
How Outbreaks Turn Into Epidemics or Pandemics
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Throughout history, humanity has faced recurring waves of infectious disease that have reshaped societies, economies, and public health systems. From localized outbreaks in small communities to global pandemics affecting billions, the transition from a single cluster of cases to widespread transmission is neither random nor mysterious. It follows identifiable biological, environmental, and social dynamics that epidemiologists study carefully.
Understanding how outbreaks evolve into epidemics or pandemics is essential not only for scientists and policymakers but also for the general public. This knowledge helps societies recognize early warning signs, implement timely interventions, and reduce the devastating consequences of uncontrolled disease spread. In the modern era—marked by rapid global travel, urban density, and environmental change—the speed at which infections can escalate has increased dramatically, making preparedness more critical than ever.
This article explores the mechanisms, stages, and risk factors that determine whether an outbreak remains contained or expands into a regional epidemic or a worldwide pandemic.
Understanding the Key Terms: Outbreak, Epidemic, and Pandemic
Before examining the progression of disease spread, it is important to clarify the terminology used in epidemiology. These terms describe the scale and geographic reach of disease transmission rather than the severity of the illness itself.
Outbreak
An outbreak refers to a sudden increase in cases of a disease in a limited geographic area or population group. It may occur in a school, hospital, city, or specific community. Outbreaks are often the earliest detectable stage of infectious disease spread.
Epidemic
An epidemic occurs when disease transmission expands beyond localized clusters and affects a larger population within a region or country. The number of cases rises above what is normally expected for that disease in that area.
Pandemic
A pandemic is an epidemic that spreads across multiple countries or continents, typically affecting a large portion of the global population. Pandemics require sustained human-to-human transmission and widespread geographic distribution.
These distinctions are fundamental in public health decision-making, as the classification of a disease event determines the level of response, resource allocation, and international coordination required.
The Early Stage: How an Outbreak Begins
Most epidemics and pandemics begin with a single introduction of a pathogen into a susceptible population. This introduction can occur through several pathways, including:
- Contact with infected animals (zoonotic transmission)
