
Depression: Causes, Symptoms, and Evidence-Based Treatment Approaches
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Depression is one of the most complex and consequential health conditions affecting modern societies. It is not simply a temporary feeling of sadness or emotional distress, nor is it a sign of weakness or lack of resilience. Depression is a multifactorial disorder involving biological, psychological, and social mechanisms that interact to alter mood, cognition, behavior, and physical health. It affects how individuals think, feel, sleep, eat, and function in daily life, and in severe cases, it can impair the ability to experience pleasure, maintain relationships, or perform basic responsibilities.
Globally, depression is a leading cause of disability and a major contributor to the overall burden of disease. Its impact extends beyond emotional suffering, influencing cardiovascular health, immune function, metabolic regulation, and neurological processes. Understanding depression requires moving beyond simplistic explanations and examining the underlying biological systems, environmental influences, and evidence-based treatments that shape outcomes.
Understanding Depression as a Brain and Body Disorder
Depression is often categorized as a mood disorder, but its effects extend far beyond mood regulation. It is increasingly recognized as a systemic condition that affects multiple biological systems simultaneously. Changes in brain function, hormonal regulation, immune activity, and energy metabolism contribute to the symptoms observed in depression.
Key biological systems involved include:
- The brain’s mood regulation circuits
- The stress response system
- Neurotransmitter networks
- The immune and inflammatory system
- The sleep-wake cycle
- The endocrine system
Depression can disrupt communication between these systems, leading to persistent emotional distress, cognitive impairment, and physical symptoms such as fatigue, pain, and appetite changes.
The Biological Causes of Depression
Depression rarely has a single cause. Instead, it emerges from the interaction of genetic vulnerability, neurochemical changes, environmental stressors, and psychological factors.
Neurotransmitter Imbalance
Neurotransmitters are chemical messengers that regulate mood, motivation, and emotional stability. Three major neurotransmitters are closely associated with depression:
Serotonin
Involved in mood regulation, sleep, and emotional stability.
Dopamine
Associated with motivation, reward processing, and pleasure.
Norepinephrine
Linked to alertness, energy, and stress response.
Disruptions in these neurotransmitters can impair the brain’s ability to regulate mood and emotional responses.
Brain Structure and Functional Changes
Neuroimaging studies have identified structural and functional differences in the brains of individuals with depression.
Common findings include:
- Reduced activity in the prefrontal cortex
- Increased activity in the amygdala
- Reduced hippocampal volume
- Altered connectivity between emotional regulation networks
These changes can affect decision-making, emotional control, and stress regulation.
Genetic and Hereditary Factors
Genetics play a significant role in depression risk. Individuals with a family history of depression are more likely to develop the condition, particularly when exposed to chronic stress or traumatic experiences.
However, genetics alone do not determine outcomes. Environmental factors and coping mechanisms influence whether genetic vulnerability translates into clinical depression.
Chronic Stress and the HPA Axis
Long-term activation of the stress response system—specifically the hypothalamic-pituitary-adrenal (HPA) axis—can contribute to depression.
Chronic stress leads to:
- Elevated cortisol levels
- Sleep disruption
- Inflammation
- Neurotransmitter imbalance
- Emotional exhaustion
Persistent stress exposure is one of the strongest predictors of depressive disorders.
Inflammation and Immune System Activation
Emerging research suggests that chronic inflammation may play a role in depression. Elevated inflammatory markers have been observed in individuals with depressive symptoms.
Inflammation can:
- Alter neurotransmitter production
- Disrupt brain signaling
- Reduce energy levels
- Affect mood regulation
This connection has led researchers to describe certain forms of depression as inflammatory disorders.
Psychological and Environmental Risk Factors
Depression is strongly influenced by life experiences, social conditions, and psychological stressors.
Common risk factors include:
- Chronic stress
- Traumatic experiences
- Social isolation
- Financial hardship
- Relationship conflict
- Job loss or occupational stress
- Chronic illness
- Sleep deprivation
- Substance misuse
These factors can overwhelm coping systems and increase vulnerability to depressive episodes.
Core Symptoms of Depression
Depression affects emotional, cognitive, physical, and behavioral functioning. Symptoms vary in severity and duration but typically persist for at least two weeks in clinical diagnoses.
