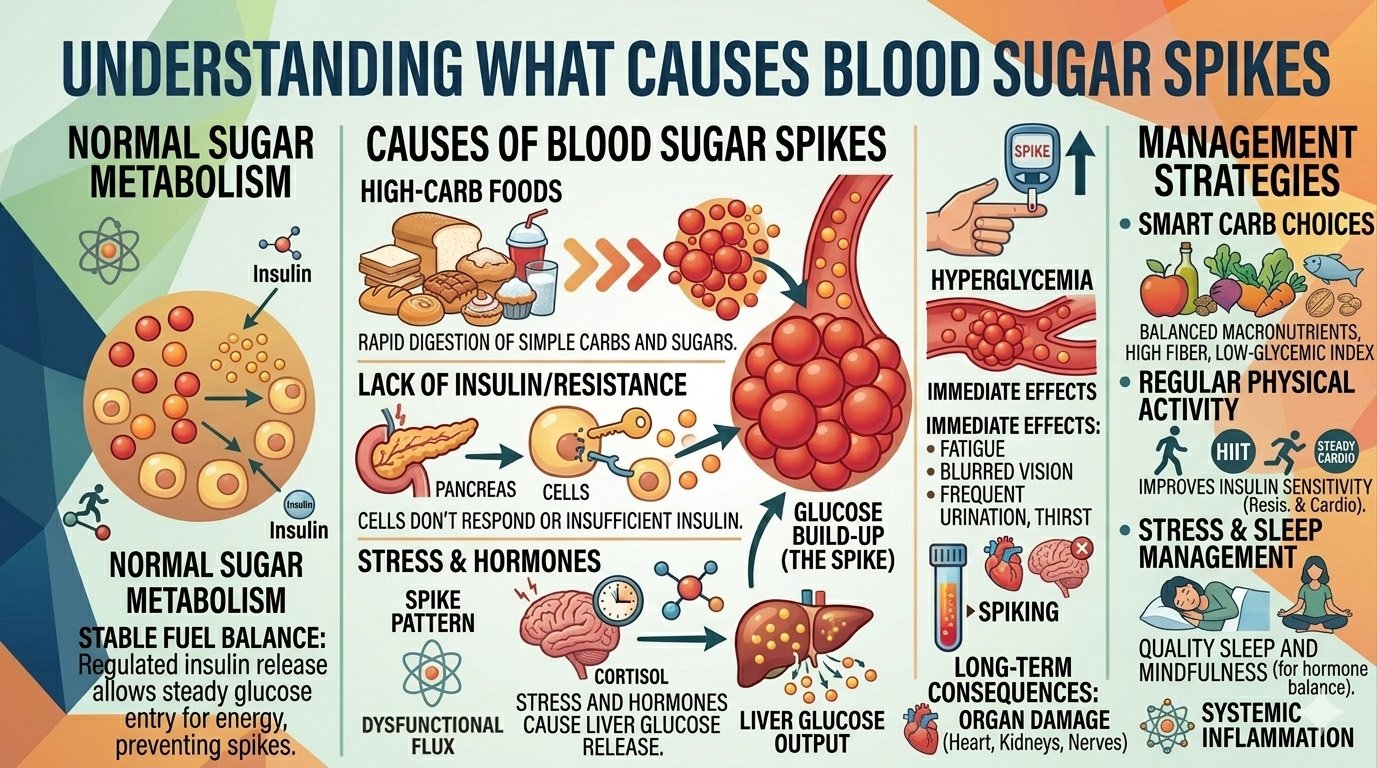
What Causes Blood Sugar Spikes
VitaCoreBalance Editorial Team | Research-based health content • Editorial review process | March 2026
Introduction
Blood sugar spikes are a common metabolic event that can affect energy levels, appetite, mood, and long-term health. While occasional fluctuations are normal, frequent or extreme spikes may signal deeper issues within the body’s metabolic and hormonal systems.
Blood glucose regulation is not controlled by a single organ. It involves coordinated interactions between the pancreas, liver, muscles, hormones, digestive processes, and daily lifestyle habits. This is why understanding blood sugar spikes requires a broader view of metabolic regulation, nutrition, and hormone balance rather than focusing only on sugar intake itself.
Many people experience blood sugar spikes without realizing it. Symptoms such as fatigue after meals, sugar cravings, irritability, or brain fog can all be linked to unstable glucose levels. Over time, repeated spikes may contribute to insulin resistance, weight gain, cardiovascular risk, and metabolic disorders.
To better understand prevention and management, it is essential to explore the real causes behind blood sugar spikes and how different body systems influence glucose stability.
