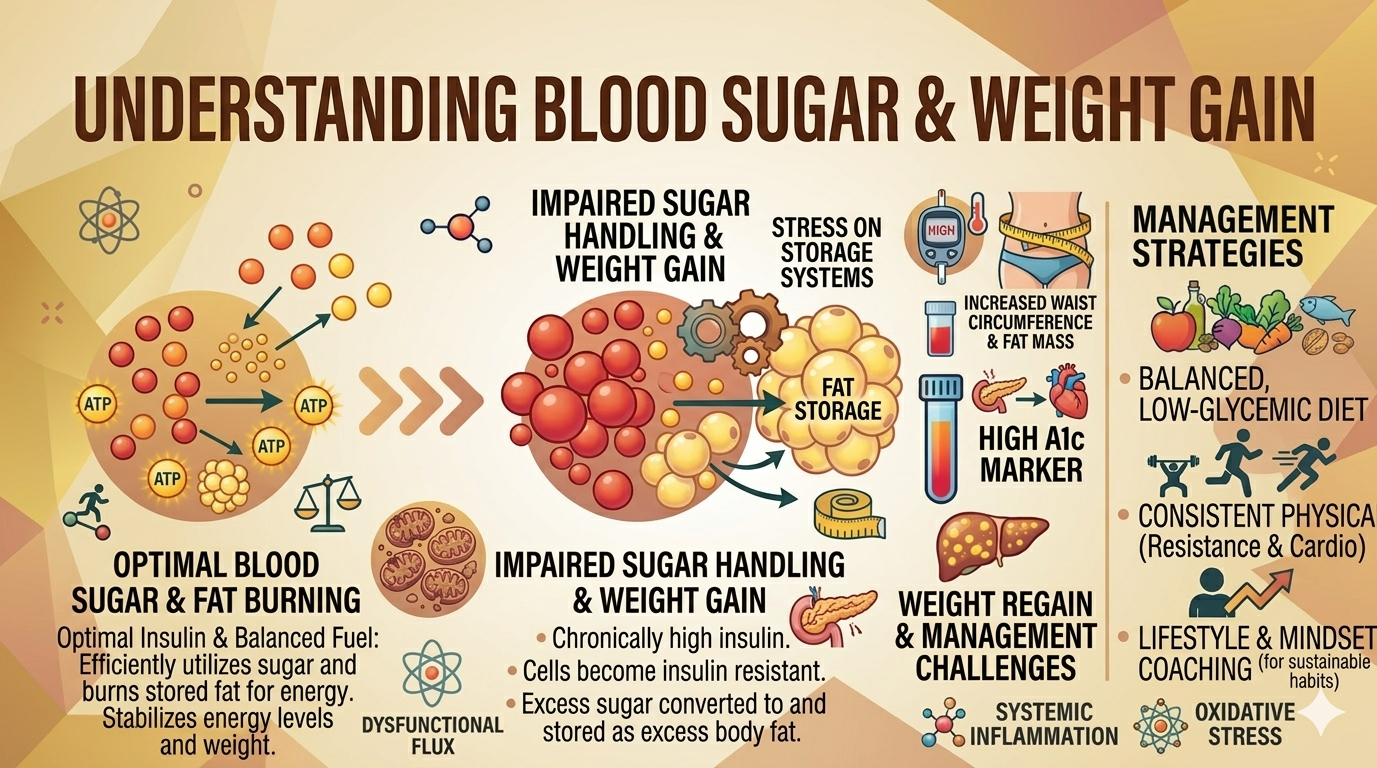
Blood Sugar and Weight Gain: How Glucose Levels Influence Body Fat and Metabolic Health
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction
Blood sugar plays a central role in how the body stores and uses energy. When glucose levels rise frequently or remain elevated over time, the body may shift toward storing more energy as fat. This connection explains why blood sugar regulation is closely linked to body weight, fat distribution, and long-term metabolic health.
