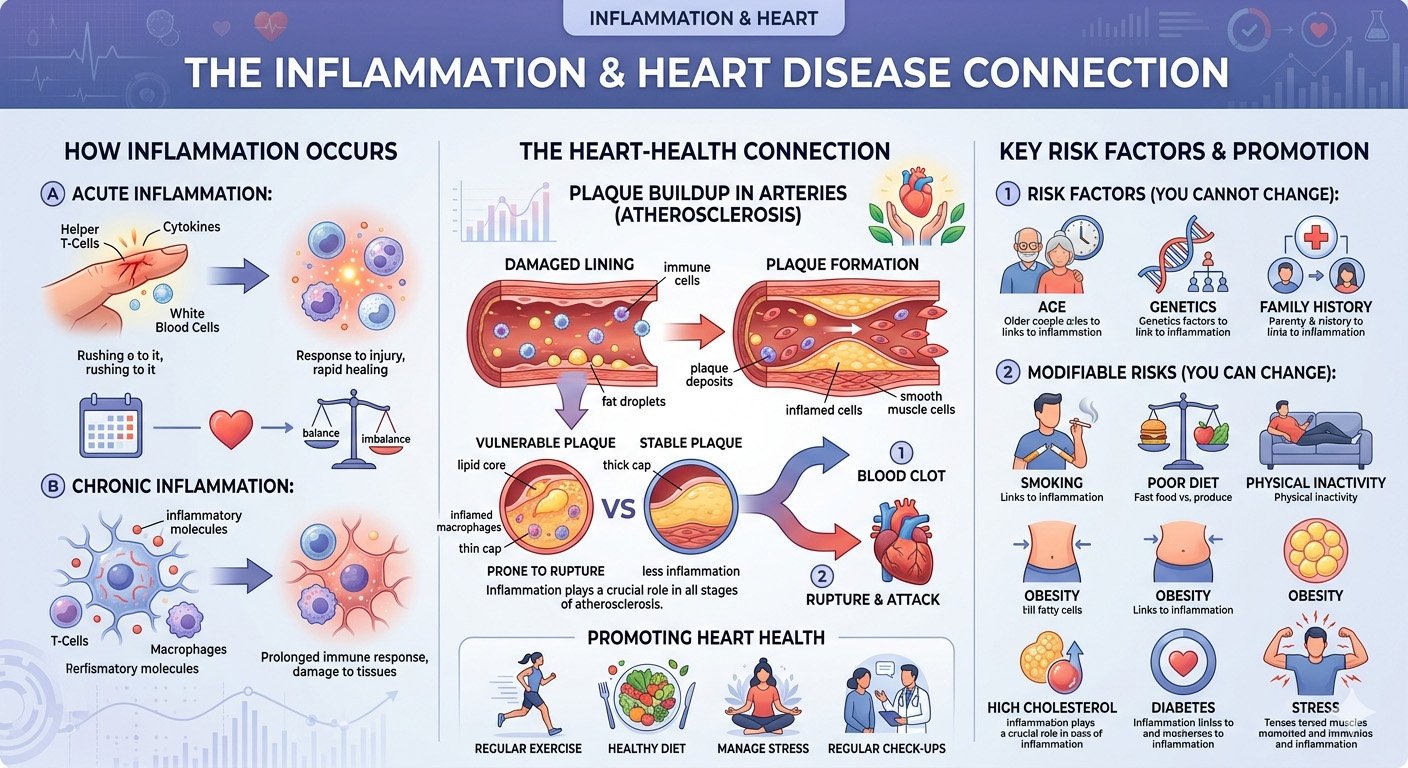
Inflammation and Heart Disease
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Inflammation is a natural part of the body’s immune response, helping protect against infection and injury. However, when inflammation becomes chronic, it can silently damage blood vessels, disrupt metabolic balance, and significantly increase the risk of heart disease. Today, chronic low-grade inflammation is recognized as a central driver of cardiovascular disease worldwide.
The connection between inflammation and heart disease highlights how multiple body systems interact. Persistent inflammation affects Metabolism, Hormone Health, and Blood Sugar, while also influencing blood pressure, cholesterol levels, and vascular function. Because inflammation often develops gradually and without obvious symptoms, understanding its role in cardiovascular health is essential for prevention.
