
Stress, Cortisol, and Heart Disease
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Stress is a normal biological response that helps the body adapt to challenges. However, when stress becomes chronic, it can disrupt hormone balance, elevate inflammation, impair metabolism, and place continuous strain on the cardiovascular system.
At the center of this process is cortisol, the body’s primary stress hormone. While cortisol is essential for survival, persistently elevated levels can contribute to high blood pressure, insulin resistance, inflammation, and vascular damage — all major drivers of heart disease.
Understanding the relationship between stress, cortisol, and cardiovascular health reveals how deeply connected the body’s systems are, particularly Hormone Health, Metabolism, Blood Sugar, and Sleep Health.
What Is Cortisol?
Cortisol is a steroid hormone produced by the adrenal glands in response to physical or psychological stress. It is regulated by the hypothalamic-pituitary-adrenal (HPA) axis — a central hormone system that helps the body maintain stability during stress.
Cortisol plays essential roles in:
- Regulating blood pressure
- Controlling inflammation
- Managing blood sugar levels
- Supporting energy production
- Maintaining immune function
- Coordinating the stress response
In healthy conditions, cortisol follows a predictable daily rhythm:
- Highest in the morning
- Gradually declines throughout the day
- Lowest at night
Disruptions to this rhythm — especially chronically elevated cortisol — are strongly associated with cardiovascular risk and metabolic dysfunction discussed in Metabolism and Hormone Health.
How Stress and Cortisol Affect the Heart (Physiology)
Chronic stress activates the body’s stress response system continuously, leading to sustained cortisol release. Over time, this creates physiological changes that increase cardiovascular strain.
1) Increased Blood Pressure
Cortisol raises blood pressure by increasing vascular tone and enhancing the body’s sensitivity to adrenaline.
Chronic elevation can lead to:
- Persistent hypertension
- Increased arterial stiffness
- Higher cardiovascular workload
- Increased risk of stroke and heart disease
High blood pressure is one of the strongest predictors of cardiovascular disease and is closely linked to long-term stress exposure.
This mechanism connects directly to Heart Health and long-term vascular integrity.
2) Increased Inflammation
Although cortisol normally reduces inflammation, chronic stress can lead to cortisol resistance, where immune cells become less responsive to the hormone.
This results in:
- Persistent low-grade inflammation
- Endothelial dysfunction
- Plaque formation in arteries
- Increased risk of atherosclerosis
Inflammation is a central mechanism linking stress to cardiovascular disease and metabolic dysfunction discussed in Gut Health and Metabolism.
3) Disrupted Blood Sugar Regulation
Cortisol increases glucose production in the liver to provide energy during stress. When stress is prolonged, this mechanism becomes harmful.
Chronic cortisol elevation can lead to:
- Insulin resistance
- Elevated fasting blood sugar
- Increased risk of type 2 diabetes
- Increased cardiovascular risk
This connection makes stress a major contributor to metabolic dysfunction addressed in Blood Sugar and Weight Loss.
4) Increased Heart Rate and Sympathetic Activation
Stress activates the sympathetic nervous system — the body’s “fight-or-flight” system.
This leads to:
- Increased heart rate
- Reduced heart rate variability
- Increased oxygen demand
- Reduced cardiovascular recovery
Persistent sympathetic activation is strongly associated with cardiovascular disease and chronic fatigue patterns discussed in Energy & Fatigue.
5) Disrupted Sleep and Recovery
Chronic stress and elevated cortisol can interfere with sleep regulation, particularly by suppressing melatonin and delaying sleep onset.
Poor sleep further increases:
- Blood pressure
- Inflammation
- Hormonal imbalance
- Cardiovascular strain
This creates a feedback loop between stress and poor sleep that directly affects Sleep Health and cardiovascular risk.
