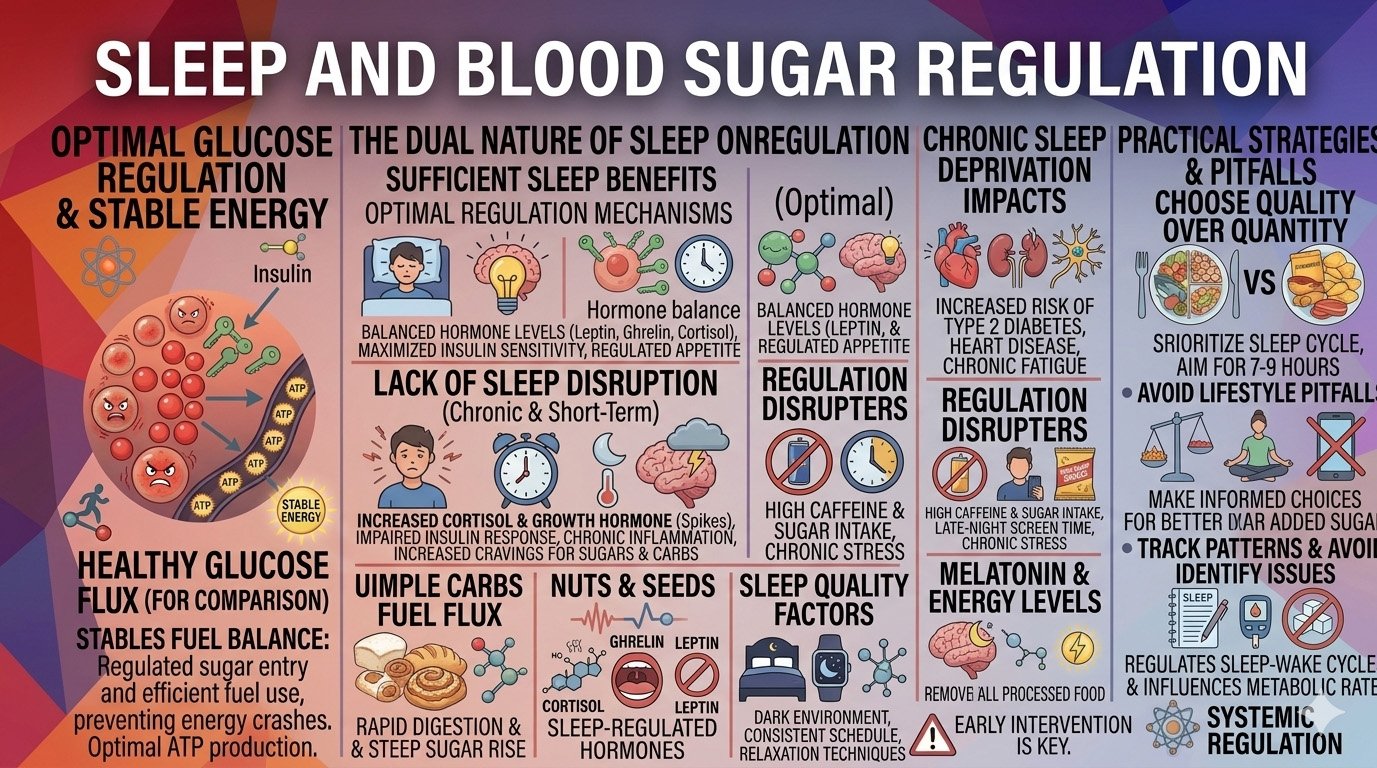
Sleep and Blood Sugar Regulation
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction: The Overlooked Connection Between Sleep and Metabolic Health
Sleep is not just a period of rest—it is a critical biological process that regulates hormones, metabolism, and blood sugar. During sleep, the body restores energy balance, adjusts hormone levels, and prepares cells to respond effectively to insulin. When sleep is disrupted or insufficient, blood sugar regulation becomes less efficient, increasing the risk of fatigue, weight gain, and metabolic disease.
