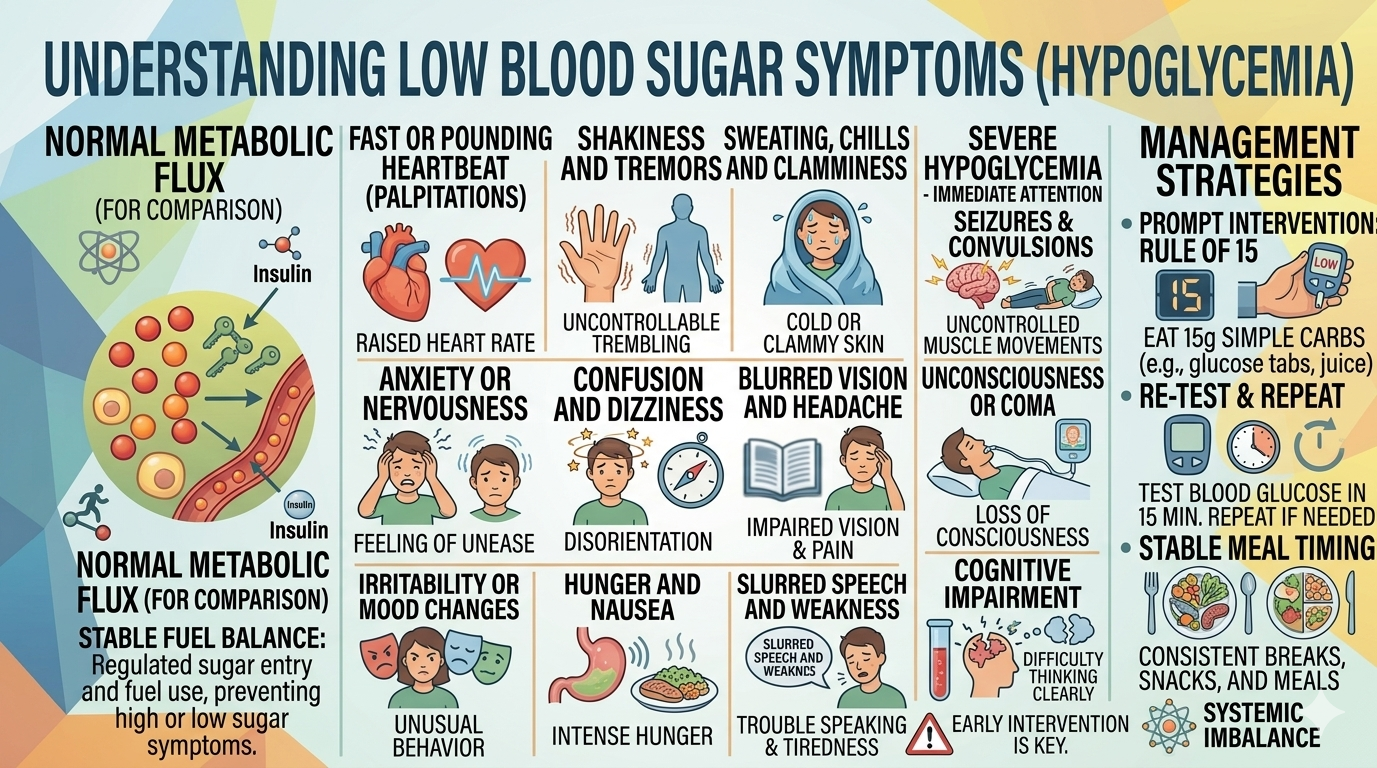
Low Blood Sugar Symptoms (Hypoglycemia)
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction
Blood sugar levels naturally fluctuate throughout the day, but when glucose drops too low, the body can no longer maintain normal energy production. Low blood sugar symptoms, also known as hypoglycemia, can develop quickly and affect multiple systems, including the brain, muscles, and cardiovascular system.
Hypoglycemia is most commonly associated with diabetes treatment, but it can also occur in people without diabetes due to fasting, medication effects, hormonal imbalances, or metabolic dysfunction. Because the brain relies heavily on glucose for fuel, even short episodes of low blood sugar can produce noticeable symptoms.
