
Stress: The Hidden Driver of Modern Mental and Physical Disease
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
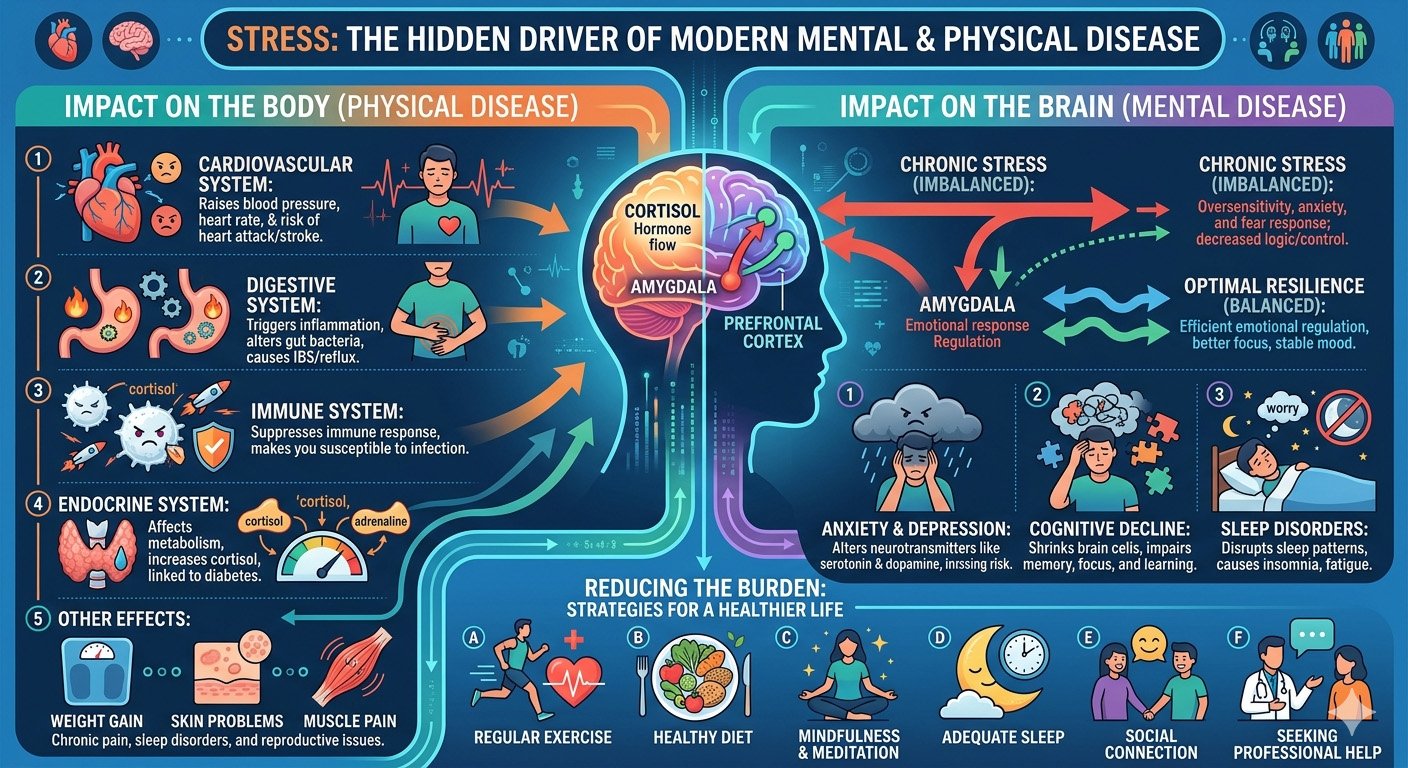
Stress is often perceived as a temporary emotional reaction to difficult situations. In reality, it is a powerful biological force capable of reshaping brain function, altering immune responses, disrupting metabolic balance, and accelerating the development of chronic disease. In the modern world, stress has become one of the most pervasive yet underestimated drivers of both mental and physical illness.
Unlike acute threats faced by earlier human societies, modern stress is frequently psychological, persistent, and cumulative. Financial pressure, information overload, sleep disruption, social instability, and chronic uncertainty create a continuous state of physiological activation. The body responds as if danger is present—even when no immediate threat exists. Over time, this prolonged activation transforms stress from a survival mechanism into a disease mechanism.