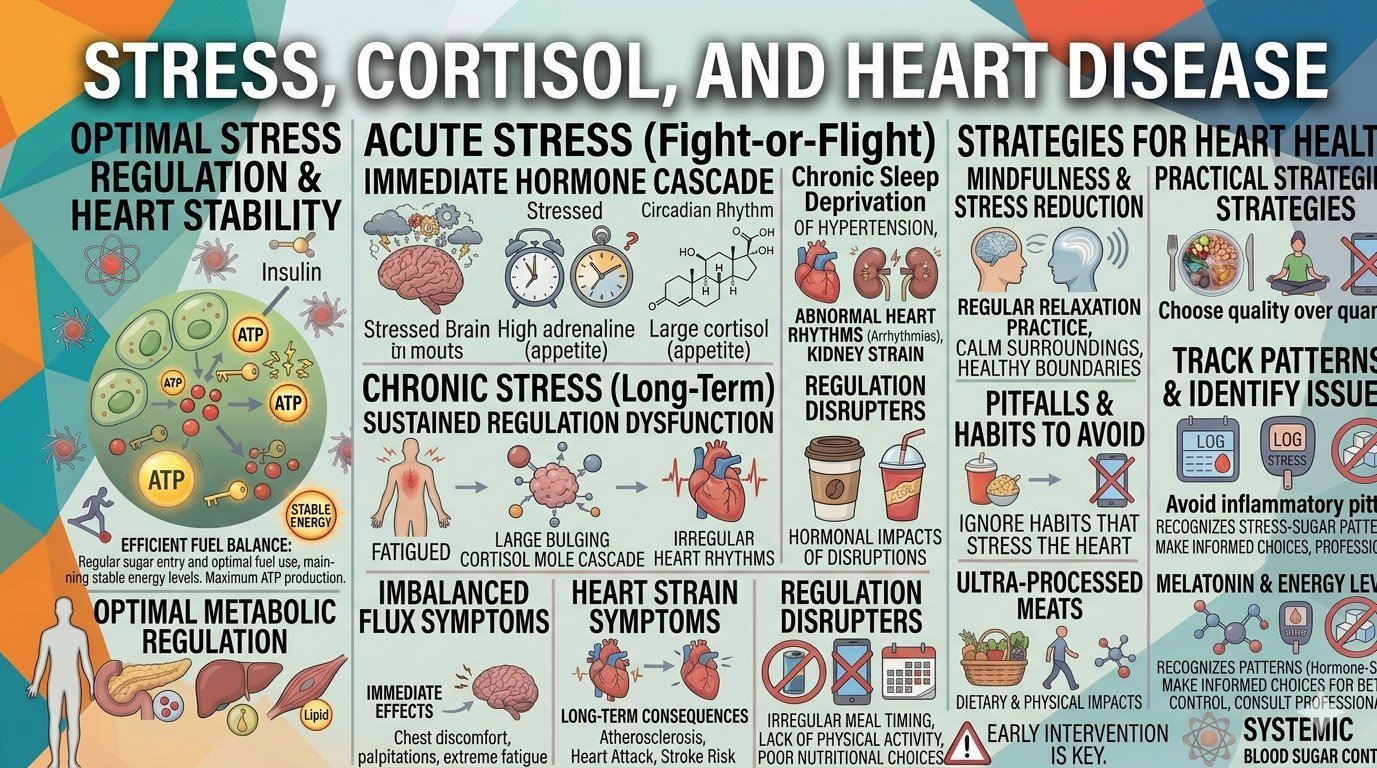
Key Factors That Increase Cortisol and Stress Burden
Stress is not caused by a single factor. It often results from cumulative physiological and lifestyle pressures.
Common contributors include:
- Chronic psychological stress
- Poor sleep
- Overwork or irregular schedules
- High caffeine intake
- Poor diet quality
- Blood sugar instability
- Physical inactivity
- Chronic illness
- Inflammation
- Social or financial stress
Many of these factors are strongly influenced by lifestyle patterns addressed in Nutrition, Metabolism, and Sleep Health.
Cardiovascular Conditions Linked to Chronic Stress and Cortisol
Long-term stress and elevated cortisol are associated with multiple cardiovascular diseases.
Hypertension (High Blood Pressure)
Chronic stress contributes to sustained elevation in blood pressure through hormonal and nervous system activation.
Over time, this can lead to:
- Persistent hypertension
- Arterial damage
- Increased stroke risk
- Increased heart attack risk
Coronary Artery Disease
Chronic stress increases the risk of plaque buildup in coronary arteries through inflammation, insulin resistance, and vascular damage.
This risk is amplified when combined with:
- Poor diet
- Sedentary lifestyle
- Obesity
- Poor sleep
These pathways connect directly to metabolic processes discussed in Metabolism and Weight Loss.
Heart Attack (Myocardial Infarction)
Sudden intense stress can trigger acute cardiovascular events.
