
Sleep and Mental Health: How Sleep Regulates Brain Function and Emotional Stability
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Sleep is not merely a period of rest—it is an active biological process essential for brain regulation, emotional balance, cognitive performance, and long-term mental health. Modern neuroscience increasingly shows that sleep functions as a nightly maintenance cycle for the brain, influencing memory consolidation, emotional processing, hormonal balance, and resilience to stress. When sleep is disrupted, the brain’s regulatory systems begin to destabilize, often leading to anxiety, mood disorders, impaired decision-making, and reduced emotional control.
In the context of mental health, sleep acts as a stabilizing force. It regulates neurotransmitters, restores neural circuits, and recalibrates the emotional centers of the brain. Without sufficient or high-quality sleep, even psychologically healthy individuals can experience irritability, emotional volatility, reduced concentration, and decreased motivation. Over time, chronic sleep deprivation becomes not just a symptom of mental health disorders—but a contributing cause.
The Brain During Sleep: A Nightly Reset Mechanism
Sleep is a structured neurological process composed of repeating cycles that include both non-REM (NREM) and REM sleep. Each stage serves a distinct function in maintaining brain health and emotional stability.
During deep sleep (slow-wave sleep), the brain performs physical restoration and metabolic cleanup. The glymphatic system—often described as the brain’s waste clearance network—removes neurotoxic byproducts that accumulate during waking hours. These include proteins associated with neurodegenerative diseases and cognitive decline.
REM sleep, by contrast, plays a central role in emotional regulation and memory integration. During this stage, the brain processes emotionally charged experiences, reduces emotional intensity, and reorganizes memories into long-term storage.
This nightly reset allows individuals to wake up with improved emotional balance and cognitive clarity. When REM sleep is reduced or fragmented, emotional reactivity increases, and the brain becomes less capable of managing stress.
Emotional Regulation and the Role of Sleep
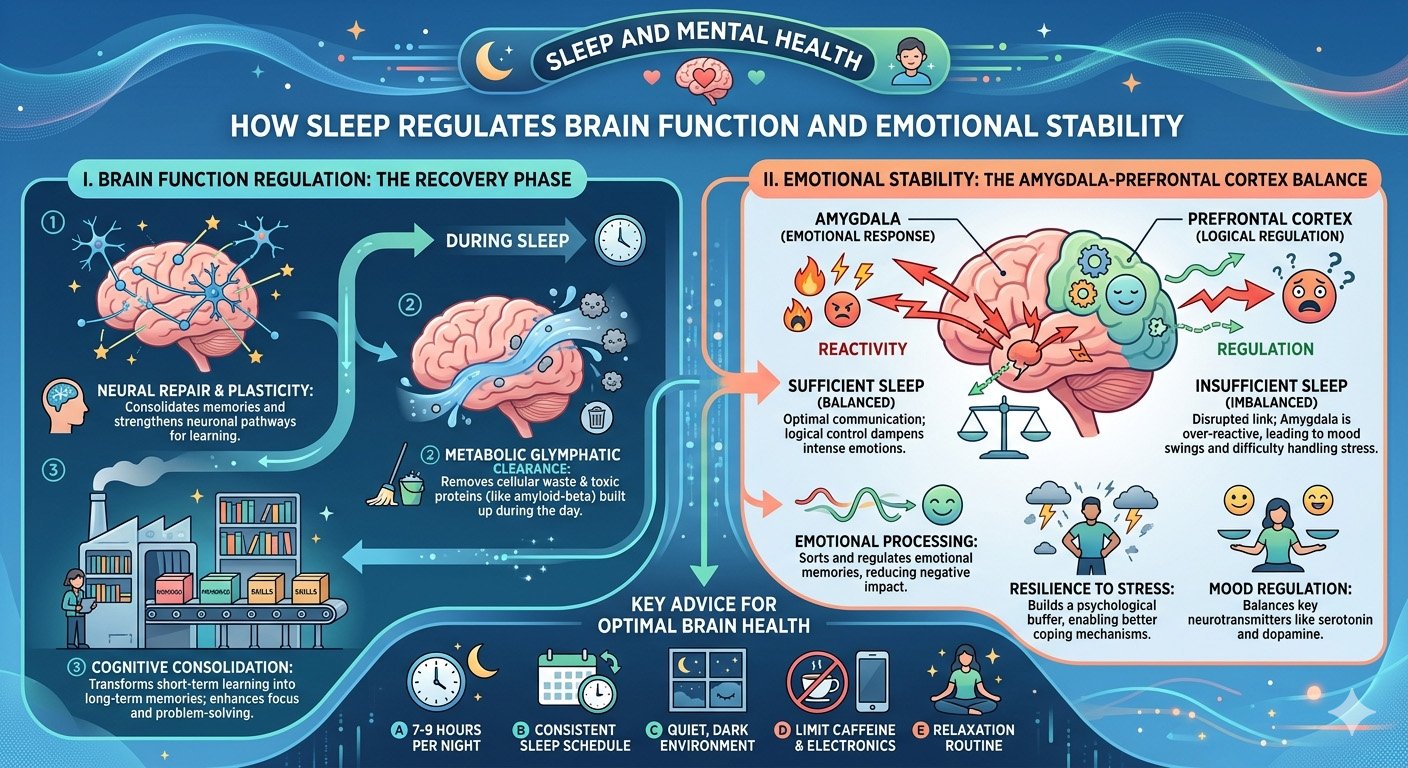
One of the most important functions of sleep is its ability to regulate the emotional centers of the brain, particularly the amygdala and prefrontal cortex.
The amygdala is responsible for detecting threats and generating emotional responses such as fear and anxiety. The prefrontal cortex, on the other hand, acts as a regulatory system that controls impulses, evaluates risks, and moderates emotional reactions.
Sleep strengthens the communication between these regions.
When sleep is adequate:
- Emotional reactions are more controlled
- Stress tolerance increases
