Insulin Resistance: Causes, Symptoms, and How It Affects Metabolic Health
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction
Insulin resistance is one of the most important drivers of modern metabolic disease. It develops gradually and often silently, affecting how the body regulates energy, blood sugar, fat storage, and hormone balance.
Although commonly associated with diabetes, insulin resistance is fundamentally a metabolic dysfunction that can influence multiple systems throughout the body. It is closely connected to Metabolism, dietary patterns in Nutrition, hormonal regulation in Hormone Health, and energy regulation in Energy & Fatigue. Over time, it can also affect cardiovascular risk, digestive health, sleep quality, and body weight.
Understanding insulin resistance is essential not only for preventing disease, but for maintaining long-term metabolic stability and overall health.
What Is Insulin Resistance?
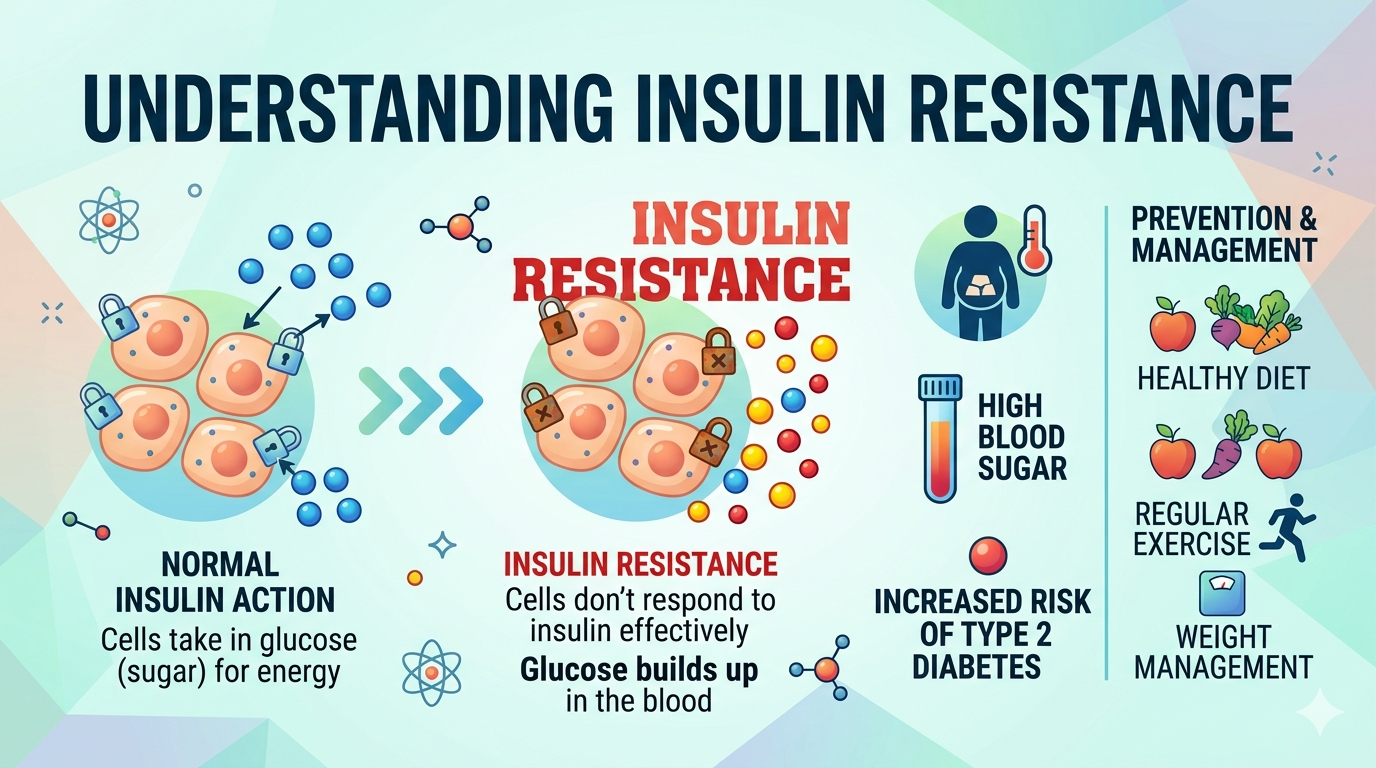
Insulin resistance is a condition in which the body’s cells become less responsive to the hormone insulin, requiring higher levels of insulin to move glucose from the bloodstream into cells.
