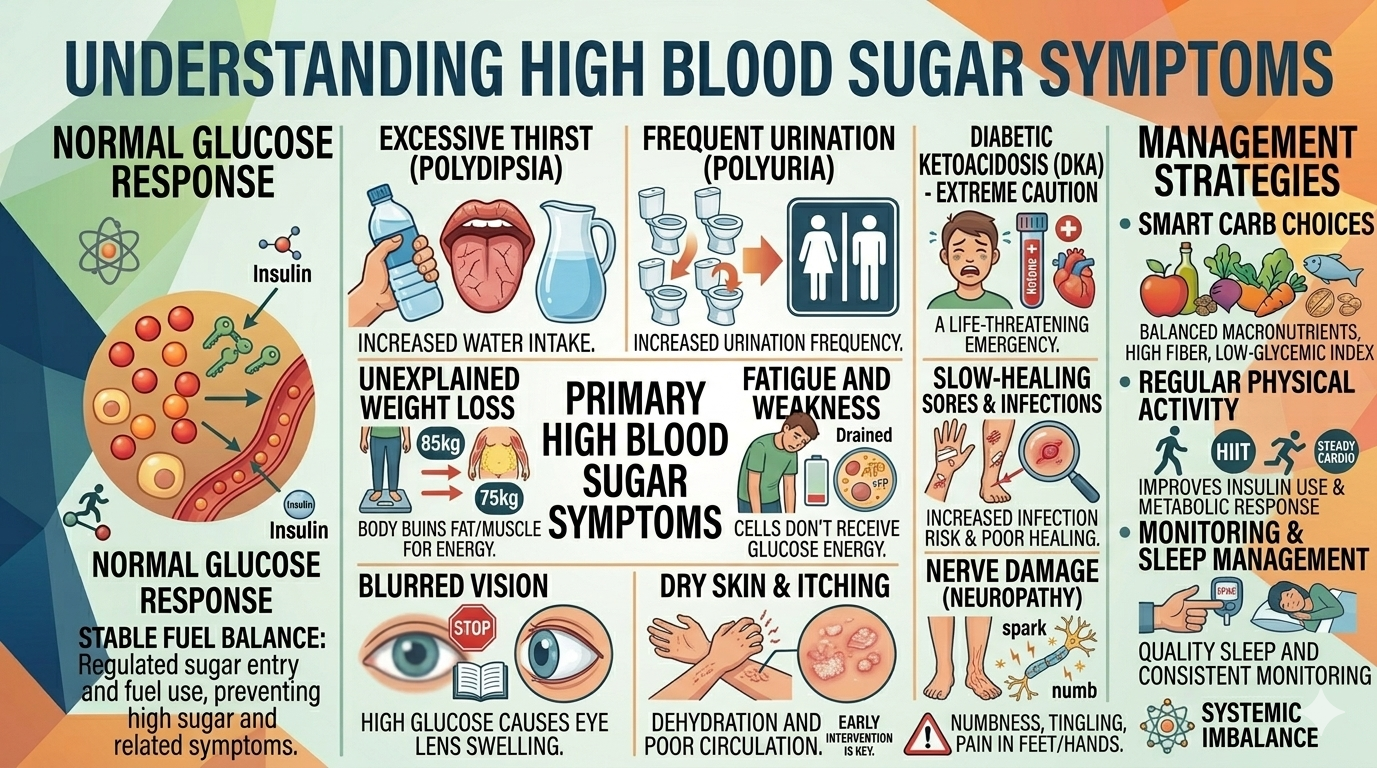
High Blood Sugar Symptoms (Hyperglycemia)
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction
Blood sugar levels fluctuate naturally throughout the day, but persistently elevated glucose levels can signal a deeper metabolic imbalance. High blood sugar symptoms, also known as hyperglycemia, often develop gradually and may go unnoticed in the early stages. Over time, however, these symptoms can affect multiple body systems, including energy regulation, hormone signaling, cardiovascular health, and brain function.
Understanding the early warning signs of hyperglycemia is essential not only for people with diabetes but also for individuals at risk of metabolic dysfunction. Elevated blood glucose is closely linked to Metabolism, Hormone Health, and Nutrition, and it can also influence Sleep Health, Heart Health, and Energy & Fatigue patterns.
Recognizing symptoms early allows for timely intervention, preventing long-term complications and improving overall metabolic stability.