Today, stress is increasingly recognized as a central factor in conditions ranging from anxiety and depression to cardiovascular disease, metabolic disorders, immune dysfunction, and cognitive decline. It is not simply a symptom of modern life—it is a biological process capable of driving disease across multiple systems simultaneously.
The Biology of Stress: A Survival System Turned Chronic
Stress begins in the brain, specifically in regions responsible for threat detection and emotional processing. When the brain perceives danger, the hypothalamus activates the hypothalamic-pituitary-adrenal (HPA) axis, initiating a cascade of hormonal responses designed to prepare the body for action.
This response includes the release of:
- Cortisol
- Adrenaline
- Noradrenaline
- Glucose into the bloodstream
- Inflammatory signaling molecules
In short bursts, this system is protective. It increases alertness, sharpens focus, and mobilizes energy. However, when stress becomes chronic, the same biological mechanisms begin to damage tissues, dysregulate hormones, and weaken the body’s regulatory systems.
Chronic activation of the stress response leads to:
- Persistent inflammation
- Elevated blood pressure
- Insulin resistance
- Immune suppression
- Neurotransmitter imbalance
- Hormonal disruption
The body is designed to recover after stress. Modern life often prevents that recovery.
Chronic Stress and the Brain: Structural and Functional Changes
Long-term stress does not merely affect mood—it physically alters the brain.
Neuroscientific research shows that chronic stress can change the structure and connectivity of key brain regions involved in emotion, memory, and decision-making.
Affected brain regions include:
Amygdala
Responsible for detecting threats and generating fear responses. Chronic stress increases its activity and sensitivity, making individuals more reactive to perceived danger.
Hippocampus
Essential for memory formation and emotional regulation. Prolonged exposure to cortisol can reduce hippocampal volume and impair memory.
Prefrontal Cortex
Responsible for planning, impulse control, and rational decision-making. Chronic stress weakens its regulatory function, reducing emotional control and increasing impulsivity.
These changes help explain why prolonged stress is associated with:
- Anxiety disorders
- Depression
- Irritability
- Difficulty concentrating
- Emotional instability
- Reduced cognitive performance
Stress, therefore, is not only an emotional experience—it is a neurological condition when sustained over time.
Stress and the Immune System: From Protection to Vulnerability
The immune system is highly sensitive to stress hormones. In the short term, stress can enhance immune activity. In the long term, it suppresses immune defenses and increases inflammation.
This paradox is known as immune dysregulation.
Chronic stress contributes to:
- Increased susceptibility to infections
- Slower wound healing
- Chronic inflammation
- Autoimmune activation
- Increased risk of inflammatory disease
Inflammation plays a central role in many modern illnesses, including:
- Cardiovascular disease
- Diabetes
- Neurodegenerative disorders
- Depression
- Cancer progression
Stress acts as a biological amplifier of inflammation, turning temporary immune responses into persistent physiological damage.
Cardiovascular Disease: The Heart Under Constant Pressure
The cardiovascular system is one of the most directly affected by chronic stress.
Stress hormones increase heart rate and blood pressure, constrict blood vessels, and promote inflammatory processes that damage arterial walls. Over time, these effects accelerate the development of cardiovascular disease.
Chronic stress is associated with:
- Hypertension
- Atherosclerosis
- Heart attacks
- Stroke
- Heart rhythm disturbances
Stress also influences behavior in ways that indirectly increase cardiovascular risk.
Common stress-related behaviors include:
- Poor diet
- Physical inactivity
- Smoking
- Excess alcohol consumption
- Sleep disruption
These behavioral patterns compound the biological effects of stress, creating a powerful cycle of risk.
Metabolic Health: Stress and the Rise of Modern Chronic Disease
Stress plays a critical role in metabolic disorders, particularly obesity and type 2 diabetes.
Cortisol increases glucose production and promotes fat storage, especially in the abdominal region. This pattern of fat accumulation is strongly associated with metabolic syndrome.
Chronic stress contributes to:
- Insulin resistance
- Increased appetite
- Cravings for high-calorie foods
- Weight gain
- Fat accumulation around organs
- Elevated blood sugar levels
This metabolic disruption is one of the reasons stress is considered a hidden driver of modern chronic disease.