Insulin is produced by the pancreas and plays a central role in:
- Regulating blood sugar levels
- Storing energy as glycogen or fat
- Controlling fat metabolism
- Supporting normal cellular function
When insulin sensitivity decreases, the body compensates by producing more insulin. Over time, this can lead to chronically elevated insulin levels (hyperinsulinemia), rising blood glucose, and eventually metabolic disease.
Insulin resistance exists on a spectrum and may be present for years before symptoms appear or laboratory values become abnormal.
How Insulin Resistance Works (Physiology)
Under normal conditions, insulin binds to receptors on muscle, fat, and liver cells, triggering a series of signals that allow glucose to enter the cell and be used for energy.
In insulin resistance, this signaling pathway becomes impaired.
Key physiological changes include:
Reduced glucose uptake
Cells do not respond effectively to insulin, leading to higher blood sugar levels and reduced energy availability at the cellular level.
Increased insulin production
The pancreas compensates by releasing more insulin to maintain normal glucose levels.
Increased fat storage
High insulin levels promote fat storage, especially in the abdominal region, linking insulin resistance to Weight Loss challenges and central obesity.
Disrupted metabolic flexibility
The body becomes less efficient at switching between burning carbohydrates and fat, a core feature of impaired Metabolism.
Over time, these changes can lead to:
- Prediabetes
- Type 2 diabetes
- Fatty liver disease
- Cardiovascular disease
Key Factors That Contribute to Insulin Resistance
Insulin resistance rarely develops from a single cause. Instead, it is typically the result of multiple interacting factors involving lifestyle, hormones, and metabolic health.
Poor Dietary Patterns
Frequent consumption of highly processed foods, refined carbohydrates, and added sugars can promote repeated spikes in blood sugar and insulin.
Diet quality plays a major role in Nutrition and directly influences insulin sensitivity.
Common dietary contributors include:
- Excess sugar intake
- Refined grains
- Low fiber consumption
- Ultra-processed foods
- High-calorie diets with low nutrient density
Excess Body Fat (Especially Visceral Fat)
Fat stored around internal organs — known as visceral fat — releases inflammatory molecules and hormones that interfere with insulin signaling.
This type of fat is strongly associated with:
- Metabolic syndrome
- Type 2 diabetes
- Cardiovascular disease
Visceral fat is also closely linked to risk factors discussed in Heart Health.
Physical Inactivity
Muscle tissue plays a major role in glucose uptake. Regular movement improves insulin sensitivity by increasing glucose transport into muscle cells.
Sedentary behavior can reduce insulin responsiveness and contribute to metabolic dysfunction.
Chronic Stress and Hormonal Imbalance
Stress hormones — particularly cortisol — can increase blood sugar levels and promote insulin resistance over time.
Hormonal interactions affecting insulin sensitivity are explored more deeply in Hormone Health.
Poor Sleep and Circadian Disruption
Sleep deprivation and irregular sleep patterns can impair glucose regulation and increase insulin resistance.
Research shows that even short-term sleep restriction can reduce insulin sensitivity.
Sleep-related metabolic regulation is a key topic in Sleep Health.
Chronic Inflammation
Low-grade inflammation interferes with insulin signaling and contributes to metabolic dysfunction.
Inflammation is often influenced by:
- Diet
- Gut health
- Obesity
- Chronic stress
These interactions highlight the connection between insulin resistance and Gut Health.
Conditions Associated With Insulin Resistance
Insulin resistance is not just a risk factor — it is a central mechanism behind many chronic diseases.
Prediabetes and Type 2 Diabetes
Insulin resistance is the primary driver of elevated blood sugar levels and impaired glucose tolerance.
These conditions are discussed in more detail in Blood Sugar.
Metabolic Syndrome
Metabolic syndrome is a cluster of risk factors that commonly occur together:
- High blood pressure
- High blood sugar
- Abdominal obesity
- High triglycerides
- Low HDL cholesterol
This condition significantly increases the risk of cardiovascular disease and stroke.