What Is Hyperglycemia?
Hyperglycemia is a condition characterized by abnormally high levels of glucose in the bloodstream.
In clinical terms:
- Fasting blood sugar: above 126 mg/dL
- Post-meal blood sugar: above 180 mg/dL
- Random blood sugar: above 200 mg/dL with symptoms
Hyperglycemia most commonly occurs in:
- Type 1 diabetes
- Type 2 diabetes
- Prediabetes
- Insulin resistance
- Acute illness or stress
However, elevated blood sugar can also occur temporarily due to diet, medications, infections, or hormonal changes.
Because glucose is the body’s primary energy source, maintaining stable levels is central to healthy Metabolism and overall physiological balance.
How High Blood Sugar Affects the Body (Physiology)
Glucose enters the bloodstream after digestion and is transported into cells with the help of insulin, a hormone produced by the pancreas.
When this system becomes impaired:
- Cells cannot efficiently absorb glucose
- Blood glucose accumulates
- Energy production becomes less efficient
- Inflammation and oxidative stress increase
Over time, persistent hyperglycemia can affect:
- Blood vessels
- Nerves
- Kidneys
- Eyes
- Brain
- Immune function
These effects explain why chronic high blood sugar is strongly associated with conditions affecting Heart Health, Gut Health, and long-term metabolic resilience.
Common High Blood Sugar Symptoms
Symptoms of hyperglycemia often develop gradually, especially in type 2 diabetes or insulin resistance.
Early Symptoms
These are the most common early warning signs:
- Increased thirst (polydipsia)
- Frequent urination (polyuria)
- Increased hunger (polyphagia)
- Fatigue or low energy
- Blurred vision
- Dry mouth
- Headaches
Fatigue is particularly common because cells are unable to access glucose efficiently, leading to reduced energy production—closely linking hyperglycemia to Energy & Fatigue regulation.
Moderate Symptoms
As blood sugar levels remain elevated, additional symptoms may appear:
- Slow wound healing
- Recurrent infections
- Skin dryness or itching
- Tingling or numbness in hands and feet
- Difficulty concentrating
- Increased abdominal fat
These symptoms often indicate developing insulin resistance, a key driver of metabolic dysfunction and challenges with Weight Loss.
Severe Symptoms (Medical Urgency)
In more advanced cases, hyperglycemia can lead to dangerous complications.
Seek medical attention if symptoms include:
- Severe dehydration
- Rapid breathing
- Fruity-smelling breath
- Confusion
- Nausea and vomiting
- Weakness or drowsiness
These signs may indicate:
- Diabetic ketoacidosis (DKA)
- Hyperosmolar hyperglycemic state (HHS)
Both are medical emergencies.
Key Factors That Influence High Blood Sugar
Hyperglycemia rarely has a single cause. It typically results from a combination of metabolic, hormonal, and lifestyle factors.
1) Insulin Resistance
This is the most common driver of chronically high blood sugar.
When cells become resistant to insulin:
- Glucose remains in the bloodstream
- The pancreas produces more insulin
- Blood sugar regulation becomes unstable
Insulin resistance is strongly associated with:
- Excess visceral fat
- Sedentary lifestyle
- Poor dietary patterns
- Chronic inflammation
It is a central topic in Metabolism and Hormone Health.
2) Diet and Nutritional Patterns
Nutrition plays a major role in blood sugar regulation.
Common dietary contributors include:
- High intake of refined carbohydrates
- Sugary beverages
- Ultra-processed foods
- Low fiber intake
- Irregular meal timing
Balanced nutrition supports stable glucose levels and reduces metabolic stress, reinforcing the importance of Nutrition in blood sugar management.
3) Hormonal Imbalances
Several hormones affect blood glucose regulation.
These include:
- Insulin
- Cortisol
- Growth hormone
- Glucagon
- Thyroid hormones
Chronic stress, poor sleep, and endocrine disorders can disrupt these hormones and worsen hyperglycemia.
This is why blood sugar control is closely connected to Hormone Health and Sleep Health.
4) Physical Inactivity
Muscle tissue is one of the body’s largest consumers of glucose.
When physical activity decreases:
- Glucose uptake declines
- Insulin sensitivity worsens
- Blood sugar rises
Regular movement improves glucose utilization and supports long-term metabolic health.
5) Illness, Infection, and Stress
Acute stress and illness can temporarily increase blood sugar.