- Mood stability improves
- Decision-making becomes more rational
- Social interactions become more balanced
When sleep is insufficient:
- Emotional responses become exaggerated
- Anxiety sensitivity increases
- Irritability rises
- Risk-taking behavior becomes more likely
- Emotional resilience declines
Neuroimaging studies show that sleep deprivation can increase amygdala reactivity by up to 60%, meaning the brain becomes significantly more reactive to negative stimuli. This helps explain why sleep loss often leads to heightened emotional sensitivity and reduced patience.
Sleep and Anxiety: A Bidirectional Relationship
Sleep and anxiety influence each other in a continuous feedback loop. Poor sleep increases physiological arousal and stress hormone levels, while anxiety makes it harder to fall asleep and remain asleep.
This relationship is known as a bidirectional cycle.
Sleep deprivation increases:
- Cortisol (stress hormone) levels
- Heart rate variability instability
- Cognitive rumination
- Hypervigilance
- Sensitivity to perceived threats
These changes create a neurological state that resembles chronic stress. Over time, the brain begins to expect danger even in safe environments, reinforcing anxiety patterns.
Conversely, improving sleep quality often leads to measurable reductions in anxiety symptoms—even without medication. This is why sleep stabilization is frequently one of the first interventions used in mental health treatment.
Sleep and Depression: A Core Biological Connection
Sleep disturbance is one of the strongest predictors of depression. In many cases, insomnia appears months before depressive symptoms fully develop.
Research shows that individuals with chronic insomnia have a significantly higher risk of developing major depressive disorder compared to those with normal sleep patterns.
Several biological mechanisms explain this connection:
- Neurotransmitter imbalance
Sleep regulates serotonin, dopamine, and norepinephrine—chemicals essential for mood stability. - Circadian rhythm disruption
The body’s internal clock controls sleep-wake cycles, hormone release, and energy levels. - Reduced emotional processing
Without adequate REM sleep, the brain struggles to process negative experiences. - Increased inflammation
Sleep deprivation triggers inflammatory responses linked to depression.
Because of this, treating sleep problems is often a critical step in managing depressive disorders.
Cognitive Function, Memory, and Mental Clarity
Sleep plays a foundational role in learning, concentration, and decision-making. During sleep, the brain consolidates information acquired during the day and strengthens neural connections.
This process supports:
- Memory retention
- Problem-solving ability
- Attention and focus
- Creativity
- Cognitive flexibility
Even moderate sleep deprivation can impair cognitive performance in ways comparable to alcohol intoxication.