Relevant systems connected to blood sugar regulation include:
- Metabolism
- Nutrition
- Hormone Health
- Gut Health
- Sleep Health
- Energy & Fatigue
- Weight Loss
- Heart Health
What Is a Blood Sugar Spike?
A blood sugar spike, also known as postprandial hyperglycemia, occurs when glucose levels rise rapidly after eating. This rise is a normal physiological response, but problems arise when the increase is excessive, prolonged, or occurs frequently.
In healthy individuals:
- Blood sugar rises after meals
- Insulin is released to move glucose into cells
- Blood sugar returns to normal within about 2–3 hours
When regulation is impaired, glucose remains elevated for longer periods, placing stress on metabolic and cardiovascular systems.
Blood sugar spikes can occur in:
- People with diabetes
- Individuals with prediabetes
- Those with insulin resistance
- People without diagnosed metabolic disease
This makes glucose stability a central topic within Blood Sugar regulation and overall Metabolism health.
How Blood Sugar Regulation Works
Blood sugar control depends primarily on the hormone insulin, which is produced by the pancreas.
The process follows a predictable physiological sequence:
- Food is digested into glucose
- Glucose enters the bloodstream
- The pancreas releases insulin
- Cells absorb glucose for energy
- Blood sugar returns to baseline
Several organs play key roles:
Pancreas
Produces insulin and glucagon.
Liver
Stores glucose as glycogen and releases it between meals.
Muscles
Use glucose for movement and physical activity.
Adipose tissue (body fat)
Stores excess energy.
Hormonal signals, nutrient intake, physical activity, sleep quality, and stress levels all influence how efficiently this system functions. Disruptions in any of these areas can lead to unstable blood sugar.
For example, poor sleep can reduce insulin sensitivity, while chronic stress can increase glucose production through hormonal pathways linked to Hormone Health and Sleep Health.
Key Causes of Blood Sugar Spikes
Blood sugar spikes are rarely caused by a single factor. Most cases involve a combination of dietary, hormonal, metabolic, and behavioral influences.
1) High Intake of Refined Carbohydrates
Refined carbohydrates are one of the most direct triggers of rapid glucose increases.
These foods are quickly digested and absorbed, causing sharp rises in blood sugar.
Common examples:
- Sugary drinks
- White bread
- Pastries
- Candy
- Sweetened cereals
- Processed snacks
These foods typically lack fiber, protein, and fat, which normally slow glucose absorption.
Dietary patterns dominated by refined carbohydrates are strongly associated with:
- Insulin resistance
- Weight gain
- Type 2 diabetes risk
- Metabolic syndrome
Balanced Nutrition that includes fiber, protein, and healthy fats can significantly reduce post-meal glucose spikes.
2) Large Portion Sizes
Even healthy foods can cause blood sugar spikes when consumed in large quantities.
This is especially true for:
- Rice
- Pasta
- Potatoes
- Fruit juices
- High-carbohydrate meals
The total carbohydrate load matters just as much as food quality.
Large meals can overwhelm insulin response capacity, particularly in people with reduced insulin sensitivity. Portion control plays a central role in both Weight Loss and blood sugar regulation.
3) Low Fiber Intake
Fiber slows digestion and reduces the speed at which glucose enters the bloodstream.
Low-fiber diets are strongly associated with:
- Faster glucose absorption
- Higher post-meal blood sugar
- Increased hunger
- Reduced metabolic stability
High-fiber foods include:
- Vegetables
- Legumes
- Whole grains
- Nuts
- Seeds
Fiber also supports beneficial gut bacteria, linking blood sugar control directly to Gut Health.
4) Insulin Resistance
Insulin resistance is one of the most important drivers of blood sugar spikes.
In this condition:
- Cells respond poorly to insulin
- Glucose remains in the bloodstream
- The pancreas produces more insulin
- Blood sugar becomes harder to control
Risk factors include:
- Excess body fat
- Physical inactivity
- Poor diet
- Chronic stress
- Sleep deprivation
- Hormonal imbalance
Insulin resistance is a core metabolic issue closely connected to Metabolism, Hormone Health, and long-term Heart Health risk.

5) Poor Sleep
Sleep is a powerful regulator of blood sugar.
Even one night of inadequate sleep can:
- Reduce insulin sensitivity
- Increase hunger hormones
- Raise cortisol levels
- Increase blood glucose
Chronic sleep deprivation is associated with:
- Higher diabetes risk
- Weight gain
- Increased appetite
- Fatigue
- Metabolic dysfunction
This is why sleep quality is a central component of Sleep Health and overall metabolic stability.