This happens because stress hormones:
- Increase glucose production
- Reduce insulin sensitivity
- Trigger inflammation
Common triggers include:
- Infections
- Surgery
- Trauma
- Emotional stress
Conditions Associated With High Blood Sugar
Persistent hyperglycemia is linked to a wide range of health conditions.
Metabolic Conditions
- Prediabetes
- Type 2 diabetes
- Metabolic syndrome
- Obesity
- Non-alcoholic fatty liver disease
These conditions reflect underlying dysfunction in Metabolism and long-term energy regulation.
Cardiovascular Conditions
High blood sugar damages blood vessels and increases cardiovascular risk.
Associated conditions include:
- Hypertension
- Atherosclerosis
- Heart disease
- Stroke
This connection highlights the importance of monitoring glucose levels for long-term Heart Health.
Neurological and Cognitive Effects
Chronic hyperglycemia can affect brain function.
Possible effects:
- Brain fog
- Memory problems
- Reduced concentration
- Increased risk of dementia
These changes often overlap with symptoms discussed in Energy & Fatigue and Sleep Health.

Practical Strategies to Reduce High Blood Sugar
These strategies are widely supported by clinical research and public health guidelines.
Improve Dietary Quality
Focus on:
- Whole foods
- High-fiber vegetables
- Lean protein
- Healthy fats
- Low-glycemic carbohydrates
Reduce:
- Added sugars
- Refined grains
- Ultra-processed foods
Dietary changes are among the most effective interventions within Nutrition and metabolic health management.
Increase Physical Activity
Regular exercise helps:
- Improve insulin sensitivity
- Lower blood sugar
- Support weight management
- Reduce inflammation
Recommended baseline:
- At least 150 minutes of moderate activity per week
This supports both Metabolism and sustainable Weight Loss.
Improve Sleep Quality
Poor sleep disrupts glucose regulation and hormone balance.
Sleep deprivation can:
- Increase insulin resistance
- Raise cortisol levels
- Increase appetite
- Reduce energy levels
Optimizing Sleep Health is a foundational step in managing blood sugar.
Manage Stress
Chronic stress elevates cortisol, which increases blood glucose.
Effective stress management strategies include:
- Regular physical activity
- Relaxation techniques
- Structured routines
- Social support
These strategies help stabilize both Hormone Health and metabolic regulation.
Why Recognizing High Blood Sugar Symptoms Matters
Early recognition of hyperglycemia can:
- Prevent progression to diabetes
- Reduce long-term complications
- Protect cardiovascular health
- Improve energy levels
- Support healthy aging
Because blood sugar regulation affects nearly every organ system, identifying symptoms early is one of the most important steps in protecting long-term health.
Hyperglycemia is not just a glucose issue—it is a whole-body metabolic signal.
Final Thoughts
High blood sugar symptoms are often subtle at first but become more serious as metabolic dysfunction progresses. Understanding the warning signs allows individuals to take proactive steps before complications develop.
Blood sugar regulation is deeply interconnected with:
- Metabolism
- Nutrition
- Hormone Health
- Sleep Health
- Energy & Fatigue
- Heart Health
- Gut Health
- Weight Loss
Viewing hyperglycemia through a systems-based lens helps explain why small changes in lifestyle, diet, and daily routines can produce meaningful improvements in long-term health.
FAQ — High Blood Sugar Symptoms
What blood sugar level causes symptoms?
Symptoms often begin when blood glucose rises above:
- 180–200 mg/dL
However, some people may experience symptoms at lower levels, especially if blood sugar rises rapidly.
Can high blood sugar cause fatigue?
Yes. High blood sugar prevents cells from efficiently using glucose for energy, leading to fatigue, weakness, and reduced physical performance.
Is hyperglycemia always caused by diabetes?
No. Hyperglycemia can also result from:
- Stress
- Illness
- Medications
- Hormonal changes
- Poor sleep
- Dietary patterns
However, persistent hyperglycemia should always be evaluated by a healthcare professional.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Centers for Disease Control and Prevention (CDC) – Diabetes
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
World Health Organization (WHO) — Diabetes
American Diabetes Association (ADA)
Nathan DM. “Long-term complications of diabetes mellitus.”
New England Journal of Medicine
American Heart Association — Diabetes and Cardiovascular Risk
International Diabetes Federation — Global Diabetes Overview