Understanding the early signs of hypoglycemia is essential for protecting Metabolism, stabilizing Hormone Health, and maintaining consistent energy levels. It also helps prevent dangerous complications and supports long-term regulation of Blood Sugar, Sleep Health, and Energy & Fatigue patterns.
What Is Hypoglycemia?
Hypoglycemia occurs when blood glucose levels fall below the normal physiological range.
Clinically, hypoglycemia is typically defined as:
- Blood glucose below 70 mg/dL
- Severe hypoglycemia may occur below 54 mg/dL
- Symptoms can appear rapidly, especially if levels drop suddenly
Hypoglycemia is most common in:
- People using insulin
- Individuals taking certain diabetes medications
- People with irregular eating patterns
- Those with excessive alcohol intake
- Individuals with endocrine disorders
Maintaining stable glucose levels is essential for healthy Metabolism and continuous energy production.
How Low Blood Sugar Affects the Body (Physiology)
Glucose is the body’s primary fuel, especially for the brain and nervous system. When blood sugar falls too low, the body activates emergency responses to restore balance.
These responses include:
- Release of stress hormones (epinephrine and cortisol)
- Increased heart rate
- Stimulation of hunger signals
- Mobilization of stored glucose from the liver
If glucose levels continue to fall, the brain begins to experience energy deprivation, a condition known as neuroglycopenia.
This can impair:
- Concentration
- Coordination
- Judgment
- Consciousness
Because of these effects, hypoglycemia is closely linked to Energy & Fatigue, neurological function, and overall metabolic stability.
Common Low Blood Sugar Symptoms
Symptoms of hypoglycemia can appear suddenly and may vary in intensity depending on how quickly glucose levels fall.
Early Symptoms
These are the most common warning signs:
- Shakiness or trembling
- Sweating
- Hunger
- Dizziness
- Headache
- Irritability
- Anxiety
- Rapid heartbeat
- Weakness or fatigue
These symptoms are caused by the body’s stress response and are strongly connected to changes in Hormone Health and energy regulation.
Moderate Symptoms
As blood sugar continues to decline, neurological symptoms may develop.
Common moderate symptoms include:
- Confusion
- Difficulty concentrating
- Blurred vision
- Slurred speech
- Poor coordination
- Mood changes
- Tingling sensations
These symptoms reflect reduced glucose availability to the brain and often overlap with issues described in Sleep Health and Energy & Fatigue.
Severe Symptoms (Medical Emergency)
Severe hypoglycemia requires immediate medical attention.
Symptoms may include:
- Loss of consciousness
- Seizures
- Inability to swallow
- Severe confusion
- Coma
These situations are life-threatening and require urgent treatment.
Key Factors That Influence Low Blood Sugar
Hypoglycemia usually results from an imbalance between glucose intake, glucose use, and hormone regulation.
1) Diabetes Medications
The most common cause of hypoglycemia is medication used to lower blood sugar.
Examples include:
- Insulin
- Sulfonylureas
- Certain injectable medications
These medications increase glucose uptake or insulin activity, sometimes lowering blood sugar too much.
This is why careful monitoring of Blood Sugar is essential during treatment.
2) Skipping Meals or Irregular Eating Patterns
When meals are delayed or skipped:
- Glucose intake decreases
- Stored glucose becomes depleted
- Blood sugar drops
This risk increases with:
- Intermittent fasting
- Very low-calorie diets
- Extended physical activity without food
Consistent meal timing supports stable Nutrition and metabolic balance.
3) Excessive Alcohol Consumption
Alcohol can interfere with the liver’s ability to release stored glucose.
This can:
- Reduce blood sugar production
- Increase risk of hypoglycemia
- Mask warning symptoms
Alcohol-related hypoglycemia is especially dangerous during sleep, linking this risk to Sleep Health and overnight glucose regulation.
4) Intense Physical Activity
Exercise increases glucose use by muscles.
If carbohydrate intake is insufficient:
- Blood sugar may fall rapidly
- Energy reserves become depleted
- Hypoglycemia risk increases
Regular physical activity supports healthy Metabolism, but nutrition timing is important to maintain stability.

5) Hormonal Disorders
Certain endocrine conditions can impair glucose regulation.