Weight gain is not determined solely by calorie intake. Hormonal responses — particularly insulin — influence how nutrients are processed, stored, and used for energy. These processes are part of the broader system of Metabolism, which interacts closely with dietary habits in Nutrition and regulatory signals within Hormone Health.
Understanding the relationship between blood sugar and weight gain can help explain why some individuals gain weight more easily, experience persistent hunger, or struggle to lose fat despite lifestyle changes.
What Is the Relationship Between Blood Sugar and Weight Gain?
Blood sugar and weight gain are connected through the body’s energy regulation system. When blood sugar rises after eating, the hormone insulin helps move glucose into cells for energy or storage.
If blood sugar levels rise frequently — especially from high-glycemic foods or excess calorie intake — insulin levels may remain elevated. Over time, this can promote fat storage and reduce the body’s ability to burn stored energy efficiently.
This process does not happen overnight. Instead, gradual changes in blood sugar regulation can lead to:
- Increased fat storage
- Reduced fat burning
- Greater appetite and cravings
- Difficulty maintaining a healthy weight
These patterns are commonly observed in conditions related to Blood Sugar regulation and metabolic balance.
How Blood Sugar Influences Weight Gain (Physiology)
The relationship between blood sugar and body weight involves several interconnected biological mechanisms.
Insulin and Fat Storage
Insulin is one of the most important hormones controlling fat storage. When insulin levels rise, the body shifts into a storage mode.
Insulin promotes:
- Glucose storage as glycogen
- Conversion of excess glucose into fat
- Reduced breakdown of stored fat
Frequent insulin spikes can gradually increase body fat, particularly around the abdomen. This process is strongly associated with insulin resistance, a key factor in long-term metabolic dysfunction.
Blood Sugar Spikes and Energy Regulation
Rapid increases in blood sugar — often caused by refined carbohydrates or sugary foods — can lead to sharp insulin responses.
After a spike, blood sugar may drop quickly, triggering:
- Hunger shortly after eating
- Cravings for carbohydrates
- Reduced energy levels
These fluctuations can contribute to patterns discussed in Energy & Fatigue, where unstable glucose levels affect daily energy balance.
Reduced Metabolic Flexibility
Metabolic flexibility refers to the body’s ability to switch between burning carbohydrates and fat for energy.
When blood sugar remains elevated for long periods, the body may rely heavily on glucose and become less efficient at using stored fat. This shift can make weight management more difficult and is closely tied to changes in overall Metabolism.
Key Factors That Influence Blood Sugar and Weight Gain
Several lifestyle and biological factors can affect how blood sugar influences body weight.
Dietary Patterns
The types of foods consumed have a direct impact on blood sugar levels.
Foods that commonly raise blood sugar quickly include:
- Refined carbohydrates
- Sugary beverages
- Highly processed foods
- Low-fiber meals
Dietary quality is one of the strongest determinants of metabolic health and is central to effective Nutrition.
Physical Activity
Regular movement improves insulin sensitivity and helps muscles use glucose more efficiently.
Physical inactivity can lead to:
- Reduced glucose uptake
- Increased fat storage
- Slower metabolism
Exercise is one of the most effective tools for supporting healthy Weight Loss and maintaining metabolic balance.
Sleep and Circadian Rhythm
Sleep affects hormones that regulate appetite, metabolism, and blood sugar.
Poor sleep can:
- Increase hunger hormones
- Reduce insulin sensitivity
- Promote weight gain
These effects highlight the connection between sleep patterns and metabolic regulation in Sleep Health.
Stress and Hormonal Balance
Chronic stress raises cortisol levels, which can increase blood sugar and promote fat storage.
Long-term stress can disrupt appetite regulation and contribute to metabolic imbalance. These interactions are explored more deeply in Hormone Health.
Gut Microbiome and Inflammation
The gut microbiome plays a role in how nutrients are processed and how the body regulates inflammation.
Changes in gut bacteria can influence:
- Insulin sensitivity
- Appetite regulation
- Fat storage
These connections are central to maintaining healthy Gut Health.
