vigilance.
Heightened vigilance increases stress.
This cycle can persist for months or years if not interrupted.
Over time, the nervous system becomes more sensitive to stress signals—a process known as sensitization.
This heightened sensitivity lowers the threshold for anxiety responses.
Modern Triggers of Anxiety
Modern environments contain persistent triggers that activate the brain’s fear system.
Common triggers include:
- Financial uncertainty
- Occupational pressure
- Health concerns
- Social comparison
- Digital overload
- Information saturation
- Sleep disruption
- Chronic stress
Unlike acute threats, these triggers often have no clear resolution, keeping the brain in a state of anticipation.
This persistent uncertainty is one of the defining characteristics of modern anxiety.
When Anxiety Becomes a Disorder
Occasional anxiety is normal. Anxiety becomes a disorder when the response is excessive, persistent, and disruptive to daily functioning.
Clinical anxiety disorders include:
- Generalized anxiety disorder (GAD)
- Panic disorder
- Social anxiety disorder
- Specific phobias
- Post-traumatic stress disorder (PTSD)
These conditions are characterized by:
- Persistent worry
- Difficulty controlling fear
- Physical symptoms of stress
- Avoidance behavior
- Functional impairment
Early recognition is critical for prevention and treatment.
Signs That the Anxiety System Is Overactive
Common warning signs include:
Emotional signs:
- Constant worry
- Irritability
- Restlessness
- Difficulty relaxing
- Feeling overwhelmed
Physical signs:
- Muscle tension
- Rapid heartbeat
- Headaches
- Fatigue
- Sleep problems
Cognitive signs:
- Difficulty concentrating
- Racing thoughts
- Indecision
- Persistent fear of negative outcomes
These symptoms reflect activation of the brain’s threat detection system.
The Core Insight: Anxiety Is a Biological Alarm System
Anxiety is not simply a psychological weakness or personality trait. It is a biological alarm system designed to detect danger and protect survival.
When functioning properly, this system enhances awareness and promotes safety. When chronically activated, it can disrupt emotional stability, impair cognitive function, and increase vulnerability to disease.
Understanding the brain mechanisms behind anxiety provides a foundation for prevention, early recognition, and effective management. It shifts the perspective from blame to biology—and from fear to understanding.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
SOURCES:
National Institute of Mental Health (NIMH) – Anxiety Disorders
https://www.nimh.nih.gov/health/topics/anxiety-disorders
American Psychological Association (APA) – Anxiety
https://www.apa.org/topics/anxiety
Centers for Disease Control and Prevention (CDC) – Anxiety and Depression
https://www.cdc.gov/mentalhealth/anxiety-depression
Harvard Health Publishing – Understanding Anxiety
https://www.health.harvard.edu/mind-and-mood/understanding-anxiety
Mayo Clinic – Anxiety Disorders
https://www.mayoclinic.org/diseases-conditions/anxiety/symptoms-causes/syc-20350961
World Health Organization (WHO) – Anxiety Disorders
https://www.who.int/news-room/fact-sheets/detail/anxiety-disorders
