
Lessons from Past Global Health Crises
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
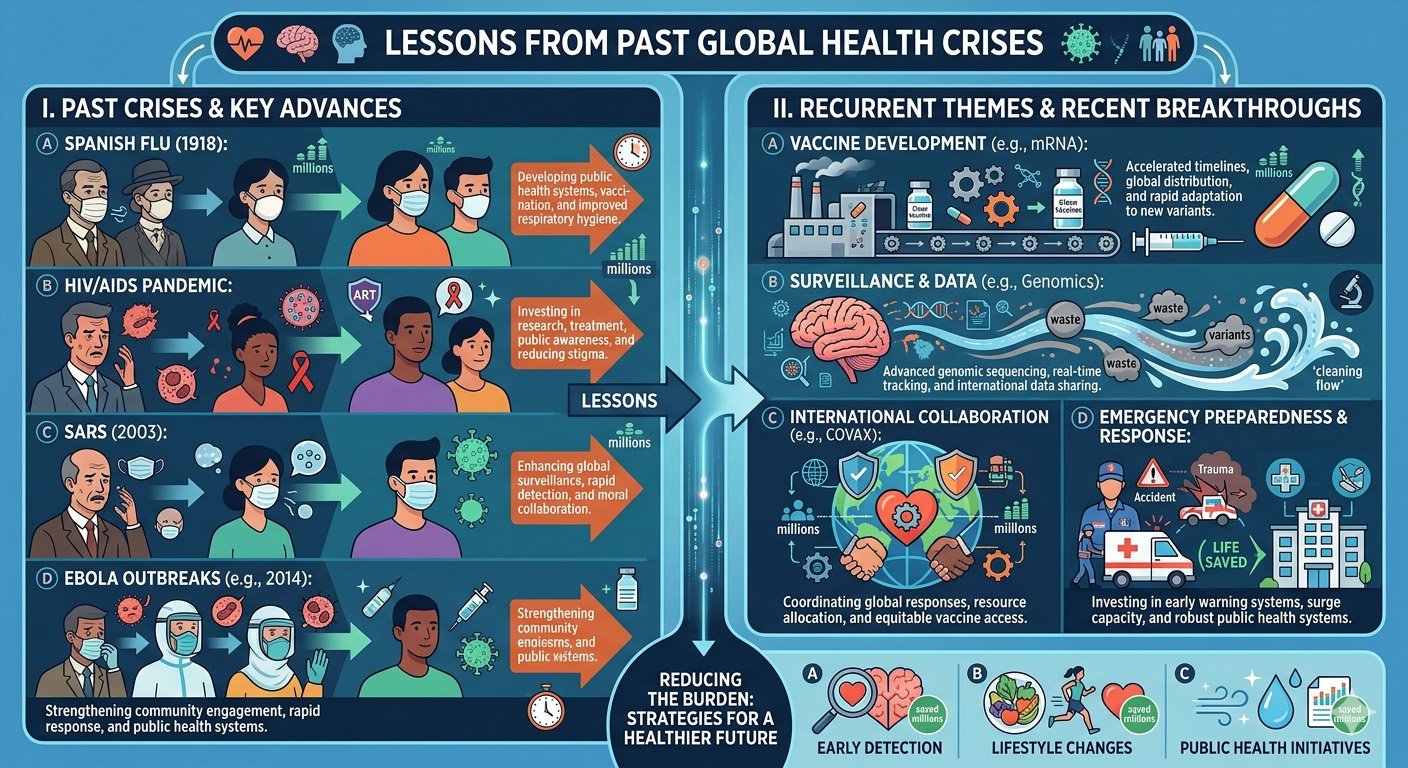
Global health crises have repeatedly reshaped societies, economies, and medical systems. From ancient plagues to modern pandemics, large-scale disease outbreaks have exposed vulnerabilities in public health infrastructure while simultaneously accelerating scientific discovery, policy reform, and international cooperation. Each crisis has left behind lessons—often learned at great human cost—that continue to guide modern responses to emerging health threats.
Understanding these lessons is not merely an academic exercise. It is essential for preparing healthcare systems, governments, and communities to respond effectively to future outbreaks. History shows that survival during health crises depends not only on medical technology but also on communication, trust, coordination, and early action.
Early Detection Saves Lives
One of the most consistent lessons from past health crises is the critical importance of early detection and rapid response. Delays in recognizing outbreaks allow diseases to spread silently, increasing transmission and mortality.
Historically, outbreaks such as cholera, influenza, and emerging viral infections often escalated because early warning signs were missed or underestimated. In contrast, timely surveillance and transparent reporting have repeatedly proven to reduce the scale and severity of epidemics.
Key components of effective early detection include:
- Disease surveillance systems
- Laboratory testing capacity
- Rapid reporting mechanisms
- Data sharing across regions
- Community awareness
Modern epidemiology relies heavily on real-time monitoring of disease patterns. Early identification allows health authorities to implement containment strategies such as isolation, contact tracing, and targeted treatment before widespread transmission occurs.
Public Trust Determines Compliance
Medical interventions alone are not enough to control health crises. Public trust plays a decisive role in determining whether communities follow health guidance.
When populations trust healthcare institutions and government authorities, they are more likely to adopt preventive measures such as vaccination, quarantine, and hygiene practices. Conversely, mistrust can lead to resistance, misinformation, and delayed response.
Historical health crises demonstrate that transparent communication is essential.
Effective communication strategies include:
- Clear and consistent messaging
- Honest acknowledgment of uncertainty
- Cultural sensitivity
- Engagement with community leaders
- Accessible public information
Public trust is not built during a crisis—it is built long before one begins.
Hygiene and Sanitation Are Foundational
Improvements in sanitation and hygiene have saved more lives than many medical treatments.