- Travel-related exposure
- Environmental contamination
- Healthcare-associated transmission
- Food or water contamination
At this stage, the disease may appear limited and manageable. However, several factors determine whether the outbreak will remain contained or escalate.
Key Conditions That Enable an Outbreak
- Presence of a pathogen capable of infecting humans
- Susceptible individuals without immunity
- Efficient transmission pathways
- Environmental conditions that support spread
If any of these elements are absent, the outbreak may fade quickly. When all are present, transmission can accelerate rapidly.
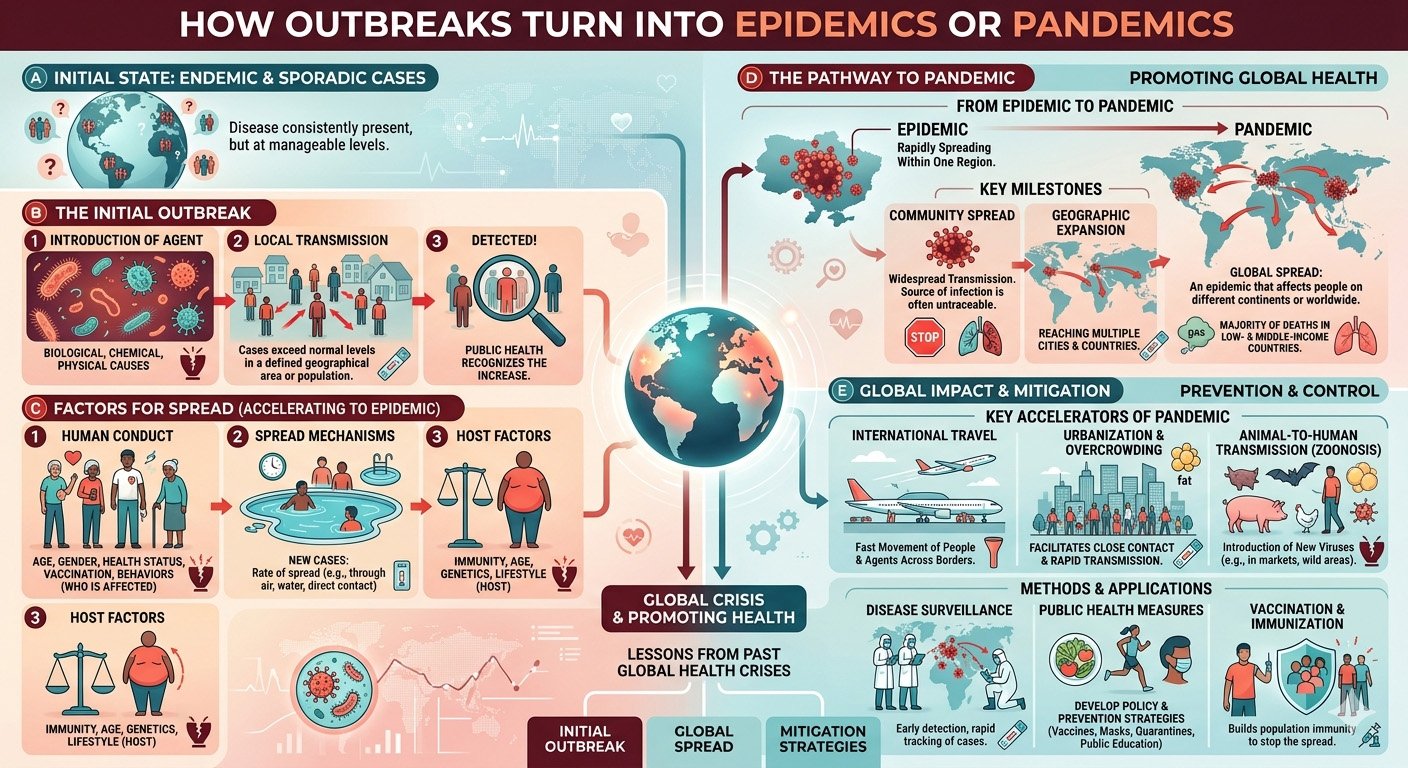
The Role of Transmission Dynamics
One of the most important concepts in epidemiology is how easily a disease spreads from person to person. This is influenced by biological characteristics of the pathogen and behavioral patterns of the population.
Factors That Influence Transmission
Mode of transmission
Diseases transmitted through the air or respiratory droplets spread more easily than those requiring direct contact.
Incubation period
A long incubation period allows infected individuals to travel and interact with others before symptoms appear.
Asymptomatic transmission
When infected individuals show no symptoms but remain contagious, detection becomes more difficult.
Population density
Crowded environments increase contact rates and accelerate disease spread.
Mobility and travel
Modern transportation allows pathogens to move across continents within hours.
These factors interact to determine whether transmission remains localized or expands into wider geographic areas.
The Tipping Point: When an Outbreak Becomes an Epidemic
An outbreak transitions into an epidemic when the number of infections grows consistently over time and spreads beyond the initial location. This transition often occurs when containment measures fail or are implemented too late.
Warning Signs of an Emerging Epidemic
- Rapid increase in case numbers
- Sustained community transmission
- Spread to new geographic regions
- Overwhelmed healthcare systems
- Rising hospitalization rates
Public health surveillance systems are designed to detect these signals early. Timely intervention at this stage can prevent escalation into a pandemic.
How Epidemics Become Pandemics
Not all epidemics become pandemics. For global spread to occur, several additional conditions must be met.
Requirements for a Pandemic
Sustained human-to-human transmission
The pathogen must spread efficiently between people without relying on a specific location or vector.
Global connectivity
International travel enables rapid geographic expansion.
Limited population immunity
If most people lack immunity, transmission continues unchecked.