What Is Inflammation?
Inflammation is the body’s protective response to injury, infection, or harmful stimuli. It involves immune cells, signaling molecules, and blood vessels working together to restore tissue health.
There are two main types of inflammation:
Acute Inflammation
Acute inflammation is short-term and protective.
Examples include:
- Healing after injury
- Fighting infection
- Tissue repair
Typical signs may include:
- Redness
- Swelling
- Warmth
- Pain
This type of inflammation usually resolves once the threat is removed.
Chronic Inflammation
Chronic inflammation occurs when the immune response remains active for extended periods.
This form of inflammation can:
- Damage healthy tissues
- Disrupt blood vessel function
- Increase cardiovascular risk
- Promote metabolic dysfunction
Chronic inflammation is strongly linked to conditions discussed in Metabolism and Heart Health.
How Inflammation Contributes to Heart Disease (Physiology)
Inflammation plays a central role in the development of cardiovascular disease, particularly through its effects on blood vessels.
Over time, inflammatory processes can:
- Damage the inner lining of arteries
- Promote plaque buildup
- Increase blood clotting risk
- Narrow blood vessels
- Reduce circulation
These processes contribute to a condition called:
atherosclerosis
Atherosclerosis is the primary cause of heart attacks and strokes.
Inflammation also interacts with metabolic pathways discussed in Blood Sugar and hormonal regulation addressed in Hormone Health.
Damage to Blood Vessel Walls
Inflammation can injure the endothelium — the protective lining of blood vessels.
This damage can lead to:
- Reduced vessel flexibility
- Increased plaque formation
- Increased blood pressure
- Increased cardiovascular risk
Healthy blood vessels depend on metabolic stability discussed in Metabolism.
Plaque Formation and Artery Narrowing
Inflammation promotes the accumulation of cholesterol and immune cells within artery walls.
This buildup forms plaques that:
- Narrow arteries
- Restrict blood flow
- Increase risk of heart attack
These changes are strongly influenced by dietary patterns discussed in Nutrition.
Increased Blood Clotting
Inflammation can increase the body’s tendency to form blood clots.
This response may lead to:
- Blocked arteries
- Heart attack
- Stroke
Clotting risk is closely connected to cardiovascular regulation discussed in Heart Health.
Interaction With Cholesterol
Inflammation affects how cholesterol behaves in the bloodstream.
It can:
- Increase LDL oxidation
- Reduce HDL effectiveness
- Promote plaque instability
These effects increase cardiovascular risk and are closely linked to metabolic regulation discussed in Metabolism.
Common Causes of Chronic Inflammation
Chronic inflammation often results from long-term exposure to lifestyle and environmental factors.
Poor Diet
Diet is one of the strongest drivers of inflammation.
Foods associated with increased inflammation include:
- Ultra-processed foods
- Added sugar
- Refined carbohydrates
- Trans fats
These dietary patterns are closely related to metabolic imbalance discussed in Nutrition.
Obesity
Excess body fat — particularly abdominal fat — produces inflammatory substances that affect the cardiovascular system.
Obesity-related inflammation can:
- Increase blood pressure
- Disrupt hormone balance
- Increase cardiovascular risk
Weight regulation is closely connected to metabolic health discussed in Weight Loss.
Chronic Stress
Persistent stress can increase inflammatory activity through hormonal and nervous system pathways.
Stress-related inflammation may:
- Increase blood pressure
- Increase blood sugar
- Disrupt sleep
- Increase cardiovascular risk
Stress regulation is closely linked to hormone balance discussed in Hormone Health.
Poor Sleep
Sleep deprivation can increase inflammatory markers in the body.
Poor sleep may lead to:
- Increased blood pressure
- Increased insulin resistance
- Increased cardiovascular risk
Sleep patterns strongly influence metabolic regulation discussed in Sleep Health.
Physical Inactivity
Sedentary behavior is associated with increased inflammation.
Regular movement helps:
- Reduce inflammatory markers
- Improve circulation
- Support metabolic health
Physical activity supports cardiovascular protection discussed in Heart Health.
Conditions Linked to Inflammation and Heart Disease
Chronic inflammation contributes to many cardiovascular and metabolic conditions.