Mechanisms include:
- Increased blood clotting
- Elevated blood pressure
- Increased heart rate
- Reduced oxygen supply to the heart
This phenomenon is sometimes called:
Stress-triggered cardiac events
Stroke
Stress increases stroke risk through:
- Elevated blood pressure
- Vascular inflammation
- Blood vessel damage
- Increased clotting tendency
Both chronic stress and acute emotional stress events have been associated with increased stroke risk.
Heart Rhythm Disorders (Arrhythmias)
Chronic stress and elevated cortisol can disrupt the electrical stability of the heart.
Risk factors include:
- Increased sympathetic nervous system activity
- Hormonal imbalance
- Sleep disruption
- Inflammation
Arrhythmias are often influenced by stress patterns discussed in Energy & Fatigue and Sleep Health.
Practical Strategies to Reduce Cortisol and Protect Heart Health
Managing stress is not about eliminating stress entirely — it is about improving the body’s resilience and recovery capacity.
1) Improve Sleep Quality and Consistency
Sleep is one of the most powerful regulators of cortisol.
Helpful strategies include:
- Maintaining consistent sleep times
- Reducing evening light exposure
- Limiting caffeine late in the day
- Creating a dark, quiet sleep environment
Healthy sleep supports cardiovascular recovery and aligns with principles discussed in Sleep Health.
2) Stabilize Blood Sugar
Blood sugar fluctuations can increase cortisol release.
Helpful habits include:
- Eating balanced meals with protein and fiber
- Avoiding long fasting periods when stressed
- Limiting ultra-processed foods
- Maintaining regular meal timing
These strategies support metabolic stability addressed in Blood Sugar and Metabolism.
3) Engage in Regular Physical Activity
Exercise helps regulate cortisol and improve cardiovascular function.
Benefits include:
- Reduced stress hormone levels
- Improved blood pressure regulation
- Better insulin sensitivity
- Reduced inflammation
Even moderate physical activity can significantly improve heart health.
This connection reinforces the role of movement in Heart Health and Weight Loss.
4) Support Stress Regulation Through Nutrition
Diet plays a direct role in hormone regulation and inflammation.
Helpful nutrients include:
Dietary patterns that support metabolic health are addressed in Nutrition and Gut Health.
5) Practice Stress Recovery Techniques
Stress recovery is as important as stress exposure.
Evidence-based strategies include:
- Deep breathing
- Mindfulness meditation
- Time in nature
- Social connection
- Structured relaxation
These practices help regulate the nervous system and improve hormonal balance.
Why Stress and Cortisol Matter for Long-Term Heart Health
Stress is not only a psychological experience — it is a physiological state that directly affects the cardiovascular system.
Over time, chronic stress and elevated cortisol can lead to:
- High blood pressure
- Insulin resistance
- Chronic inflammation
- Weight gain
- Sleep disruption
- Cardiovascular disease
These changes accumulate gradually and often remain unnoticed until disease develops.
Because stress influences Hormone Health, Metabolism, Blood Sugar, and Heart Health, managing stress is a foundational component of long-term cardiovascular protection.
Final Thoughts
Stress and cortisol are essential survival mechanisms, but when stress becomes chronic, the same systems designed to protect the body can begin to damage the heart.
Chronic stress increases inflammation, disrupts metabolism, impairs sleep, and elevates blood pressure — all of which increase cardiovascular risk over time.
Protecting heart health requires an integrated approach that includes:
- Stress regulation
- Healthy sleep
- Stable metabolism
- Balanced nutrition
- Hormonal resilience
The heart does not function in isolation. It responds continuously to signals from the brain, hormones, metabolism, and lifestyle — making stress management a central pillar of long-term cardiovascular health.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Medical Institutions
American Heart Association (AHA)
National Institutes of Health (NIH)
Mayo Clinic — Stress and Heart Disease
Cleveland Clinic — Cortisol and Stress
Global Organizations
World Health Organization (WHO) — Cardiovascular Disease and Stress
Peer-Reviewed Studies
Steptoe A, Kivimäki M
Stress and cardiovascular disease
Nature Reviews Cardiology
Chandola T et al.
Work stress and coronary heart disease
European Heart Journal
Hackett RA, Steptoe A
Psychosocial stress and hypertension
Hypertension
Scientific Review
Russell G, Lightman S
The human stress response
Nature Reviews Endocrinology