Delayed detection or response
Slow recognition of the threat allows the disease to spread widely before containment begins.
Pandemics are therefore not only biological events but also logistical and political challenges.
The Role of Globalization in Disease Spread
Modern globalization has transformed the dynamics of infectious disease transmission. Air travel, trade, and urbanization have increased the speed and scale of pathogen movement.
Globalization Factors That Accelerate Spread
International travel
Large urban populations
Global supply chains
Migration and displacement
Climate change
These forces create interconnected systems where a local outbreak can become a global crisis within weeks.
For example, a traveler infected in one country may unknowingly introduce a pathogen into multiple cities before symptoms develop. This pattern has been observed repeatedly in modern pandemics.
Superspreading Events and Their Impact
Some outbreaks escalate rapidly due to superspreading events—situations in which a single individual infects a large number of people in a short period.
Common Settings for Superspreading
- Large gatherings
- Religious events
- Conferences
- Healthcare facilities
- Crowded indoor environments
Superspreading events can dramatically accelerate the transition from outbreak to epidemic by increasing transmission intensity in a short timeframe.
Environmental and Seasonal Influences
Environmental conditions play a significant role in disease transmission. Temperature, humidity, and seasonal patterns can affect both pathogens and human behavior.
Environmental Drivers of Disease Spread
Climate conditions
Rainfall patterns
Air quality
Water availability
Vector populations
For example, mosquito-borne diseases often increase during rainy seasons, while respiratory infections may peak during colder months when people spend more time indoors.
The Importance of Public Health Response
Effective public health interventions can interrupt transmission chains and prevent outbreaks from escalating.
Core Public Health Strategies
Disease surveillance
Testing and diagnosis
Contact tracing
Isolation and quarantine
Vaccination programs
Public communication
Rapid response is the most powerful tool in preventing epidemics and pandemics.
Even small delays in implementing control measures can allow exponential growth in infections.
Lessons from Recent Global Health Events
Recent outbreaks have demonstrated both the vulnerability and resilience of modern societies. They have also highlighted the importance of preparedness, coordination, and transparent communication.
Key Lessons
Early detection saves lives
Public trust is essential
Healthcare capacity matters
Global cooperation is critical
Prevention is more effective than reaction
These lessons continue to shape modern public health strategies and emergency preparedness planning.
Why Some Outbreaks Stay Small
Not every outbreak becomes an epidemic. Many are contained quickly due to effective intervention or unfavorable conditions for transmission.
Factors That Limit Spread
Strong surveillance systems
Rapid isolation of cases
High vaccination coverage
Natural immunity
Geographic barriers
Understanding these protective factors helps public health authorities design strategies to prevent large-scale disease spread.
The Future of Pandemic Prevention
Advances in science and technology are transforming the way societies detect and respond to infectious diseases.
Emerging Tools in Epidemiology
Genomic sequencing
Artificial intelligence modeling
Real-time surveillance systems
Digital contact tracing
Predictive analytics
These innovations allow faster identification of threats and more precise control measures.
However, technology alone is not enough. Preparedness requires sustained investment in healthcare infrastructure, education, and international collaboration.
Conclusion
The transformation of an outbreak into an epidemic or pandemic is driven by a complex interaction of biological, environmental, and social factors. While pathogens initiate disease spread, human behavior, public health systems, and global connectivity determine the scale of impact.
Understanding these dynamics empowers societies to act early, respond effectively, and protect populations from large-scale health crises. In an increasingly interconnected world, vigilance, preparedness, and cooperation remain the most powerful defenses against future pandemics.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
SOURCES:
World Health Organization (WHO)
https://www.who.int
Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov
Johns Hopkins Bloomberg School of Public Health
https://publichealth.jhu.edu
European Centre for Disease Prevention and Control (ECDC)
https://www.ecdc.europa.eu
National Institutes of Health (NIH)
https://www.nih.gov
Harvard T.H. Chan School of Public Health
https://www.hsph.harvard.edu