In the nineteenth and twentieth centuries, the introduction of clean water systems, waste management, and handwashing practices dramatically reduced deaths from infectious diseases such as cholera, typhoid fever, and dysentery.
These interventions demonstrated that disease prevention often depends on environmental conditions rather than clinical care alone.
Fundamental hygiene measures include:
- Safe drinking water
- Proper sewage systems
- Hand hygiene
- Food safety
- Clean healthcare facilities
Even in modern healthcare systems, sanitation remains one of the most effective tools for controlling infection.
Vaccination Is the Most Powerful Preventive Tool
Vaccination has consistently been one of the most effective interventions in reducing mortality during health crises.
Mass vaccination campaigns have prevented millions of deaths and, in some cases, eliminated diseases entirely. The eradication of smallpox is a landmark example of global cooperation and scientific success.
Vaccines work by preparing the immune system to recognize pathogens before exposure, reducing both disease severity and transmission.
Benefits of vaccination programs include:
- Reduced infection rates
- Lower hospitalization rates
- Decreased mortality
- Protection of vulnerable populations
- Prevention of outbreaks
Sustained investment in vaccination infrastructure is essential for maintaining population health.
Healthcare Capacity Determines Outcomes
The ability of healthcare systems to manage patient volume during a crisis significantly influences survival rates.
Hospitals with sufficient staff, equipment, and resources can provide timely care, reducing complications and deaths. Overwhelmed healthcare systems, by contrast, face shortages that compromise patient outcomes.
Critical elements of healthcare capacity include:
- Hospital beds and intensive care units
- Trained healthcare professionals
- Medical supplies and equipment
- Emergency response coordination
- Surge capacity planning
Preparedness planning ensures that healthcare systems can adapt to sudden increases in demand.
Global Cooperation Is Essential
Infectious diseases do not respect borders. International collaboration is therefore essential for controlling global health crises.
Cooperation among countries allows for:
- Shared scientific research
- Coordinated response strategies
- Distribution of medical resources
- Rapid development of treatments and vaccines
- Standardized public health guidelines
Global health organizations play a key role in facilitating cooperation and providing technical guidance.
The interconnected nature of modern travel and trade makes global coordination more important than ever.
Data and Science Guide Effective Policy
Evidence-based decision-making is one of the most important lessons from past health crises.
Policies grounded in scientific data are more effective than those driven by speculation or political pressure. Accurate information allows leaders to assess risk, allocate resources, and implement targeted interventions.
Examples of data-driven tools include:
- Epidemiological modeling
- Case tracking systems
- Mortality analysis
- Risk assessment frameworks
- Public health surveillance
Scientific research continues to inform strategies for disease prevention and treatment.
Protecting Vulnerable Populations Reduces Mortality
Health crises often disproportionately affect vulnerable groups, including older adults, children, individuals with chronic illness, and communities with limited healthcare access.
Protecting these populations is essential for reducing overall mortality.
Protective strategies include:
- Targeted vaccination programs
- Access to medical care
- Nutritional support
- Safe housing conditions
- Social services
Equity in healthcare access is a key factor in improving survival outcomes during crises.
Mental Health Is Part of Crisis Response
Health crises affect not only physical health but also psychological well-being.
Fear, uncertainty, isolation, and economic disruption can increase anxiety, depression, and stress-related conditions. These mental health effects can persist long after the immediate crisis ends.
Integrating mental health services into emergency response plans improves long-term recovery.
Key mental health support strategies include:
- Psychological counseling
- Community support programs
- Stress management resources
- Crisis hotlines
- Social connection initiatives
Recognizing mental health as a core component of public health response is essential for comprehensive care.
Preparedness Reduces Future Risk
Perhaps the most important lesson from past global health crises is the value of preparedness.
Preparedness involves planning, training, and investment before emergencies occur. Countries with established emergency response systems are better equipped to manage outbreaks and protect their populations.
Preparedness measures include:
- Emergency response plans
- Healthcare workforce training
- Stockpiling essential supplies
- Public health education
- Simulation exercises
Preparedness transforms reactive responses into proactive strategies.
The Role of Innovation in Crisis Response
Health crises often accelerate innovation.
Historically, major outbreaks have driven advances in:
- Vaccine development
- Diagnostic testing
- Medical technology
- Public health infrastructure
- Digital health systems
Innovation improves both immediate response and long-term resilience.
Investing in research and development ensures that societies are better prepared for future challenges.
The Core Insight: Crises Reveal Weaknesses—and Drive Progress
Past global health crises have exposed vulnerabilities in healthcare systems while also inspiring breakthroughs that improved survival and resilience. Each crisis has provided lessons about prevention, preparedness, communication, and cooperation.
These lessons remain relevant today. As new health threats emerge, the ability to learn from history will determine how effectively societies protect human life.
Global health crises are not only tests of medical capability—they are tests of collective responsibility, scientific integrity, and social solidarity.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
SOURCES:
World Health Organization (WHO) – Managing Epidemics: Key Facts About Major Deadly Diseases
https://www.who.int/publications/i/item/managing-epidemics-key-facts-about-major-deadly-diseases
Centers for Disease Control and Prevention (CDC) – Pandemic Preparedness and Response
https://www.cdc.gov/globalhealth/healthprotection/fieldupdates/winter-2023/pandemic-preparedness.html
World Bank – Lessons from Past Pandemics
https://www.worldbank.org/en/topic/pandemics
The Lancet – Global Health and Pandemic Preparedness
https://www.thelancet.com/series/global-health-security
Johns Hopkins Bloomberg School of Public Health – Pandemic Lessons and Public Health Response
https://publichealth.jhu.edu/2021/lessons-from-covid-19-pandemic
Our World in Data – Pandemics and Disease History
https://ourworldindata.org/pandemics