Related Conditions and Metabolic Imbalances
Persistent changes in blood sugar regulation can contribute to several metabolic conditions.
Insulin Resistance
Insulin resistance occurs when cells respond less effectively to insulin, leading to higher insulin levels and increased fat storage.
This condition is one of the most common drivers of weight gain and metabolic dysfunction.
Prediabetes and Type 2 Diabetes
Chronic elevation of blood sugar can lead to impaired glucose regulation and eventually type 2 diabetes.
These conditions are strongly associated with long-term metabolic stress and increased cardiovascular risk.
Metabolic Syndrome
Metabolic syndrome is a cluster of risk factors that includes:
- High blood sugar
- Increased abdominal fat
- High blood pressure
- Abnormal cholesterol levels
This condition significantly increases the risk of heart disease, highlighting the importance of maintaining healthy Heart Health.
Fatty Liver Disease
When excess glucose is converted into fat, it can accumulate in the liver.
Over time, this process may lead to non-alcoholic fatty liver disease, a common complication of metabolic dysfunction.
Practical Strategies to Stabilize Blood Sugar and Support Healthy Weight
Managing blood sugar is one of the most effective ways to support long-term weight stability.
Choose Balanced Meals
Balanced meals help prevent rapid changes in blood sugar.
Helpful strategies include:
- Combining protein, fiber, and healthy fats
- Choosing whole foods over processed foods
- Limiting added sugars
- Increasing vegetable intake
These dietary patterns support stable glucose levels and are foundational in Nutrition.

Increase Daily Movement
Regular physical activity improves insulin sensitivity and energy use.
Recommended approaches include:
- Walking after meals
- Strength training
- Aerobic exercise
- Reducing sedentary time
Movement supports efficient glucose metabolism and overall Metabolism.
Maintain Consistent Sleep Patterns
Healthy sleep routines help regulate hormones that control hunger and energy balance.
Helpful habits include:
- Maintaining regular sleep and wake times
- Limiting late-night eating
- Reducing screen exposure before bed
These behaviors support metabolic regulation and are key components of Sleep Health.
Manage Stress Effectively
Reducing stress can improve hormone balance and stabilize blood sugar levels.
Effective strategies include:
- Mindfulness practices
- Regular physical activity
- Structured daily routines
- Relaxation techniques
Stress regulation helps maintain stable glucose control and supports overall Hormone Health.
Why Blood Sugar and Weight Gain Matter for Long-Term Health
The relationship between blood sugar and body weight affects more than appearance or short-term health goals. It plays a central role in preventing chronic disease and maintaining long-term metabolic stability.
Persistent high blood sugar can increase the risk of:
- Type 2 diabetes
- Cardiovascular disease
- Obesity
- Fatty liver disease
- Chronic fatigue
- Hormonal imbalance
Maintaining stable blood sugar levels supports energy balance, protects organ function, and reduces the risk of long-term metabolic disease.
Final Thoughts
Blood sugar and weight gain are closely connected through the body’s energy regulation system. Frequent blood sugar spikes, hormonal changes, and lifestyle factors can gradually shift the body toward fat storage and reduced metabolic efficiency.
Addressing blood sugar regulation requires a whole-system approach that integrates Metabolism, Nutrition, Hormone Health, Sleep Health, and Weight Loss strategies. By supporting these interconnected systems, individuals can improve metabolic resilience and maintain long-term health.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
- Centers for Disease Control and Prevention (CDC)
Diabetes and Blood Sugar - National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK — NIH)
- Insulin Resistance and Prediabetes
- Mayo Clinic
- Hyperglycemia in Diabetes — Symptoms and Causes
- World Health Organization (WHO)
- Obesity and Overweight
- Ludwig DS.
- The Glycemic Index: Physiological Mechanisms Relating to Obesity
JAMA - Hall KD et al.
- Energy Balance and Its Components
American Journal of Clinical Nutrition - Samuel VT, Shulman GI.
- Mechanisms for Insulin Resistance
Cell