6) Chronic Stress
Stress activates the body’s fight-or-flight response.
This response increases the release of:
- Cortisol
- Adrenaline
- Glucagon
These hormones signal the liver to release glucose into the bloodstream, even when food has not been consumed.
Over time, chronic stress can lead to:
- Persistent blood sugar elevation
- Insulin resistance
- Increased abdominal fat
- Energy instability
Stress-related glucose changes are closely linked to Hormone Health and Energy & Fatigue regulation.
7) Physical Inactivity
Muscle tissue plays a major role in glucose utilization.
During physical activity:
- Muscles absorb glucose from the bloodstream
- Insulin sensitivity improves
- Blood sugar stabilizes
Sedentary behavior reduces glucose uptake and increases insulin resistance risk.
Even short daily movement sessions can significantly improve glucose regulation and support healthy Metabolism.
8) Hormonal Imbalances
Hormones strongly influence blood sugar regulation.
Important hormones include:
- Insulin
- Cortisol
- Growth hormone
- Thyroid hormones
- Estrogen
- Progesterone
Hormonal changes can occur during:
- Menopause
- Thyroid disorders
- Chronic stress
- Polycystic ovary syndrome (PCOS)
- Aging
Hormonal disruptions often lead to changes in glucose control, appetite, and body composition, highlighting the connection between Hormone Health and blood sugar stability.
Conditions Associated With Frequent Blood Sugar Spikes
Repeated blood sugar spikes may indicate underlying metabolic dysfunction.
Common related conditions include:
- Prediabetes
- Type 2 diabetes
- Metabolic syndrome
- Insulin resistance
- Polycystic ovary syndrome (PCOS)
- Obesity
- Nonalcoholic fatty liver disease
- Cardiovascular disease
These conditions are closely linked to long-term Heart Health, Weight Loss, and metabolic regulation.
Practical Strategies to Reduce Blood Sugar Spikes
Evidence-based strategies can significantly improve glucose stability.
Focus on Balanced Meals
Include:
- Protein
- Fiber
- Healthy fats
- Whole foods
This combination slows digestion and stabilizes blood sugar.
Increase Physical Activity
Even moderate activity improves insulin sensitivity.
Examples:
- Walking after meals
- Resistance training
- Daily movement routines
Physical activity is one of the most effective tools for improving Metabolism and preventing glucose spikes.
Improve Sleep Consistency
Aim for:
7–9 hours of sleep per night
Consistent sleep schedules support:
- Hormonal balance
- Insulin sensitivity
- Appetite regulation
- Energy stability
Sleep regulation is essential for both Sleep Health and blood sugar control.
Reduce Refined Sugar Intake
Prioritize:
- Whole foods
- Fiber-rich carbohydrates
- Protein-based snacks
- Balanced meals
Dietary quality is one of the strongest predictors of stable blood sugar and sustainable Weight Loss.
Manage Stress
Helpful strategies include:
- Regular physical activity
- Relaxation techniques
- Time outdoors
- Consistent daily routines
Stress regulation supports both Hormone Health and metabolic stability.
Why Blood Sugar Spikes Matter for Long-Term Health
Frequent blood sugar spikes are not just a short-term issue. Over time, they can contribute to:
- Insulin resistance
- Chronic inflammation
- Fat accumulation
- Cardiovascular disease
- Reduced energy levels
- Hormonal imbalance
- Metabolic dysfunction
Stable blood sugar supports:
- Energy regulation
- Cognitive performance
- Appetite control
- Weight management
- Cardiovascular health
- Longevity
This makes glucose regulation one of the central pillars of overall health.
Final Thoughts
Blood sugar spikes are influenced by far more than sugar intake alone. They reflect the interaction between diet, hormones, sleep, stress, physical activity, and metabolic health.
Understanding these connections allows individuals to make informed decisions that support long-term health rather than focusing on isolated symptoms.
Blood sugar stability is deeply connected to:
- Metabolism
- Nutrition
- Hormone Health
- Sleep Health
- Gut Health
- Energy & Fatigue
- Weight Loss
- Heart Health
Addressing these systems together provides the most effective path toward sustainable metabolic health and disease prevention.
Medical Disclaimer
This content is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional.
Editorial Transparency
This article was created following evidence-based health content guidelines and reviewed by the VitaCoreBalance Editorial Team.
Sources
Centers for Disease Control and Prevention (CDC)
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
World Health Organization (WHO)
JAMA Internal Medicine
Polonsky KS et al.
Pathogenesis of Type 2 Diabetes Mellitus
The Lancet
Postprandial Hyperglycemia and Cardiovascular Risk
Diabetes Care Journal