Examples include:
- Adrenal insufficiency
- Pituitary disorders
- Thyroid dysfunction
These conditions affect Hormone Health and may disrupt normal glucose production.
Conditions Associated With Low Blood Sugar
Hypoglycemia can occur in both short-term and chronic medical conditions.
Metabolic and Endocrine Conditions
- Diabetes
- Prediabetes
- Insulin resistance
- Reactive hypoglycemia
- Hormonal disorders
These conditions reflect changes in Metabolism and glucose regulation.
Neurological and Cognitive Effects
Low blood sugar directly affects brain function.
Possible effects include:
- Brain fog
- Memory problems
- Reduced alertness
- Slowed reaction time
Repeated episodes of hypoglycemia can increase the risk of long-term neurological complications and persistent Energy & Fatigue.
Cardiovascular Effects
Hypoglycemia activates stress hormones that increase heart rate and blood pressure.
Potential effects include:
- Heart rhythm changes
- Increased cardiovascular stress
- Elevated risk of cardiac events in vulnerable individuals
This connection highlights the importance of stable glucose levels for Heart Health.
Practical Strategies to Prevent Low Blood Sugar
Preventing hypoglycemia focuses on stabilizing glucose intake and improving metabolic regulation.
Eat Regular, Balanced Meals
Include:
- Complex carbohydrates
- Protein
- Healthy fats
- Fiber-rich foods
Balanced meals support consistent energy supply and stable Nutrition.
Monitor Blood Sugar Levels
Regular monitoring helps:
- Detect early drops in glucose
- Adjust medication timing
- Prevent severe episodes
This is particularly important for individuals managing diabetes or insulin resistance within the Blood Sugar system.
Adjust Exercise and Meal Timing
Before prolonged physical activity:
- Eat a balanced snack
- Monitor glucose levels
- Stay hydrated
This supports safe physical activity while maintaining stable Metabolism.
Improve Sleep and Recovery
Sleep affects hormone balance and glucose regulation.
Poor sleep can:
- Increase stress hormone levels
- Disrupt glucose stability
- Increase risk of nighttime hypoglycemia
Optimizing Sleep Health helps maintain consistent metabolic function.
Manage Stress
Stress hormones can influence glucose production and insulin activity.
Effective stress management supports:
- Stable glucose regulation
- Improved energy balance
- Better hormone function
This reinforces the connection between hypoglycemia and Hormone Health.
Why Recognizing Low Blood Sugar Symptoms Matters
Recognizing hypoglycemia early can:
- Prevent medical emergencies
- Reduce risk of injury
- Improve daily functioning
- Protect brain health
- Support long-term metabolic stability
Because the brain depends on glucose for energy, maintaining stable blood sugar is essential for both short-term safety and long-term health.
Hypoglycemia is not simply a temporary inconvenience—it is a signal of metabolic imbalance.
Final Thoughts
Low blood sugar symptoms can develop quickly and may become dangerous if not recognized and treated promptly. Understanding the warning signs allows individuals to respond early and maintain stable glucose levels.
Blood sugar regulation depends on the coordinated function of:
- Metabolism
- Nutrition
- Hormone Health
- Sleep Health
- Energy & Fatigue
- Heart Health
- Gut Health
- Weight Loss
Viewing hypoglycemia as part of a broader metabolic system helps explain why consistent nutrition, sleep, and lifestyle habits are essential for maintaining long-term health.
FAQ — Low Blood Sugar Symptoms
What blood sugar level is considered low?
Hypoglycemia is generally defined as:
- Below 70 mg/dL
Severe hypoglycemia may occur below:
- 54 mg/dL
Can low blood sugar happen without diabetes?
Yes. Hypoglycemia can occur in people without diabetes due to:
- Skipping meals
- Alcohol consumption
- Hormonal disorders
- Certain medications
- Intense exercise
How quickly can hypoglycemia develop?
Symptoms can appear within minutes, especially if glucose levels fall rapidly.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Centers for Disease Control and Prevention (CDC)
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
World Health Organization (WHO) — Diabetes
American Diabetes Association (ADA)
Cryer PE. “Hypoglycemia in Diabetes.”
New England Journal of Medicine
International Diabetes Federation — Global Diabetes Overview
American Heart Association — Blood Sugar and Cardiovascular Health