Emotional Symptoms
- Persistent sadness or low mood
- Feelings of hopelessness
- Irritability
- Loss of interest in activities
- Emotional numbness
- Feelings of guilt or worthlessness
Cognitive Symptoms
- Difficulty concentrating
- Memory problems
- Slowed thinking
- Indecision
- Negative thought patterns
Physical Symptoms
- Fatigue
- Changes in appetite
- Weight gain or loss
- Sleep disturbances
- Chronic pain
- Reduced energy
Behavioral Symptoms
- Social withdrawal
- Reduced productivity
- Loss of motivation
- Decreased physical activity
- Avoidance behavior
Recognizing these symptoms early can improve treatment outcomes and reduce long-term complications.
Types of Depressive Disorders
Depression is not a single condition but a group of related disorders with different patterns and causes.
Major Depressive Disorder (MDD)
Characterized by persistent sadness and loss of interest lasting at least two weeks.
Persistent Depressive Disorder (Dysthymia)
A chronic, lower-grade form of depression lasting two years or longer.
Seasonal Affective Disorder (SAD)
Depression linked to seasonal changes, often occurring during winter months.
Postpartum Depression
Depression occurring after childbirth, associated with hormonal and emotional changes.
Bipolar Depression
Depressive episodes occurring within bipolar disorder.
Understanding the specific type of depression is essential for selecting appropriate treatment.
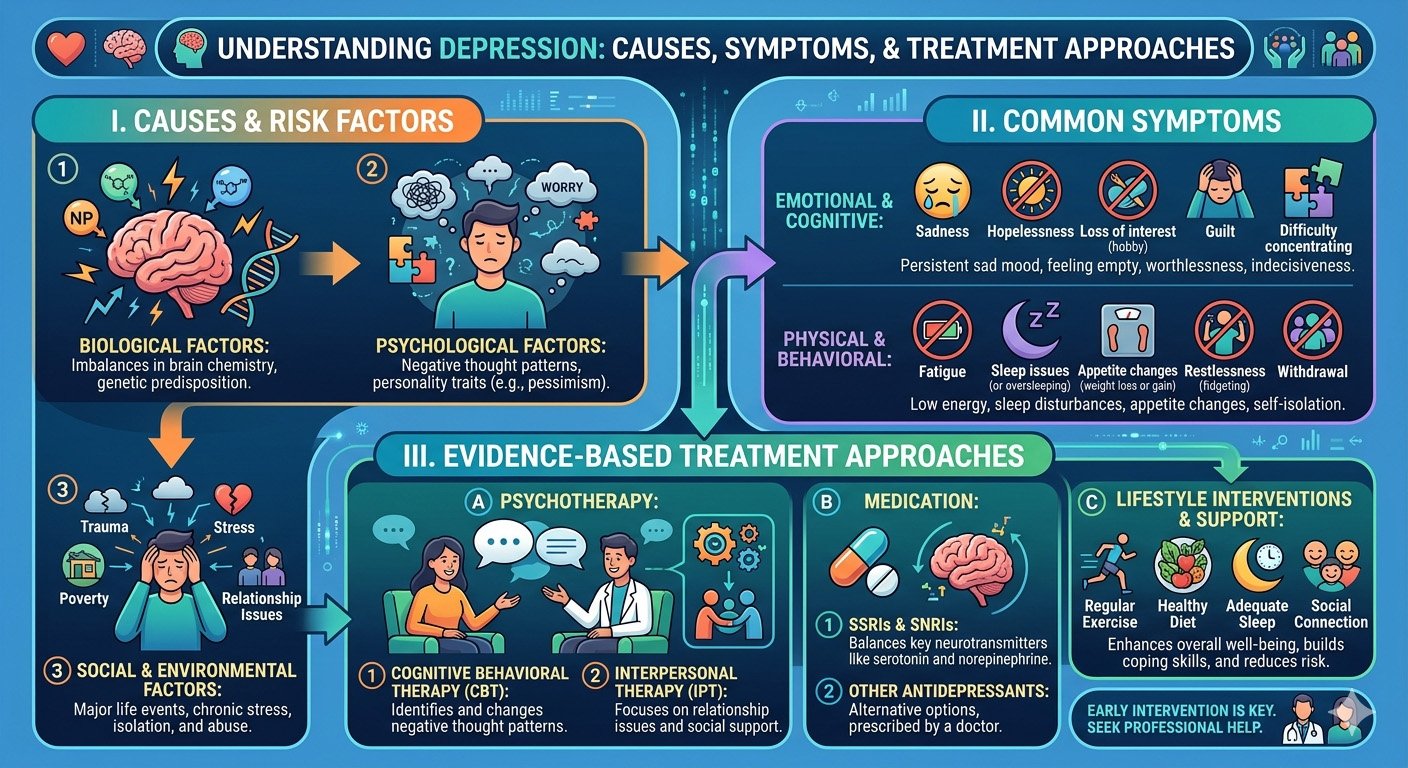
The Relationship Between Depression and Physical Health
Depression is closely linked to chronic physical disease. It can both contribute to and result from medical conditions.