Non-Alcoholic Fatty Liver Disease (NAFLD)
Excess insulin promotes fat accumulation in the liver, leading to fatty liver disease even in individuals who consume little or no alcohol.
Polycystic Ovary Syndrome (PCOS)
Insulin resistance is a major underlying factor in many cases of PCOS and can disrupt reproductive hormone balance.
Obesity
Insulin resistance and obesity reinforce each other in a cycle:
- Insulin resistance increases fat storage
- Increased fat mass worsens insulin resistance
This relationship explains why insulin regulation is central to sustainable Weight Loss.
Common Signs and Symptoms
Insulin resistance often develops gradually and may not produce obvious symptoms early on.
However, potential signs include:
- Increased abdominal fat
- Fatigue after meals
- Sugar cravings
- Brain fog
- Difficulty losing weight
- Frequent hunger
- Elevated triglycerides
- High fasting insulin or glucose
Persistent fatigue related to blood sugar instability is explored in Energy & Fatigue.

Practical Strategies to Improve Insulin Sensitivity
Insulin resistance is often reversible — especially in its early stages — through consistent lifestyle changes.
Improve Dietary Quality
Focus on whole, nutrient-dense foods that stabilize blood sugar levels.
Helpful dietary patterns include:
- High-fiber vegetables
- Lean protein sources
- Healthy fats
- Whole grains
- Minimally processed foods
Reducing added sugars and refined carbohydrates is one of the most effective dietary interventions in Nutrition.
Increase Physical Activity
Exercise improves insulin sensitivity independently of weight loss.
Effective strategies include:
- Walking after meals
- Resistance training
- Interval training
- Daily movement
Muscle activity helps regulate glucose metabolism and supports overall Metabolism.
Improve Sleep Quality
Consistent sleep patterns support hormone balance and glucose regulation.
Recommended habits include:
- Maintaining a regular sleep schedule
- Limiting screen exposure before bed
- Creating a dark, quiet sleep environment
- Avoiding late-night meals
Sleep optimization is a foundational strategy in Sleep Health.
Manage Stress
Reducing chronic stress helps stabilize cortisol and improve insulin sensitivity.
Effective approaches include:
- Mindfulness practices
- Regular physical activity
- Relaxation techniques
- Structured routines
Stress regulation is an important component of Hormone Health.
Support Gut Health
A healthy gut microbiome can influence inflammation, metabolism, and insulin sensitivity.
Helpful habits include:
- Eating fiber-rich foods
- Consuming fermented foods
- Maintaining dietary diversity
These strategies are discussed more deeply in Gut Health.
Why Insulin Resistance Matters for Long-Term Health
Insulin resistance is one of the strongest predictors of chronic disease worldwide. It plays a central role in the development of:
- Type 2 diabetes
- Cardiovascular disease
- Obesity
- Fatty liver disease
- Hormonal disorders
- Chronic fatigue
- Cognitive decline
Because insulin affects nearly every organ system, impaired insulin signaling can disrupt the body’s ability to regulate energy, maintain stable blood sugar, and protect long-term health.
Addressing insulin resistance early can significantly reduce disease risk and improve overall metabolic resilience.
Final Thoughts
Insulin resistance is not simply a blood sugar issue — it is a systemic metabolic condition that affects energy balance, hormone regulation, fat storage, and cardiovascular health.
Its development is influenced by lifestyle, diet, sleep, stress, and body composition, making it deeply connected to core health systems including Metabolism, Nutrition, Hormone Health, Blood Sugar, and Heart Health.
Understanding how insulin resistance works provides a foundation for preventing chronic disease and supporting long-term metabolic health.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
- American Diabetes Association (ADA)
Insulin Resistance and Prediabetes
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) — NIH
Insulin Resistance & Prediabetes
- Centers for Disease Control and Prevention (CDC)
Insulin Resistance and Diabetes
- World Health Organization (WHO)
Diabetes — Key Facts
- Samuel VT, Shulman GI.
The Pathogenesis of Insulin Resistance: Integrating Signaling Pathways and Substrate Flux
The Journal of Clinical Investigation
- Mayo Clinic
Insulin Resistance