Stress, Sleep, and the Breakdown of Recovery
Sleep is the body’s primary recovery mechanism. Stress disrupts sleep, and poor sleep increases stress, creating a self-reinforcing cycle.
Stress interferes with:
- Falling asleep
- Staying asleep
- Deep sleep cycles
- REM sleep
- Circadian rhythm stability
Sleep deprivation, in turn, increases cortisol levels and reduces emotional regulation.
This cycle leads to:
- Fatigue
- Mood instability
- Reduced cognitive performance
- Increased anxiety
- Reduced resilience to stress
Over time, the body remains in a state of chronic activation without sufficient recovery.
Mental Health Disorders and Chronic Stress
Chronic stress is one of the strongest predictors of mental health disorders.
It is closely associated with:
- Anxiety disorders
- Depression
- Burnout
- Panic disorder
- Post-traumatic stress disorder (PTSD)
- Substance use disorders
Stress affects neurotransmitters such as serotonin, dopamine, and norepinephrine—chemicals essential for mood regulation and emotional stability.
When stress persists, these systems become dysregulated, increasing vulnerability to mental illness.
In many cases, stress is not merely a trigger—it is a sustaining force that maintains psychological symptoms over time.
Stress and Aging: Accelerating Biological Wear and Tear
Chronic stress accelerates biological aging through a process known as allostatic load—the cumulative burden of repeated stress on the body.
This process affects:
- Cellular repair mechanisms
- DNA stability
- Immune function
- Hormonal regulation
- Brain health
Stress is associated with:
- Shortened telomeres
- Increased oxidative stress
- Reduced tissue regeneration
- Earlier onset of chronic disease
In effect, chronic stress increases the speed at which the body wears down.
Modern Stress: Why It Is Different From the Past
Human physiology evolved to handle short bursts of physical danger. Modern stress is fundamentally different.
Key characteristics of modern stress include:
- Psychological rather than physical threats
- Continuous exposure to information
- Financial and occupational pressure
- Social comparison and digital overload
- Irregular sleep patterns
- Sedentary lifestyles
Unlike acute stress, modern stress often has no clear endpoint. The nervous system remains activated for extended periods, preventing recovery.
This shift has transformed stress into one of the defining health challenges of the 21st century.
Signs That Stress Is Affecting Health
Stress-related health problems often develop gradually and may go unnoticed until symptoms become severe.
Common warning signs include:
Physical signs:
- Persistent fatigue
- Headaches
- Muscle tension
- Digestive problems
- Elevated blood pressure
- Frequent illness
Emotional signs:
- Irritability
- Anxiety
- Mood swings
- Difficulty concentrating
- Feeling overwhelmed
Behavioral signs:
- Sleep disruption
- Increased caffeine or alcohol use
- Emotional eating
- Social withdrawal
- Reduced productivity
Recognizing these signs early is critical for preventing long-term health consequences.
The Core Insight: Stress Is a System-Wide Disease Driver
Stress is not confined to the mind. It affects every major biological system—neurological, cardiovascular, metabolic, immune, and endocrine. It alters behavior, disrupts recovery, and accelerates disease processes across the body.
In modern health science, stress is increasingly viewed as a foundational risk factor—similar to poor diet, physical inactivity, and smoking. Its effects are cumulative, systemic, and often invisible until damage has already begun.
Managing stress is not simply about relaxation. It is about protecting the body’s regulatory systems, preserving mental resilience, and preventing the progression of chronic disease.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
American Psychological Association (APA) – Stress Effects on the Body
https://www.apa.org/topics/stress/body
National Institute of Mental Health (NIMH) – 5 Things You Should Know About Stress
https://www.nimh.nih.gov/health/publications/stress
Centers for Disease Control and Prevention (CDC) – Stress and Coping
https://www.cdc.gov/mentalhealth/stress-coping
World Health Organization (WHO) – Stress
https://www.who.int/news-room/questions-and-answers/item/stress
Harvard Health Publishing – Understanding the Stress Response
https://www.health.harvard.edu/staying-healthy/understanding-the-stress-response
Mayo Clinic – Chronic Stress
https://www.mayoclinic.org/healthy-lifestyle/stress-management/in-depth/stress/art-20046037