Depression is associated with:
- Cardiovascular disease
- Diabetes
- Obesity
- Chronic pain
- Neurodegenerative disorders
- Immune dysfunction
The relationship is bidirectional. Physical illness can increase depression risk, while depression can worsen physical health outcomes.
Evidence-Based Treatment Approaches
Effective treatment for depression typically involves a combination of medical, psychological, and lifestyle interventions. Evidence-based treatments are supported by clinical research demonstrating safety and effectiveness.
Psychotherapy
Psychotherapy is a primary treatment for depression, particularly for mild to moderate cases.
Common evidence-based therapies include:
Cognitive Behavioral Therapy (CBT)
Focuses on identifying and changing negative thought patterns.
Interpersonal Therapy (IPT)
Addresses relationship problems and social functioning.
Behavioral Activation
Encourages engagement in meaningful activities to improve mood.
Psychotherapy helps individuals develop coping skills, improve emotional regulation, and reduce relapse risk.
Antidepressant Medications
Medications are often recommended for moderate to severe depression.
Common classes include:
Selective Serotonin Reuptake Inhibitors (SSRIs)
Examples: sertraline, fluoxetine, escitalopram.
Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs)
Examples: venlafaxine, duloxetine.
Atypical Antidepressants
Examples: bupropion, mirtazapine.
These medications work by regulating neurotransmitter activity in the brain.
Medication effectiveness varies by individual, and treatment often requires adjustment over time.
Lifestyle and Behavioral Interventions
Lifestyle changes can significantly improve depression outcomes and support long-term recovery.
Evidence-based strategies include:
Regular physical activity
Exercise improves mood and reduces inflammation.
Sleep regulation
Consistent sleep patterns stabilize mood and energy levels.
Balanced nutrition
Healthy diets support brain function.
Stress management
Reducing chronic stress improves emotional stability.
Social connection
Strong relationships protect against depression.
These interventions are often used alongside medical treatment.
Emerging and Advanced Treatments
In treatment-resistant cases, additional interventions may be considered.
Examples include:
Transcranial Magnetic Stimulation (TMS)
Uses magnetic pulses to stimulate brain activity.
Electroconvulsive Therapy (ECT)
A highly effective treatment for severe depression.
Ketamine and Esketamine Therapy
Rapid-acting treatments targeting glutamate pathways.
These therapies are typically used under specialized medical supervision.
Barriers to Treatment and Recovery
Despite effective treatments, many individuals with depression do not receive adequate care.
Common barriers include:
- Stigma surrounding mental illness
- Limited access to healthcare
- Financial constraints
- Lack of awareness about symptoms
- Fear of medication side effects
- Social isolation
Reducing stigma and improving access to treatment are essential for improving outcomes.
Prevention and Long-Term Management
Preventing depression involves strengthening resilience and maintaining stable biological and psychological systems.
Protective factors include:
- Regular sleep
- Physical activity
- Stress management
- Healthy relationships
- Meaningful daily activities
- Emotional support networks
Early intervention is one of the most effective strategies for preventing severe depressive episodes.
The Core Insight: Depression Is a Treatable Medical Condition
Depression is a serious but treatable health condition. It is not a personal failure, a character flaw, or a temporary weakness. It is a complex disorder involving brain function, hormonal regulation, and environmental influences.
Modern research shows that recovery is possible with appropriate treatment, support, and early recognition. Understanding the causes, symptoms, and evidence-based treatments for depression empowers individuals, families, and healthcare systems to respond effectively to one of the most significant health challenges of our time.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
SOURCES:
National Institute of Mental Health (NIMH) – Depression
https://www.nimh.nih.gov/health/topics/depression
World Health Organization (WHO) – Depression
https://www.who.int/news-room/fact-sheets/detail/depression
American Psychiatric Association – What Is Depression?
https://www.psychiatry.org/patients-families/depression/what-is-depression
Centers for Disease Control and Prevention (CDC) – Depression
https://www.cdc.gov/mentalhealth/depression
Mayo Clinic – Depression (Major Depressive Disorder)
https://www.mayoclinic.org/diseases-conditions/depression/symptoms-causes/syc-20356007
Harvard Health Publishing – What Causes Depression?
https://www.health.harvard.edu/mind-and-mood/what-causes-depression