This relationship connects directly to Metabolism, Hormone Health, and Nutrition, as well as daily energy patterns, appetite control, and cardiovascular health. In recent years, researchers have identified poor sleep as a major risk factor for insulin resistance and type 2 diabetes, even in otherwise healthy individuals.
Understanding how sleep influences blood sugar regulation helps explain why consistent, high-quality sleep is a foundational pillar of metabolic health.
What Is Blood Sugar Regulation During Sleep?
Blood sugar regulation refers to the body’s ability to maintain stable glucose levels throughout the day and night. During sleep, the body continues to manage glucose using hormones that control energy production, storage, and release.
Healthy overnight blood sugar regulation typically includes:
- Stable glucose levels during sleep
- Balanced hormone activity
- Efficient insulin response
- Controlled appetite the next day
- Consistent energy levels
When sleep is disrupted, these processes can become unstable, leading to increased hunger, fatigue, and higher blood sugar levels.
This is why sleep is considered a core component of both Blood Sugar management and long-term Energy & Fatigue regulation.
How Sleep Regulates Blood Sugar (Physiology)
Sleep affects blood sugar through multiple hormonal and metabolic mechanisms.
1) Insulin Sensitivity
During normal sleep, cells become more responsive to insulin, allowing glucose to enter cells efficiently.
Poor sleep can:
- Reduce insulin sensitivity
- Increase blood sugar levels
- Promote insulin resistance
- Increase diabetes risk
Research shows that even one night of sleep deprivation can significantly impair glucose metabolism.
2) Cortisol Regulation
Cortisol is a stress hormone that raises blood sugar to provide energy.
Healthy sleep helps:
- Lower nighttime cortisol
- Maintain hormonal balance
- Stabilize glucose levels
Sleep deprivation can lead to:
- Elevated cortisol
- Increased glucose production
- Blood sugar instability
This connection highlights the role of Hormone Health in metabolic regulation.
3) Appetite Hormones: Ghrelin and Leptin
Sleep influences hunger and fullness signals.
Poor sleep increases:
- Ghrelin (hunger hormone)
And decreases:
- Leptin (satiety hormone)
This hormonal shift can lead to:
- Increased appetite
- Sugar cravings
- Overeating
- Weight gain
These effects are closely tied to Weight Loss and long-term metabolic health.
4) Circadian Rhythm and Glucose Control
The body’s internal clock, known as the circadian rhythm, regulates when hormones are released and how the body processes glucose.
Irregular sleep schedules can disrupt:
- Insulin release
- Glucose metabolism
- Energy production
Maintaining consistent sleep timing supports both Sleep Health and blood sugar stability.

Common Sleep Problems That Affect Blood Sugar
Several sleep disorders are strongly associated with poor glucose regulation.
Sleep Deprivation
Defined as regularly getting less than the recommended amount of sleep.
Typical threshold:
Less than 7 hours per night for adults.
Effects on blood sugar:
- Reduced insulin sensitivity
- Increased glucose levels
- Increased hunger
- Fatigue and low energy
Sleep deprivation is one of the most common contributors to metabolic imbalance.
Sleep Apnea
A condition characterized by repeated pauses in breathing during sleep.
Effects:
- Oxygen disruption
- Increased stress hormones
- Elevated blood sugar
- Increased risk of diabetes
Sleep apnea is strongly linked to both obesity and insulin resistance.
This condition also increases risk for poor Heart Health.
Poor Sleep Quality
Even when total sleep time is adequate, poor sleep quality can disrupt glucose regulation.
Examples:
- Frequent awakenings
- Restless sleep
- Insomnia
- Nighttime stress
Poor sleep quality can lead to:
- Hormonal imbalance
- Increased fatigue
- Blood sugar instability
Signs That Sleep May Be Affecting Blood Sugar
People often overlook sleep as a cause of metabolic symptoms.