Coronary Artery Disease
Inflammation accelerates plaque formation in coronary arteries.
This condition may lead to:
- Chest pain
- Reduced blood flow
- Heart attack
Hypertension (High Blood Pressure)
Inflammation can damage blood vessels and increase vascular resistance.
This can lead to:
- Persistent high blood pressure
- Increased cardiovascular risk
Blood pressure regulation is closely connected to cardiovascular health discussed in Heart Health.
Stroke
Inflammation increases the risk of blood clots and vascular damage.
Stroke risk increases when inflammation is combined with:
- High blood pressure
- High cholesterol
- Diabetes
These risks are closely related to metabolic regulation discussed in Blood Sugar.
Heart Failure
Chronic inflammation can weaken heart muscle over time.
This may result in:
- Reduced pumping ability
- Fluid buildup
- Fatigue
Heart function is closely connected to energy regulation discussed in Energy & Fatigue.
Warning Signs of Chronic Inflammation
Chronic inflammation often develops silently but may produce subtle symptoms.
Common signs include:
- Persistent fatigue
- Joint pain
- Digestive discomfort
- Frequent illness
- Brain fog
- Poor sleep
- Weight gain
These symptoms often overlap with metabolic and energy-related issues discussed in Metabolism.
Practical Strategies to Reduce Inflammation and Protect Heart Health
Reducing inflammation requires consistent lifestyle habits that support metabolic and cardiovascular health.
Eat Anti-Inflammatory Foods
Foods that support inflammation control include:
- Fruits and vegetables
- Whole grains
- Fatty fish
- Nuts and seeds
- Olive oil
These dietary patterns align with guidance discussed in Nutrition.
Maintain a Healthy Body Weight
Healthy weight management can significantly reduce inflammation.
Benefits include:
- Improved blood pressure
- Reduced metabolic strain
- Reduced cardiovascular risk
Weight regulation is closely connected to metabolic balance discussed in Weight Loss.
Stay Physically Active
Regular exercise helps regulate inflammatory responses.
Benefits include:
- Reduced inflammation
- Improved circulation
- Improved metabolic health
Physical activity supports prevention strategies discussed in Heart Health.
Improve Sleep Quality
Sleep supports immune regulation and inflammation control.
Helpful habits include:
- Consistent sleep schedule
- Dark, quiet sleep environment
- Limiting caffeine late in the day
Healthy sleep patterns support recovery discussed in Sleep Health.
Manage Stress
Stress management supports both hormonal and cardiovascular health.
Helpful strategies include:
- Deep breathing
- Physical activity
- Relaxation techniques
Stress regulation supports systems discussed in Hormone Health.
Why Inflammation Matters for Heart Health
Inflammation is now considered a central mechanism in cardiovascular disease. Many heart conditions develop gradually as chronic inflammation damages blood vessels and disrupts metabolic regulation.
Over time, persistent inflammation can lead to:
- Atherosclerosis
- Heart attack
- Stroke
- High blood pressure
- Metabolic dysfunction
Because inflammation affects multiple systems, reducing inflammation supports prevention strategies across Metabolism, Nutrition, Blood Sugar, Hormone Health, and Heart Health.
Final Thoughts
Inflammation is a normal and necessary biological process, but when it becomes chronic, it can significantly increase the risk of heart disease. The connection between inflammation and cardiovascular health highlights the importance of lifestyle habits that support immune balance and metabolic stability.
Small, consistent changes in diet, sleep, physical activity, and stress management can significantly reduce inflammation and protect heart health over time.
Protecting the heart often begins with controlling inflammation.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Medical Institutions
American Heart Association (AHA)
National Institutes of Health (NIH)
Mayo Clinic — Inflammation and Heart Disease
Cleveland Clinic — Inflammation and Cardiovascular Health
Global Organizations
World Health Organization (WHO) — Cardiovascular Disease and Inflammation
Peer-Reviewed Studies
Ridker PM et al.
Inflammation and atherosclerosis
New England Journal of Medicine
Libby P
Inflammation in cardiovascular disease
Nature
Scientific Review
Hansson GK
Inflammation, atherosclerosis, and coronary artery disease
New England Journal of Medicine