Common cognitive effects of poor sleep include:
- Slower reaction time
- Reduced concentration
- Forgetfulness
- Poor judgment
- Mental fatigue
For individuals working in demanding cognitive environments—or managing complex projects—sleep quality directly affects productivity, planning ability, and strategic thinking. In practice, sleep functions as a performance multiplier for the brain.
The Stress Response System and Sleep
Sleep regulates the body’s stress response system, particularly the hypothalamic-pituitary-adrenal (HPA) axis.
This system controls:
- Cortisol production
- Energy regulation
- Immune response
- Emotional reactivity
When sleep is disrupted, cortisol levels remain elevated for longer periods, keeping the body in a persistent state of alertness. This state is biologically similar to chronic stress and can lead to emotional exhaustion and burnout.
Over time, chronic sleep disruption can contribute to:
- Anxiety disorders
- Depression
- Burnout
- Mood instability
- Reduced resilience to stress
Sleep, therefore, acts as a nightly reset for the stress response system.
Circadian Rhythms and Mental Health Stability
The circadian rhythm is the body’s internal biological clock, regulating sleep timing, hormone release, body temperature, and energy cycles.
This rhythm is primarily controlled by light exposure.
When circadian rhythms become misaligned—due to irregular schedules, shift work, excessive screen time, or late-night stimulation—the brain struggles to maintain emotional stability.
Circadian disruption is associated with:
- Mood disorders
- Seasonal depression
- Anxiety
- Insomnia
- Cognitive fatigue
Maintaining a consistent sleep schedule is one of the most effective ways to stabilize circadian rhythms and protect mental health.
Long-Term Consequences of Chronic Sleep Deprivation
Short-term sleep loss affects mood and cognition. Long-term sleep deprivation affects brain structure and mental health outcomes.
Chronic insufficient sleep is associated with:
- Increased risk of depression
- Anxiety disorders
- Emotional dysregulation
- Burnout
- Cognitive decline
- Neurodegenerative disease risk
Sleep deprivation also reduces the brain’s ability to recover from stress, making individuals more vulnerable to emotional exhaustion and psychological instability.
In mental health research, sleep is increasingly recognized as a foundational biological requirement—not a lifestyle preference.
Signs That Sleep Is Affecting Mental Health
Sleep-related mental health problems often develop gradually. Early warning signs may include:
- Persistent fatigue despite adequate time in bed
- Difficulty concentrating
- Increased irritability
- Emotional sensitivity
- Anxiety at night
- Waking frequently during sleep
- Feeling unrefreshed in the morning
- Reduced motivation
Recognizing these signs early allows for intervention before more severe mental health symptoms develop.
Strategies That Improve Both Sleep and Mental Health
Small changes in sleep habits can produce significant improvements in emotional stability and cognitive function.
Evidence-based strategies include:
Maintain a consistent sleep schedule
Go to bed and wake up at the same time every day.
Limit screen exposure before bedtime
Blue light delays melatonin production and disrupts sleep timing.
Create a stable sleep environment
A quiet, dark, and cool room improves sleep quality.
Reduce late caffeine intake
Caffeine can remain active in the body for several hours.
Get morning light exposure
Natural light helps regulate circadian rhythms.
Manage stress before bedtime
Relaxation routines reduce physiological arousal.
These interventions are often more effective than expected because sleep influences nearly every system involved in mental health.
The Core Insight: Sleep Is a Biological Regulator of Emotional Stability
Sleep is not simply rest—it is regulation.
Each night, the brain recalibrates emotional responses, restores cognitive function, stabilizes neurotransmitters, and resets the stress response system. When sleep is consistent and restorative, mental health becomes more resilient. When sleep is disrupted, emotional stability becomes fragile.
In modern mental health science, sleep is increasingly viewed as a foundational pillar—alongside nutrition, physical activity, and social connection. Protecting sleep is not just about feeling rested. It is about maintaining the biological systems that support emotional balance, clear thinking, and psychological resilience.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
National Institute of Mental Health (NIMH) – Sleep and Mental Health
National Sleep Foundation – Sleep and Mental Health
Harvard Medical School – Division of Sleep Medicine
Centers for Disease Control and Prevention (CDC) – Sleep and Sleep Disorders