Common signs include:
- Morning fatigue
- Sugar cravings
- Difficulty losing weight
- Brain fog
- Increased hunger
- Afternoon energy crashes
These symptoms frequently overlap with issues in Energy & Fatigue regulation.
Long-Term Health Risks of Poor Sleep and Blood Sugar Imbalance
Chronic sleep disruption is associated with several metabolic and cardiovascular conditions.
These include:
- Insulin resistance
- Type 2 diabetes
- Obesity
- Metabolic syndrome
- Hypertension
- Cardiovascular disease
Research increasingly shows that sleep duration and quality are independent risk factors for metabolic disease.
This relationship underscores the connection between sleep, Metabolism, and long-term health outcomes.
Practical Strategies to Improve Sleep and Support Blood Sugar Regulation
These strategies are supported by clinical research and behavioral health guidelines.
Maintain a Consistent Sleep Schedule
Going to bed and waking up at the same time daily helps regulate the body’s internal clock.
Benefits:
- Improved hormone balance
- Stable glucose regulation
- Better energy levels
Limit Late-Night Eating
Eating late at night can disrupt glucose control.
Try to:
Finish meals:
2–3 hours before bedtime.
This supports healthy blood sugar regulation and improves sleep quality.
Reduce Evening Screen Exposure
Blue light from screens can interfere with melatonin production.
Reducing screen time before bed helps:
- Improve sleep onset
- Support hormonal balance
- Stabilize blood sugar
Create a Sleep-Friendly Environment
Healthy sleep environments include:
- Dark room
- Cool temperature
- Quiet setting
- Comfortable bedding
These factors improve sleep quality and metabolic regulation.
Manage Stress
Chronic stress disrupts both sleep and blood sugar regulation.
Helpful strategies:
- Relaxation techniques
- Regular physical activity
- Mindfulness practices
- Time management
Stress management supports Hormone Health and metabolic balance.
Why Sleep Is a Core Pillar of Blood Sugar Control
Many people focus on diet and exercise but underestimate the role of sleep.
Sleep affects:
- Insulin sensitivity
- Hormone balance
- Appetite regulation
- Energy production
- Glucose metabolism
Without adequate sleep, even healthy diet and exercise habits may not fully stabilize blood sugar.
This is why sleep is considered one of the three foundational pillars of metabolic health:
- Nutrition
- Physical activity
- Sleep
Final Thoughts: Stable Sleep Supports Stable Blood Sugar
Sleep is not optional for metabolic health—it is essential.
Consistent, high-quality sleep supports:
- Stable blood sugar
- Balanced hormones
- Sustained energy
- Healthy body weight
- Reduced disease risk
Understanding the relationship between Sleep Health, Blood Sugar, Metabolism, and Hormone Health provides a powerful framework for improving both daily performance and long-term health.
FAQ
Can poor sleep raise blood sugar?
Yes. Sleep deprivation can reduce insulin sensitivity and increase glucose levels, even in healthy individuals.
How many hours of sleep are needed for blood sugar control?
Most adults need:
7 to 9 hours per night.
Does sleep affect insulin resistance?
Yes. Chronic sleep deprivation is strongly associated with increased insulin resistance.
Can improving sleep lower blood sugar?
Improving sleep quality can significantly improve glucose regulation, especially when combined with healthy diet and physical activity.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Centers for Disease Control and Prevention (CDC)
Sleep and Chronic Disease
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
American Diabetes Association (ADA)
Sleep and Blood Glucose Control
Spiegel K et al.
Sleep Loss: A Novel Risk Factor for Insulin Resistance and Type 2 Diabetes
The Lancet
Tasali E et al.
Sleep Restriction and Glucose Metabolism
Journal of Clinical Endocrinology & Metabolism
Reutrakul S, Van Cauter E
Sleep Influences on Obesity, Insulin Resistance, and Risk of Type 2 Diabetes
Nature Reviews Endocrinology
